By: Priya Shetty
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Priya Shetty explores the truths and the myths about chronic diseases in the developing world.
The developing world is facing a deadly new health threat: chronic diseases. Illnesses such as cancer, diabetes and heart disease are quickly overtaking infections as the biggest killers of the world’s poor.
The numbers are disheartening. Around 80 per cent of people dying from chronic, non-communicable diseases live in the developing world. In 2002, the number of people dying from cancer worldwide (7.6 million) was greater than the 5.6 million dying from HIV/AIDS, malaria and tuberculosis combined.
The situation looks set to worsen. The incidence of cancer worldwide rose by 19 per cent between 1990 and 2000, mostly in developing countries. Between 1990 and 2020, the number of deaths worldwide from ischemic heart disease (arising from restrictions in the blood supply) is predicted to rise by 120 per cent for women and 137 per cent for men. Between 2000 and 2030, the number of people with diabetes will increase from 171 million to 366 million, 298 million of whom will be in poor countries.
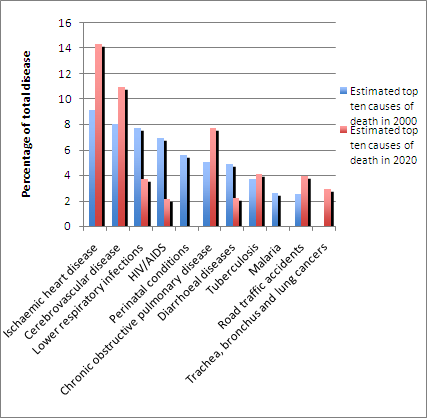
Changes in disease in developing countries
Source: International Journal of Epidemiology 34, 961-966 (2005)
.gif)
Diabetes prevalence (millions)
Source: adapted from International Journal for Equity in Health 4, 2 (2005)
All this threatens large dips in economic productivity, putting a phenomenal drain on countries’ economies. The WHO estimates that over the next decade, China is set to lose a massive US$558 billion, and India $237 billion, in national income as a result of diabetes, heart disease and stroke. These countries cannot afford not to tackle chronic diseases.
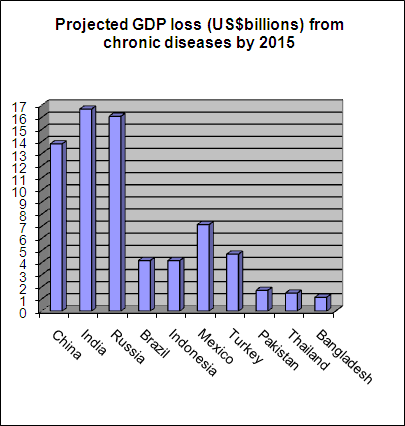


Economic loss from chronic diseases in developing countries
Source: adapted from The Lancet 370, 1929-38 (2007)
Links between diseases
Some infectious diseases co-exist — for example, people with HIV/AIDS are at a higher risk of tuberculosis because of their reduced immune resistance. Similarly, chronic diseases can be linked to other manifestations of poor health, either biologically or socially.
Mothers who are depressed, for example, are less likely to take proper care of their babies than mothers who are not depressed, potentially causing child health problems like poor nutrition and missed vaccinations.
Type 2 diabetes (non-insulin-dependent or adult-onset diabetes) is closely linked with obesity. About 90 per cent of cases are attributable to excess weight. Obesity, in turn, is linked to cardiovascular disease. Obese people are five times more likely to have high blood pressure than people of healthy weight.
Twin troubles
These trends hold a particular danger for the health systems of developing countries. Chronic non-communicable illnesses now kill a higher proportion of people than infectious diseases. However, infectious diseases still pose a considerable threat to the health of the world’s poor. In India, for example, 2.5 million children die from infections such as diarrhoea, malaria and pneumonia each year.
Health systems in developing countries, many of which are under-resourced and over-stretched, must now cope with this twin burden. But while the world’s aid system funnels millions every year towards tackling infectious diseases in poor countries, comparatively little is spent on chronic diseases.
