By: Claire Marris
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Claims about the benefits of a biotech project to make artemisinin are overblown, says Claire Marris.
In April, a consortium led by the global health NGO PATH — and comprising the University of California, Berkeley, synthetic biology company Amyris and pharmaceutical firm Sanofi — announced the first industrial production of ‘semi-synthetic artemisinin’.
The consortium called this “a pivotal milestone in the fight against malaria” and “a triumph for synthetic biology”. [1,2] The project has certainly helped to brand synthetic biology as a revolutionary new field of science that could “heal us, heat and feed us” [3] — but the extent to which it will deliver benefits to people in countries burdened with malaria is debatable.
The role of interlinked technological, economic, social and political factors has been overlooked, at least in public communication about the project.
Grand claims
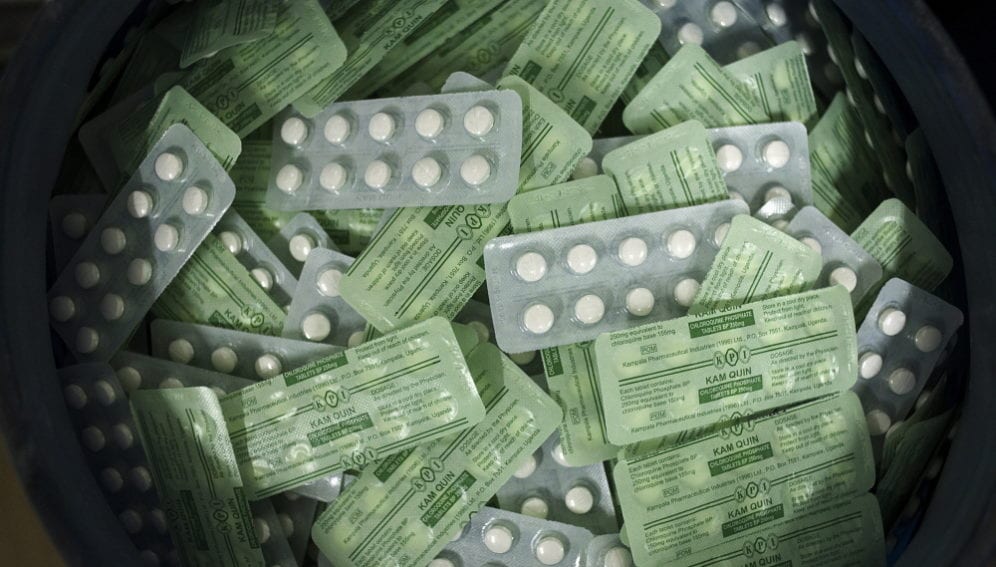
Since 2003, artemisinin-based combination therapies (ACTs) have been the WHO’s recommended treatment for malaria, with artemisinin being extracted from the plant Artemisia annua. But in 2006, scientists succeeded in creating a yeast strain that produces a precursor to artemisinin called artemisinic acid.
This was undoubtedly a scientific feat, but early on the scientists involved also made grand claims about the societal benefits of this research, which they portrayed as “a biotechnology solution to the global problem of access to affordable antimalarial drugs”. [4]
It has taken seven years to convert the initial laboratory success into the production of commercially significant quantities of artemisinin, due to the ordinary technological challenges of industrial scaling-up.
In the meantime, I have, as a sociologist working in this area, attended numerous talks that have used this project as a stupendous illustration of what synthetic biology can achieve — complete with slides portraying African children, menacing-looking mosquitoes and stark numbers for malaria cases and deaths.
The clear implication is that the prowess and idealism of synthetic biologists will — or indeed already has — saved hundreds of thousands of poor people from this devastating disease.
This use of this project to garner support for synthetic biology is troubling.
Market matters
The project’s fundamental premise has been that producing artemisinin through biotechnology would be cheaper than extracting it from plants. However, Sanofi has announced that the price of its semi-synthetic artemisinin will be similar to the agricultural product (US$350-400 per kilogram).
“Far from helping to promote the field, the use of the Artemisinin Project as a poster child could end up tarnishing the image of synthetic biology if the outcomes turn out to be less than triumphant.”
