By: Maryke Steffens
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Vaccines for non-infectious illness could help developing nations tackle the growing burden of chronic disease. Maryke Steffens reports.
HIV/AIDS has had glitzy rock stars like Bob Geldof and Bono campaigning for action. Malaria got the slightly less glitzy British prime minister Gordon Brown. These two diseases certainly wreck lives, killing children and adults, rich and poor. But they’re now being overshadowed by a deadlier health threat. Non-communicable diseases of old age and poor lifestyles, such as heart disease, cancer and diabetes, are the biggest killers in the developing world.
Now, some researchers think vaccines could be part of the solution — not to avoid these diseases, but to treat their effects.
A growing problem
Chronic, non-communicable diseases are responsible for almost 60 per cent of all deaths annually worldwide, with half of these from cardiovascular disease.
"It’s a myth that cardiovascular disease is only seen in rich countries", says Liam Smeeth, from the non-communicable diseases epidemiology group at the UK-based London School of Hygiene and Tropical Medicine.
Smeeth recently completed a study looking for high blood pressure — a predictor of stroke and heart attacks — in over 800 civil servants in Ghana, and found disturbing trends. Over a third were at increased risk of heart disease he says, compared with an average of ten per cent in rural parts of West Africa.
Two-thirds of the estimated 177 million people affected by diabetes — mostly type 2 diabetes — live in the developing world. Currently, over half of new cancer cases occur in people living in the developing world. This is set to increase to 70 per cent by 2020 as deaths from infectious diseases fall, letting people live longer. "Cardiovascular disease and cancers are essentially diseases of older people," points out Smeeth.
Longer life, double trouble
The rise in chronic diseases in developing nations comes down to several factors, not least lifestyle changes associated with rising wealth: more smoking and alcohol, less physical activity and eating more fat, salt and refined sugar.

The rise in chronic diseases is down to factors such as eating more fat, salt and refined sugar
Flickr/Mr DoeyBags
Smeeth studied civil servants because they’re relatively well off for Ghana and have taken on a ‘western lifestyle’ at quite an early stage of the country’s development. They’re like a ‘sentinel group’ for those who will be taking on that kind of lifestyle in the coming years, he says.
The drop in deaths from infectious diseases has also played a role, Smeeth adds.
"The proportion of over 65s in developing countries is very tiny at the moment, about three or four per cent, but that’s scheduled to rise to about ten per cent by 2030," says Max Parkin, a cancer epidemiologist with the UK’s Oxford University. "That will have quite a profound impact on the number of cancer cases and indeed other non-communicable diseases that are common in the elderly. "
This rise in chronic diseases has created a unique dilemma for developing countries, as Bobby John, a physician and president of the nongovernmental organisation Global Health Advocates in Pune, India, points out.
"India is a classic case where you have a stunning rise in diabetes, heart disease, and tobacco-related diseases, but you also find a persistence of infectious diseases. We are facing a twin problem, and that’s something that countries like India need to grapple with," he says.
Chronic diseases also require a different approach, focussing on continuity of care, monitoring and long-term follow-up. The health systems of emerging economies don’t have the experience or capacity to manage this, says John.
"Communicable disease control has been mostly vaccine-based. You do one immunisation and you’re done with that person. "
A new approach
Certainly, vaccines have long been a mainstay in the arsenal against infectious diseases. But recently there have been murmurs about a new type of vaccine, designed for non-infectious diseases. These therapeutic vaccines still use the immune system to attack the disease, but, as the name suggests, they’re designed to treat rather than prevent illness.
The idea isn’t as outlandish as it may sound. In 1999, the US-based Institute of Medicine ranked chronic illnesses such as type one diabetes and melanoma as promising vaccine candidates, labelling the development of these vaccines a matter of public health urgency.
Biotechnology companies took the hint, and since then, several vaccines targeting cancers, cardiovascular disease and hypertension have made it to phase I and II clinical trials.


Vaccines have long been a mainstay in the arsenal against infectious diseases
Flickr/Nick Atkins Photography
Two companies, Switzerland-based Cytos and UK-based Protherics, are testing hypertension vaccines in phase II trials. The vaccine is designed to prompt the immune system to produce antibodies against the hormone angiotensin, which constricts blood vessels and raises blood pressure.
"If you can avoid pills, you avoid the compliance issues around current high blood pressure medication," says Andrew Heath, chief executive officer of Protherics.
He says the vaccine will need to be administered once or twice a year, adding "That’s important, especially for the developing world. If you’ve got to give a shot once a month, it isn’t practical, ".
A vaccine against atherosclerosis — the build-up of fatty plaques of cholesterol on artery walls, which can lead to heart attack or stroke — is in phase I trials. Developed by Swedish company Bioinvent, in conjunction with US company Genentech, the vaccine is made up of the human antibody BI-204 that, when injected in the body, is designed to recognise a type of cholesterol (low-density lipoprotein, or LDL) that forms plaques as foreign and attack it. The company hopes the vaccine will prevent heart attacks in patients with acute coronary artery disease.
These heart disease vaccines are still in the early stages of development. But there are already two vaccines against cancer-causing viruses, says Oxford University’s Max Parkin: the hepatitis B vaccine, which protects against liver cancer, and the human papillomavirus vaccine, which protects against cervical cancer.
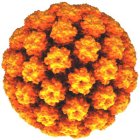


