By: Sam Otieno
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[NAIROBI] Cost-effective interventions are needed in low- and middle-income countries (LMICs) to reduce death burden caused by non-communicable diseases (NCDs), a study recommends.
According to researchers, inadequate evaluation of how lifestyle-related diseases are addressed in LMICs motivated them to conduct the study.
Cancer, diabetes and other lifestyle-related diseases kill more people in developing countries than in high-income Western countries at every age, the study says.
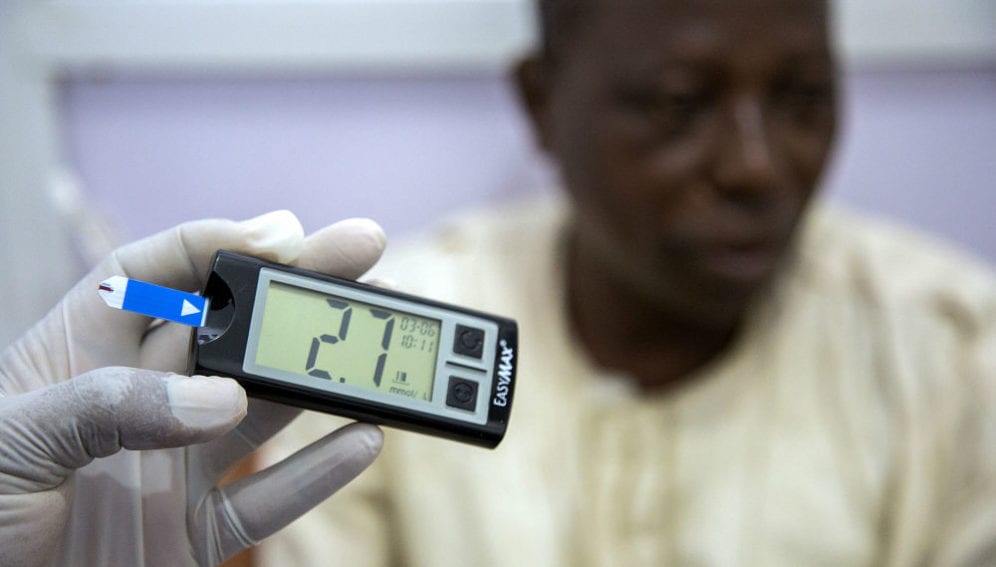
Cases of diabetes, cancer and heart disease have risen dramatically in developing countries in recent years as people eat more meat and have increasingly sedentary lifestyles, according to health experts.
“It is also important that donors, who have overlooked NCDs in their development financing, realise that the poor are most affected.”
Majid Ezzati, Imperial College London
“Of the about 25 million deaths in the four tropical regions — Africa, India (South Asia), Southeast Asia, Latin America and the Caribbean — in 2016, almost 9 million (34 per cent) were from infectious and parasitic diseases, maternal and perinatal conditions, and nutritional deficiencies; and 14 million (55 per cent) from NCDs,” says the study, which was published in the 25 July issue of Nature.
Majid Ezzati, lead author of the study and the chair of the global environmental health group at the UK-based Imperial College London, attributes the leading causes of NCDs in tropical LMICs to poor nutrition and living environment, infections, insufficient regulation of tobacco and alcohol, and inaccessible healthcare.
The study, which included 2016 WHO mortality data from 46 tropical LMICs, identified the five African countries with highest death rates for NCDs per 100,000 as Burkina Faso, Cote d'Ivoire, Mali, Sierra Leone and Togo while those with the lowest death rates were Congo, Ethiopia, Gabon, Kenya and Tanzania.
The introduction of health insurance and other essential health interventions in some African countries might have led to the differences in death rates among the countries, Ezzati suggests, without naming the countries.

African countries in the study that had the highest age-standardised death rates and those that had the lowest age-standardised death rates for NCDs
Ezzati explains that African countries need to fund and implement cost-effective interventions that can prevent lifestyle-related diseases such as hypertension, cervical cancer, diabetes and stroke.
“It is also important that donors, who have overlooked lifestyle-related diseases in their development financing, realise that the poor are most affected and that they should be a priority alongside issues such as HIV,” he says.
The study recommends interventions to promote better environment, nutrition and health behaviours, including a need to reduce salt in processed foods.
Jennifer Mabuka, programme manager, Human Hereditary and Health in Africa, a programme being implemented by the Alliance for Accelerating Excellence in Science in Africa, tells SciDev.Net that for some time now the African continent is experiencing an epidemiological shift – the change from infectious diseases to chronic diseases as public health improves.
“I think the more we highlight the issues the more people in the right offices will pay attention. Generally we tend to work in silos, and that is wrong,” explains Mabuka.
“I believe that we can’t really anticipate what the NCD epidemic will look like in a few years on the continent because it’s happening in the context of communicable diseases, which isn’t true for the West. It’s going to be different and difficult to deal with.”Mabuka calls on African governments, health officials and religious leaders to spearhead prevention efforts against lifestyle-related diseases, and to help conduct extensive research to tackle the menace.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.
References
Majid Ezzati and others Acting on non-communicable diseases in low- and middle-income tropical countries (Nature,25 July 2018)