Claire Marris, King's College London
This is despite Sanofi selling it on a ‘no-profit, no-loss’ basis, more than US$50 million research and development funding for the project from the Bill & Melinda Gates Foundation, and not having to pay royalties to Amyris and Berkeley, which hold patents on the technology.
Over time, the project leaders have put forward an additional aim: rather than replacing plant-derived artemisinin, the semi-synthetic form would provide an additional source, helping to stabilise a market price that has fluctuated from year to year just like other agricultural products.
This rationale has been used to explain why Sanofi has chosen to produce only 60 tonnes a year, one-third of global demand. It was also a good way to counter arguments from critics such as the advocacy NGO ETC group, which stressed how biotechnologically derived artemisinin could harm Artemisia farmers’ livelihoods.
Meanwhile, Jay Keasling, the project’s lead scientist, has said that it is possible to cheaply produce the entire global supply through biotechnology by making the industrial process more efficient, and that this is necessary to control supplies and eradicate the use of artemisinin as a single therapy (which could trigger resistance). [5, 6] Regardless of the validity — or not — of this position, such public statements are, in the current situation, likely to further destabilise an already highly uncertain market.
Limited influence
The reality is that semi-synthetic artemisinin is simply another source of a compound already used in malarial therapies. Sufficient global supplies can be produced by farmers and, in fact, this year a surplus of plant-derived artemisinin is expected.
Since the new form is not cheaper than the existing source, nor alleviating a shortage, it will — at best — play a relatively small part among the multitude of factors that determine whether or not people suffer and die from malaria.
For example, the local price of ACTs is largely determined by donor strategies rather than the price pharmaceutical companies charge. In addition, Oxfam argues that easier access to cheaper ACTs, when not accompanied by adequate diagnosis and supervision, will fail to bring increased health benefits and is a “dangerous distraction” from better strategies such as investing in community health. [7] Health is more than a medical matter that can be ‘fixed’ by new technology.
When I have put such considerations to scientists and others who glorify the project, they have argued that these are outside their remit and sphere of expertise. Fair enough, perhaps. But if they do not want to take responsibility for the real-world complexities of what happens beyond the confines of the laboratory, they should take care not to make simplistic claims about the project’s global health benefits.
I do not wish to dispute the humanitarian motivation of those involved. But synthetic biologists and their supporters have latched on to this project because they believe they need a success story to demonstrate the societal benefits of the field in order to counter what they perceive — wrongly — as the public’s general opposition to genetic modification (GM). [8]
This fails to recognise that the current controversy around GM crops developed partly as a result of similar, overblown promises, made in the late 1990s, about their prospects for ‘feeding the poor’ that proved out of step with what was actually delivered.
Far from helping to promote the field, the use of the Artemisinin Project as a poster child could end up tarnishing the image of synthetic biology if the outcomes turn out to be less than triumphant.
Some of the first synthetic biology products on the market are cosmetics containing compounds produced by the companies Amyris and Solazyme. Why don’t we hear more about those?
Claire Marris is senior research fellow in the Department of Social Science, Health and Medicine at King’s College London, United Kingdom, and in the Centre for Synthetic Biology and Innovation at Imperial College London. She can be contacted at [email protected]
References
[1] PATH Sanofi and PATH announce the launch of large-scale production of semisynthetic artemisinin against malaria (PATH, 11 April 2013)
[2] Sanders, R. Launch of antimalarial drug a triumph for UC Berkeley, synthetic biology (UC Berkeley News Center, 11 April 2013)
[3] Speech by the Chancellor of the Exchequer, Rt Hon George Osborne MP, to the Royal Society (Gov.uk, 2012)
[4] American Journal of Tropical Medicine and Hygiene 77 (supplement 6), 198 (2007)
[5] Peplow, M. Malaria drug made in yeast causes market ferment (Nature, 13 February 2013)
[6] Thomas, J. Synthetic anti-malarial compound is bad news for artemisia farmers (The Guardian, 2013)
[7] Dransfield, S. Put an end to risky malaria scheme, warns Oxfam (Oxfam, 24 October 2012)
[8] EMBO Reports 2 (7), 545 (2001)