By: Esther Nakkazi
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
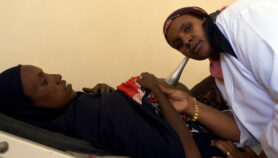
[KAMPALA] Early initiation of antiretroviral therapy (ART) for adults infected with HIV in rural Sub-Saharan Africa can generate widespread economic benefits, researchers have found.
In a study presented today at the XIX International AIDS Conference in Washington DC, United States, researchers from Uganda and the US found that HIV-infected adults with high CD4+ counts — a health status benchmark for HIV–positive people — are able to work on average 30 per cent more hours each day than people with low CD4+ counts.
Furthermore, their children’s school enrolment rates were 15 per cent higher than those of children with parents showing low CD4+ counts.
CD4+ counts are a measure of immune system strength. Normal CD4 blood levels are 500-1200 per microlitre. When infected with HIV, the body’s CD4 count begins to fall, and when levels reach 350 cells per microlitre, it is recommended that the person begins ART treatment. When a CD4 count reaches less than 200 cells per microlitre, the person is said to have developed AIDS.
This new study is part of a wider project called the Sustainable East Africa Research in Community Health (SEARCH) Collaboration, run by the University of California, San Francisco, the San Francisco General Hospital and Trauma Center, and Makerere University in Kampala, Uganda.
Although the effect of treatment on some socio-economic indicators has been assessed before, this study represents the first population-level research into how socio-economic indicators differ among persons at various stages of HIV infection, and how rapidly people lose their ability to work.
It is based on a strategy known as ‘test and treat’ that combines universal testing (regular testing for all people in countries with high HIV prevalence), improved access to care, and early ART treatment.
Early HIV treatment, given long before people start to become ill or develop AIDS symptoms, keeps individuals relatively healthy. It also keeps transmission rates within communities lower, as — due to their suppressed or undetectable HIV viral loads — the infectiousness of HIV-positive people is reduced, the researchers say.
"When treatment is delayed, even if it is not yet [showing] full blown AIDS, the body is disturbed by opportunistic infections and is weakened," said Hakim Sendagire, a microbiology lecturer at the Makerere University College of Health Sciences. "Therefore early treatment would enable people to have healthier bodies and to work for longer periods of time and fend for their families."
Through its guidelines, the World Health Organisation (WHO) has already endorsed early treatment for people with a 250 to 350 CD4+ count, especially for pregnant women.
Joseph Matovu, a behavioural change expert at the School of Public Health Makerere University, told SciDev.Net that people needed to be educated to see the benefits of early treatment, but that adherence would need to be emphasised so that any side effects are minimised.
"Although the study’s recommendations are good in terms of prevention, they could cause further resistance to drugs because people might not adhere [to treatment programmes] if they are not actually showing signs of HIV-related illness," Matovu said.