By: Ines Nastali
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
The first vaccine candidate against Middle East respiratory syndrome (MERS) protects mice, camels and monkeys from the disease, paving the way for human trials later this year.
The so-called DNA vaccine has been developed in a collaboration led by the University of Pennsylvania, United States, and a paper on its success was published today in Science Translational Medicine.*
Conventional vaccines against viral diseases involve injecting a live virus or a foreign protein, called an antigen, both of which generate a protective immune response in the body.
The new vaccine instead works by injecting a DNA sequence that codes for a MERS antigen and relying on the patient’s body to make this protein. Lastly, the immune system reacts to the antigens by developing antibodies that defend against future infection.
Karuppiah Muthumani, a researcher at the University of Pennsylvania and one of the study’s two lead authors, says the DNA vaccine would be safer than conventional vaccines.
“Unlike attenuated vaccines, which are essentially weakened live viruses, there is no possibility through mutation for reversion into a live replicative virus,” says Muthumani.
“We have ways to take care of people and help them to recover more quickly but we don’t have specific vaccines and medicines, as yet.”
Rana Sidani, WHO
Just one single dose of vaccination protected eight rhesus monkeys used in the study from the MERS virus, the paper states. The same response was seen in three camels that were treated with the DNA vaccine.
According to David Weiner, another study author, who works with Muthumani at the University of Pennsylvania, two firms are preparing clinical trials. US business Inovio and Korean company GeneOne Life Science are scheduled to take the vaccine “into human safety and efficiency studies by the end of 2015”, he says.
MERS is prevalent across the Middle East and parts of Asia. The researchers say DNA vaccines are easier to create and use in developing countries than attenuated vaccines, as they need no refrigeration and do not need advanced laboratories for the production of antigens.
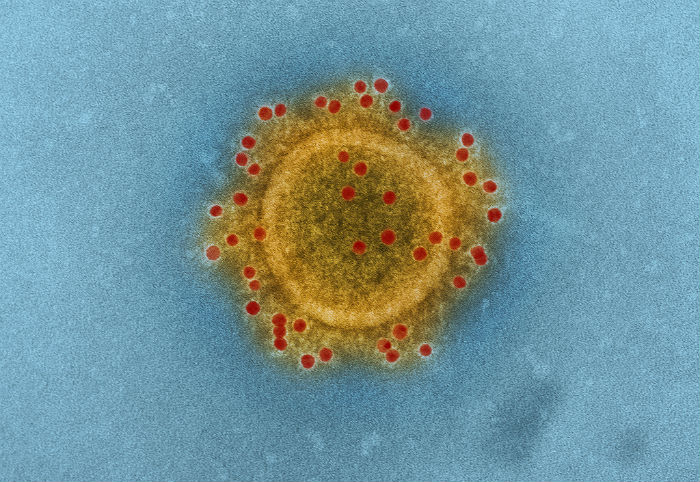
MERS was discovered in 2012 in Saudi Arabia. It causes fever, coughing and dangerous shortness of breath, which kills more than 30 per cent of those it infects. Since its first outbreak, MERS has claimed nearly 500 lives.
“I visited South Korea twice during this current outbreak,” says Weiner. “The infection created a great deal of stress and concern from health administrators as well as in the public.”
Rana Sidani, a spokeswoman for the World Health Organization’s Eastern Mediterranean office, says a vaccine is urgently needed as MERS is on the rampage in Saudi Arabia. Millions of Islamic pilgrims from all around the world visit the country each year.
Since the start of the year, 264 cases of MERS and 115 resulting deaths have been reported in Saudi Arabia.
“We have ways to take care of people and help them to recover more quickly but we don’t have specific vaccines and medicines, as yet,” Sidani says.
She would like to see more international collaboration on bringing the vaccine to market. “It will be very hard for any single country to take that on by itself,” she says.
* Article corrected on 21 August 2015. It originally said the research was published in Infectious Disease, but this refers to the research topic not a journal.
References
Karuppiah Muthumani and others A synthetic consensus anti-spike protein DNA vaccine induces protective immunity against Middle East respiratory syndrome coronavirus in nonhuman primates (Infectious Disease, 19 August 2015)