The human papillomavirus
Flickr/AJC1
"The hep B vaccine has been around for 20-odd years, " he says. "Theoretically, if all newborn babies were vaccinated against hepatitis B, that would eliminate a large proportion of liver cancer in the world."
Biotechnology companies are hoping to emulate these successes with vaccines against cancers with non-infectious causes. Pharmaceutical company Merck is running a phase III trial of a vaccine for non-small cell lung cancers (the commonest group of lung cancers), set to finish in 2010. The vaccine is designed to induce an immune reaction to a molecule (MUC1) on the outside of cancerous cells. The 1,300 patients participating are spread across the world, including people in developing countries Brazil, China, India and Mexico. This wide-ranging recruitment reflects the global problem of lung cancer.
UK-based research company Onyvax has a vaccine for prostate cancer in phase II trials, involving about 80 patients. "Our objective is to keep the patients symptom free and turn the condition from something life-threatening into more of a chronic condition," says Anthony Walker, chief executive officer of Onyvax.
The vaccine is made up of whole, inactive prostate cancer cells that, when injected into the body, should trigger an immune response to the prostate cancer, hopefully prolonging life expectancy. Walker says the product requires several more years at least until it is ready for market, but that he expects that market to include the developing world.
"There’s no difference between a cancer vaccine and any other cancer therapy. If advanced cancer therapies are being marketed in developing countries, so would a vaccine," he says.
Competing costs
The question remains, of course, whether someone with a chronic disease in the developing world would have access to these therapies. In many places, particularly low-income countries, the answer is a resounding no.
"Infectious disease is where the money is right now. Non-infectious diseases don’t have any money," says Bobby John.
"In India, the health minister has been making noises about tobacco-related morbidity and mortality, but it hasn’t translated into policy. We know that we will be stuck with one of the largest proportions of diabetes [patients] in the world, but do we have planning for that? No — because we’re still grappling with infectious diseases."
John says part of the problem is that chronic diseases aren’t as glamorous or emotive as communicable diseases. "Even now when you see someone with diabetes or hypertension, the judgement is ‘you ate your way into it’ or ‘you lived your life into it’. That’s pretty much the public health mindset when it comes to non-communicable diseases."



Chronic diseases aren’t as glamorous or emotive as communicable diseases, says John
Flickr/A. Currell
The difficulty in introducing the vaccine against cervical cancer in developing countries highlights some of the hurdles to come. "Everybody’s trying to figure out how best to set about using this vaccine. Cost is going to be a big problem, as it’s extremely expensive at the moment," says Max Parkin.
Prohibitive costs mean that neither the hepatitis B nor the papillomavirus vaccine are widely used across the developing world.
But Smeeth says history shows that costs can be overcome. "Take the example of antiretrovirals for HIV. The problem was that the poorer countries couldn’t afford them. But what has been successful is putting pressure on the pharmaceutical companies to make these drugs available in an affordable way to people who need them."
Capacity comes first
Although the promise of a ‘magic bullet’ for chronic diseases is enticing, John emphasises that the development of national health systems must go hand in hand with any new technology. Health systems like India’s must adapt to managing long-term illnesses and accessing a completely new patient group, he says.
"An early life vaccine could be integrated into the early infancy vaccine programmes. But if it’s something that has to be applied later in life, we currently don’t have a national health scheme to pull that person in."
John believes the Indian pharmaceutical industry could play a role in delivering affordable technology like vaccines to the developing world, but that it needs to embrace innovation, rather than just producing generic drugs.
"If you’re talking about costs of healthcare, the solutions are right here and the market is here to justify those investments, " he says.
But he also says both the developed and the developing world must keep the promise that therapeutic vaccines hold in perspective.
"HIV is a classic case where the wait for a vaccine has proved quite long and in the meantime, things that ought to have been done were not done or were shelved because the promise was, ‘It’s coming!’ …and that [risk] has to be balanced out."
Maryke Steffens is a freelance science and health journalist.
This article is part of a Spotlight on Tackling chronic diseases.













