By: Priya Shetty
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Priya Shetty explains the links between climate change and insect-borne disease, and outlines priorities for developing country policymakers.
Some researchers have called climate change the biggest health threat the world has ever faced. With good reason — it is now an unavoidable truth that the health of the planet is linked to the health of its people.
As the world heats up, ecosystems are visibly struggling to cope with the rapid ecological changes. Global warming has already triggered weather changes — from flooding and storms to heatwaves and drought — that are taking a heavy toll on people's health around the world.
In high-level meetings, developed and developing country governments are busy battling over emission targets. Meanwhile, the world's poor, who bear the biggest disease burdens, can expect soaring rates of ill health.
This increase will come partly from shifting population dynamics, as people flee flooded coasts or searing deserts for more habitable areas. A rise in diseases carried by insects, such as mosquitoes or ticks, could be a key factor. Climate influences these 'vectors' in many ways — from controlling the length of their life cycle to influencing breeding conditions.
Scientists broadly agree that climate change will affect insect-borne diseases, but the exact consequences remain uncertain. Whether warmer, wetter conditions make it easier for vectors such as mosquitoes to multiply and spread disease will depend on a much broader range of ecological and societal factors than just rainfall or temperature.
We urgently need to build our understandingof how climate change will affect health, especially through insect-borne disease. And we must strengthen health systems to deal with the expected changes.
The warming planet
Climate scientists say a rise of up to two degrees Celsius more than pre-industrial global temperatures could be manageable, with people only in specific, vulnerable regions suffering catastrophic environmental effects. Any larger temperature increase puts the whole planet's population at risk.
But sticking to this limit seems impossible. The Intergovernmental Panel on Climate Change predicts that if emissions continue to rise unchecked — they are already 38 per cent higher than in 1990 — the world could warm by as much as four degrees Celsius by 2100 (see Figure 1). [1]
Some of the damage has already been done. The rise in greenhouse gas emissions over the past few decades has already warmed the planet by 0.8 degrees Celsius. The lag between growing emissions and the corresponding increase in temperature means that we can expect at least another 0.6-degree Celsius global temperature rise over the next few decades.
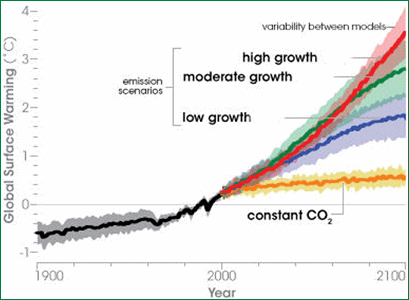
Figure 1: Global warming predictions based on different emission scenarios [2]
Credit: IPCC
And how much we must cut emissions remains unresolved. The G8 meeting of world leaders in July 2009 called for a 50 per cent cut in emissions by 2050. Earlier, in January, the World Economic Forum's Global Agenda Council on Climate Change, in Davos, was more ambitious. It called for a cut of 80 per cent by 2050.
Harmful health effects
Initial concerns about climate change in the early 1990s focused on environmental impacts and all but ignored links with health. But this imbalance is slowly changing as research emerges on the likely effects climate change will have on people's health and the spread of disease.
This year, for example, The Global Humanitarian Forum (GHF) published a report estimating that 315,000 people die due to climate change every year, and they predict this will rise to half a million by the year 2030. [3] While such estimates of direct deaths remain low relative to the size of the global population, about 310 million people are expected to have suffered ill health because of climate change by 2030.
Nine out of ten of these people will be in developing countries and the number of healthy years of life lost to environmental change, including climate change, is set to be 500 times higher in Africa than Europe (see Figure 2).
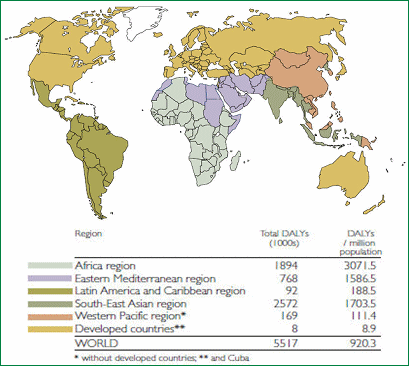


Figure 2: Estimated effects of climate change on health through number of Disability Adjusted Life Years (DALYs) — the sum of years of potential life lost due to premature death, and the years of productive life lost due to disability, associated with climate change [4]
Credit: WHO
Developing countries already bear the brunt of the global disease burden. Their populations are more likely to be undernourished, lack access to clean water and contract infectious diseases such as malaria. They are also dealing with a growing epidemic of chronic diseases such as diabetes and cancer.