There is currently no major donor initiative to tackle chronic diseases, unlike the situation for malaria or HIV/AIDS. Official Overseas Development Aid for health was $2.9 billion in 2002, of which 0.1 per cent was allocated to chronic diseases. The true figure might be marginally higher, since about 30 per cent of the money goes to basic health services, which would also tackle chronic diseases.
Much of the data available on rates of chronic diseases comes from the WHO, which is trying to build a clear picture of how such diseases are affecting different regions of the world. Knowing how disease trends are changing is important, but it is just as important to understand why they are changing.
Cause and effect
Many people still believe that illnesses like diabetes, obesity and heart disease only affect those in industrialised, and therefore wealthier, countries, where risk factors like eating fattier foods, getting less physical exercise, and smoking and drinking more are commonplace. But many developing countries are now seeing their own economies improve, with a corresponding change in behaviours.
Between 2000 and 2005, China’s gross domestic product (GDP) grew at an average rate of almost ten per cent and India’s at seven per cent, while average growth in other low-income and middle-income countries was five per cent. In high-income countries GDP grew at just two per cent in this period.
While Brazil, China and India are the three with the highest profiles, many other countries around the world are becoming richer too.
In 2002, raised blood pressure (an important risk factor for heart disease) was partly responsible for 15.8 per cent of deaths in the United States. But China, at 14.3 per cent, and Brazil, at 12.7 per cent, were not far behind.
The United States is thought to have the greatest problem of obesity — in 2002, 11.5 per cent of all deaths were because of a raised body-mass index. In Mexico, however, this percentage was 14.4, representing 639,400 years of lost life.
The WHO has created an online, searchable database of risk factors in 180 countries, focusing on key factors such as tobacco use, obesity and blood pressure.
But wealth and risks are not the only rising causes of chronic disease. In 2005, the percentage of people in developing countries aged 65 years or older was 5.5 per cent. This is set to reach 9.8 per cent in 2030 and 15 per cent by 2050 (see figure).
This shows that global efforts to solve the problem of infectious diseases are working and people are living longer — but with a deadly flipside. Put simply, people are living long enough for their rising risks to cause chronic disease.
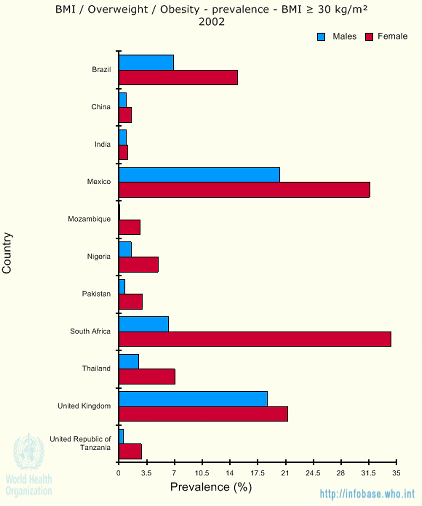


Obesity prevalence in 2002
Source: Infobase/WHO
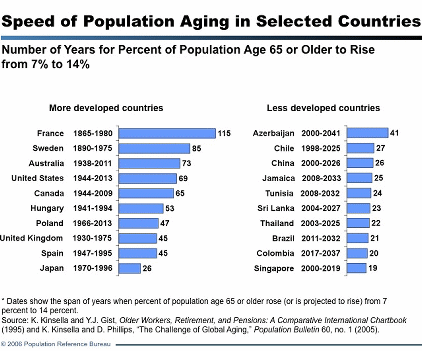


Speed of population ageing
Source: Population Reference Bureau (2006)
Cost-effective approaches
Any healthcare programme must compete with a hundred other funding priorities, and, in developing nations in particular, cost-effectiveness often determines whether a programme will be sustainable.
