Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
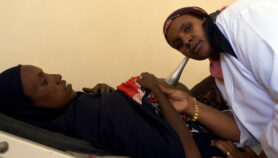
[SANTIAGO] A tool to monitor how HIV-positive patients respond to antiretroviral therapy (ART) could free up scarce personnel and laboratory resources in developing countries, according to an international team of researchers.
HIV destroys immune system cells, including a type of white blood cell known as CD4. The World Health Organisation recommends that ideally, ART is provided once the number of CD4 cells falls below 350 per microlitre of blood, and in all instances after the count falls below 200. Once ART is begun, patients should receive regular CD4 tests to monitor how their immune system is reacting.
But the tests require specialised equipment and personnel, and difficulties in providing these in poor countries have been identified as a factor in a lack of provision of ART. In 2010, less than half the 15 million people in developing countries in need of ART were receiving it.
The researchers sought to establish whether it might be possible to ‘triage’ people on ART and prioritise CD4 tests for patients in the greatest need.They applied a ‘prediction-based classification’ (PBC) tool to nearly 2,000 blood samples from people undertaking courses of ART in seven clinics in several countries including Argentina, Malaysia and South Africa.
They wanted to ascertain whether the tool would reduce the need to monitor CD4 cells constantly. Instead, they took a CD4 count at the start of ART and after that, cheaper white blood cell tests were used to predict when CD4 counts would fall below 200 cells per microlitre of blood.
When tested retrospectively on the blood samples, the PBC tool correctly classified 90 per cent of samples in which CD4 counts had fallen below 200.
Writing in the April issue of PLoS Medicine, the researchers say using the PBC tool could eliminate up to 54 per cent of CD4 tests, potentially lowering costs and freeing up resources.
"Introducing PBC will diminish the burden on poorly resourced laboratories, releasing funding to reach more patients," Ian Sanne, a co-author of the study from South Africa’s University of Witwatersrand, told SciDev.Net.
Luis Montaner, senior author of the study and director of the HIV-1 Immunopathogenesis Laboratory at the United States-based Wistar Institute, said further studies would be needed to improve the method’s predictive accuracy and demonstrate the feasibility and cost-effectiveness of the approach over long periods of time in the field.
Victor DeGruttola, professor of statistics at the Harvard School of Public Health, who was not involved with the study, told SciDev.Net: "This study demonstrates how a fairly straightforward statistical tool — PBC — can help make the cost of monitoring HIV-infected patients who receive ART therapy modest … whilst providing quality care."
References
PLoS Medicine doi:10.1371/journal.pmed.1001207 (2012)