Climate could worsen the problems in many ways. Changing rainfall patterns and sea level rises mean some areas will become drought-prone while others are flooded. Both situations have dire consequences for access to clean water. This, in turn, means a likely spread of waterborne diseases such as cholera and diarrhoea, which alone kills nearly two million children a year.
Increasing hunger and malnutrition are expected as increasingly common extreme weather events destroy crops, patterns of crop pest infestation change, and salt infiltrates flooded coastal areas. [5]
Heatwaves can kill thousands — in August 2003, Europe's summer was about 3.5 degrees Celsius above average and an estimated 45,000 people died over two weeks.
Climate change will also worsen air pollution. Both temperature and humidity influence how air pollutants and fine particulates form, and evidence suggests that fine particulates contribute to respiratory disease (such as pneumonia, asthma and chronic obstructive pulmonary disease), especially in children. [1] The WHO estimates that 800,000 people alreadydie each year because of outdoor air pollution.
Virulent vectors
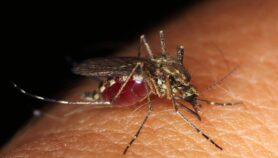
One area of particular concern is how climate change will affect the spread of insect-borne diseases. These include dengue fever, malaria, Lyme disease, West Nile virus, Rift Valley fever, chikungunya and yellow fever. They are spread through the bite of 'vectors' such as mosquitoes, ticks and flies.
Researchers currently focus much of their attention on dengue fever and malaria, partly because the diseases are so prevalent but also because outbreaks seem linked to climate. Increased rainfall in normally dry areas, for example, can create stagnant pools of water where mosquitoes breed.
But the links between climate and insect-borne disease are far from simple (see Table 1 for potential interactions). The same rainfall increase in wet regions could reduce malaria by washing immature mosquitoes away. Changes in temperature can also have opposing effects, depending on where they occur.
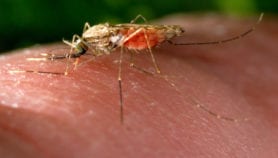
Generally speaking, the malaria mosquito digests blood quicker and feeds more often in warmer weather, thus speeding up transmission. The parasite meanwhile completes its life cycle more quickly, increasing replication. In theory then, global warming might allow these vectors to spread into areas they weren't previously able to colonise.
By 2080, up to 320 million more people could be affected by malaria because of these new transmission zones. [6] Worryingly, the disease would then also be spreading to people whose immune systems may never have been exposed to malaria, and who may be more vulnerable as a result.
But increased temperatures in already hot regions could reduce the spread of malaria mosquitoes by pushing temperatures higher than the mosquitoes can survive. Most mosquitoes cannot survive above about 40 degrees Celsius, so regions where climate change pushes temperatures above this level could see a drop in malaria. This is starting to be seen in Senegal, for example, where malaria prevalence has dropped by more than 60 per cent in the past 30 years. [7]
And an increase in the population of vectors does not automatically translate into an increase in disease.
The dynamics of malaria transmission, for example, depend on both the human population's immunity and the parasite's levels of drug resistance. Other ecological and societal factors are equally important: water storage and disposal systems, agricultural practices, deforestation, population density, living conditions, control programmes and health infrastructure all play a role in determining the reach and spread of malaria.
|
Climate factor
|
Potential effects on vector
|
Potential effects on pathogen
|
|
Increased temperature |
|
|
|
Decreased rainfall |
|
|
|
Increased rainfall |
|
|
|
Sea-level rise |
|
|
Table 1: The effect of climate change on insect-borne disease recorded in research studies. [1]
These complexities mean that while on the surface climate seems linked to malaria transmission, scientists disagree about specific local impacts. For instance, in East Africa, a drop in mosquito control and a rise in drug resistance appears to be confounding studies assessing whether malaria incidence has grown because of, or independently of, climate. [1]
Similarly, studies arguing that climate change is extending malaria's latitudinal or altitudinal boundaries may not consider historical records that show malaria has previously existed in such places before global temperatures began to increase (see The malaria myths of climate change).