There are several low-cost ways to reduce the risk of chronic diseases. Reducing people’s salt intake by 15 per cent and implementing key elements of the WHO’s tobacco control framework (such as raising taxes on tobacco) could cost as little as US$0.14 per person per year in developing nations.
And multidrug regimens of a statin, aspirin, and two blood-pressure lowering drugs to tackle cardiovascular disease would cost US$0.43–0.90 per year in low-income countries and US$0.54–2.93 per year in middle-income countries, potentially saving 17.9 million lives over the next ten years.
The next step is to investigate how to expand these measures and increase public awareness in developing nations, so that people are willing to engage with such strategies.
Box: Top five myths about chronic diseases
Myth 1: We must deal with HIV/AIDS/TB/malaria first
Chronic diseases are starting to develop alongside infectious diseases and many people are dying of a combination of both. So healthcare systems need to deal with both types at the same time, especially as infectious diseases can become chronic.
Myth 2: Economic growth will automatically improve all health conditions
Development can improve health, but economic growth can also spur the growth of ‘lifestyle ‘ diseases such as diabetes.
Myth 3: Poor lifestyle choices cause chronic conditions, making them the responsibility of individuals
Social and cultural contexts influence individuals’ personal choices. Thus, governments, industry and others play an important role too.
Myth 4: Chronic conditions are problems of the rich and old
Low socio-economic status increases exposure to risk factors and decreases access to quality medical care. In developing countries, high-risk individuals are much younger than in developed nations.
Myth 5. Treating chronic conditions is too expensive for poor countries
Research indicates that some strategies, such as reducing salt intake, can be achieved for just a few cents per person per year.
Adapted from Myths About Chronic Diseases The Oxford Health Alliance with additional information from The Lancet chronic diseases supplement (December 2007).
This article is part of a Spotlight on Tackling chronic diseases.
References
Abdesslam, B.& Boutayeb, S. The burden of non-communicable diseases in developing countries. The International Journal of Equity in Health (2005).
Anderson, G. F. & Chu, E. Expanding priorities: confronting chronic disease in countries with low income. New England Journal of Medicine 356, 209–211 (2007).
Asaria, P., Chisholm, D., Mathers C., Ezzati M., Beaglehole R. Chronic disease prevention: health effects and financial costs of strategies to reduce salt intake and control tobacco use. The Lancet 370, 2044–53 (2007).
Bustelo, P. The economic rise of China and India and its implications for Spain. Real Instituto Eleano (2007).
Daar, A., Singer, P. A., Persad, D. L., et al. Grand challenges in chronic non-communicable diseases. Nature 450, 494–496 (2007).
Lingwood, R. J., Boyle, P., Milburn, A., Ngoma, T., Arbuthnott, J., McCaffrey, R., Kerr, S. H. & Kerr, D. J. The challenge of cancer control in Africa. Nature Reviews Cancer 8, 398–403 (2008).
Lim, S. L., Gaziano, T. A., Gakidou, E., Reddy, K. S., Farzadfar, F., Lozano, R. & Rodgers, A. Prevention of chronic disease in high-risk individuals in low-income and middle-income countries: health effects and costs. The Lancet 370, 2054–62 (2007).
Miranda, J. J. & Patel, V. Achieving the millennium development goals: does mental health play a role. PLoS Medicine 2, 0962–0965 (2005).
Parvez, H., Kawar, B. & El Nahas, M. Obesity and diabetes in the developing world: a growing challenge. New England Journal of Medicine 356, 213–215 (2007).
Population Division of the Department of Economic and Social Affairs of the United Nations Secretariat. World Population Prospects: the 2006 revision and World Urbanization Prospects: the 2005 revision.
Population Reference Bureau, Graphics Bank.
Yach, D., Hawkes C., Gould, C. L. & Hofman, K. J. The global burden of chronic diseases: overcoming impediments to prevention and control. Journal of the American Medical Association 291, 2616–22 (2004)
More on Capacity building


Script media release
Journalists offered ‘big break’ mentoring opportunity from Radio Nigeria
03/04/19