The complexities of dengue transmission also lead studies to report conflicting associations between climate variations and infection rates. The clearest links come from small countries such as Honduras and Nicaragua, where the number and spread of the dengue mosquito population has been well correlated with climate. [8]Links in larger countries like Brazil and China have not been significant — although this may be because climate data was country-wide rather than location-specific.
Nevertheless, some scientists estimate that by 2080, six billion people will be at risk of dengue, compared with 3.5 if the climate does not change. If the global population grows to about 10 or 11 billion by then, as some estimates suggest, over half the planet could be at risk.
The spread of other vector-borne diseases could also increase. The cholera bacteria Vibrio cholerae can live on some species of plankton. Warmer sea temperatures mean more plankton blooms, which could mean the cholera bacteria flourishes, spreading to populations on the warm coasts of countries such as Bangladesh.
Schistosomiasis, a parasitic disease transmitted by aquatic snails, also seems to be affected by climate. In China, the latitudinal threshold beyond which temperatures were too cold for the snail to live has moved northwards, putting nearly 21 million more people at risk of the disease.
Strategic policies
Although scientists have yet to agree how far climate change will make insect-borne disease rise, there is an emerging consensus on how to tackle a potential crisis. Developing accurate models and surveillance to predict or detect disease outbreaks and act as early warning systems is central to this.
Such systems will require both climate and disease data, and lots of it, if they are to be rigorous enough to be reliable (see Better surveillance key to malaria early warning systems).
In the past, the paucity of surveillance systems has meant developing countries have lacked up-to-date information on diseases. One outcome of the threat of SARS and bird flu H5N1, and the current pandemic of swine flu A(H1N1), is that many countries have been shocked into action. Several, including China and India, are pledging to update their disease-monitoring systems.
But this is a challenging undertaking. These systems require advanced computer hardware and software to collate and analyse incoming data. Such technology might include, for example, geographic information systems that can link data to specific locations and allow both spatial and temporal analyses of disease data. The infrastructure of existing systems may need to be upgraded to accommodate these additions.
But monitoring disease is just one aspect of creating an early-warning system. Accuracy will also rely on researchers understanding how non-climatic factors, such as drug resistance, influence epidemics.
And early warning systems will only work if there are resources to respond to the alarm bells. Strengthening health systems in poor countries, a long-called-for necessity, is even more urgent in the face of these future challenges. Moreover, the medical staff within these must be fully aware of how climate is likely to affect the people they treat.
A WHO feasibility analysis for creating prediction systems calls for health policymakers' involvement at the earliest stages, because even the best early warning systems will be worth little if operational responsibilities aren't clearly delineated and agreed from the beginning. [9]
Earlier this year, The Lancet medical journal commissioned the University College London Institute for Global Health to draw up a policy response framework on climate change and disease. [5] Their recommendations for policies on vector-borne disease are summarised in Box 1.
|
Box 1: Priorities for policymakers
Information
Poverty/equity
Technology
Sociopolitics
Institutions
|
And finally, pouring valuable resources into adapting to climate change is only worthwhile if countries also make serious attempts to mitigate global warming. Ultimately, this means a commitment from all countries to reduce greenhouse gas emissions and move to a low-carbon economy.
Priya Shetty is a freelance science writer on health and the environment, based in New York.
References
[1] Intergovernmental Panel on Climate Change. Climate change 2007: Contribution of Working Group II to the Fourth Assessment Report of the Intergovernmental Panel on Climate Change. M.L. Parry, O.F. Canziani, J.P. Palutikof, P.J. van der Linden and C.E. Hanson, Eds. Cambridge University Press (2007)
[2] Predicting future warming NASA (2007)
[3] Global Humanitarian Forum The anatomy of a silent crisis ![]()
![]()
![]()
[4] WHO Climate change and human health: Risks and responses (2003)
[5] Costello, A., Abbas, M., Allen A. et al Managing the health effects of climate change The Lancet 373 1693-1733 (2009)
[6] Lindsay S. W. and Martens W. J. M. Malaria in the African highlands: Past, present and future ![]()
![]()
[7] Githeko, A. K., Lindsay, S. W., Confalonieri, U. E. et al Climate change and vector-borne diseases: A regional analysis ![]()
![]()
![]()
[8] Patz, J. A., Campbell-Lendrum, D., Holloway, T. et al Impact of regional climate change on human health Nature 438 310-317 (2005)
[9] Kuhn, K., Campbell-Lendrum, D., Haines, A. et al Using climate to predict infectious disease epidemics WHO (2005)