By: Amzath Fassassi
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
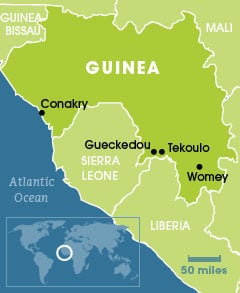
When Ebola broke out in Guinea in March local people were suspicious of the health workers who arrived to help. Those who accepted that the disease was real thought it had been imported by the humanitarian organisations operating in the area. As a result, there was much mistrust of Médecins Sans Frontières and the WHO. Mistrust turned to defiance, and led to many incidents between local people and the NGOs.
“Families hid their sick and, in certain villages, people resisted and prevented humanitarian organisations from doing their work,” Marc Poncin, a biologist with Médecins Sans Frontières, tells SciDev.Net.
“Contamination has therefore continued within communities, because control measures have not been put in place, and this has contributed to the fresh upsurge in the epidemic.”
Amadou Sall, scientific director of the Pasteur Institute in Dakar, Senegal, says that “one of the main problems has been cooperation of communities”.
He adds: “When populations do not cooperate and we cannot identify the sick or their contacts, the transmission chains continue and the teams responsible for monitoring the epidemic have no idea what’s going on.”
Anthropologists to the rescue
Faced with this situation, the international organisations working in Guinea have had to bring in anthropologists from the region and elsewhere to encourage the population to cooperate.
Sylvain Landry Faye, a health anthropologist from Cheikh Anta Diop University in Dakar, is one of the group of experts supporting front-line medical staff. Diseases such as Ebola are usually “considered to be a question for medical specialists”, he tells SciDev.Net. “Nevertheless, if disease is an absence of physical, psychological and social wellbeing, it becomes a question of humanity and of society, and anthropology has a fundamental role to play in this context.”
Faye adds that “doctors have always considered disease to be within a medical paradigm, by treating viruses, prions and sick bodies rather than individuals”. For Faye, illness “involves a society and a culture and, if we want we want to cure it, we must take account of these parameters”, hence the importance of the anthropologists, who specialise in such issues.
“If disease is an absence of physical, psychological and social wellbeing, it becomes a question of humanity and of society, and anthropology has a fundamental role to play in this context.”
Sylvain Landry Faye, Cheikh Anta Diop University
In the case of Guinea, Faye notes that, while the medical teams knew exactly what had to be done to help the population, the implementation of the response plan was hit by poor collaboration with communities. “The teams were beaten up and NGOs couldn’t get to the villages to implement the protocols,” he says.
But he says anthropologists can understand the culture of the area and help the medical teams adapt their practice to it. He notes that the transmission of the Ebola virus is not understood as a biological phenomenon in rural parts of the country where traditional beliefs — in particular sorcery — have the upper hand over science.
Onion-flavoured hot chocolate ‘cure’
The low literacy level in Guinea — around 25 per cent — and the inadequacy of information channels further hinder the fight against the epidemic. At one point text messages spread a rumour that a Guinean researcher based in Senegal had developed a cure for Ebola based on hot chocolate, milk, sugar and onions. This was enough for these products to run out in various shops around the country, including in Conakry, the capital.
The job of the anthropologists is to act as educators, mediators and facilitators with the population, to enable the response plan to be smoothly implemented.



“In the framework of the management of the Ebola epidemic, we’re talking about death, contamination, uncleanliness, funeral rites; we’re talking about people and society”, says Faye.
Anthropologists are considered a central part in the effort to combat the outbreak because, without their intervention, medical staff would struggle to do their jobs. “We have reached a situation in which people don’t want to hear what they’re being told,” explains Faye.
In such a difficult situation, the anthropologists make recommendations, aiming to find a balance between the fears and resistance of local people and the need to bring the epidemic under control. For example, they have recommended that medical staff stop using the term ‘isolation centres’ to refer to the places where people infected with Ebola are gathered, and instead to use the more reassuring term ‘treatment centres’.
According to Amadou Sall, of the Pasteur Institute in Dakar, “at one point, the treatment centres became synonymous with death chambers. People refused to go there, saying that, once you entered, you wouldn’t come out again alive” — a reference to the high mortality among victims of Ebola. A study published yesterday in the New England Journal of Medicine estimates that overall 71 per cent of people who get Ebola do not survive it — and that figure only drops to 64 per cent among those who are hospitalised.
Local beliefs
Faye also cites additional difficulties, linked to local beliefs. “In these societies, in which death is accompanied by a set of traditional rituals including the preparation of the corpse and the invocation of the spirits before burial, they don’t understand when we explain that they mustn’t touch the bodies of Ebola victims,” he says.
“From the point of view of their traditions, the corpse must be interrogated to discover the cause of death: whether the person died a natural death or died of ‘sorcery’. It is therefore necessary to touch the body.”
Yet given the virulence of the Ebola virus, the medical advice is to avoid touching the bodies of people who have died of the disease. Faye says: “We had to find a solution that enabled us to save what is essential: human lives. In this case, anthropologists had to engage communities in discussion to explain the medical risk that they were running [when touching the corpses].”
For him the question was: “At what price could we manage the social risk of not burying the body according to tradition?”
“We had to find a balance, which was to allow the populations to at least see the body and to throw objects into the body bag before the burial. That, at least, calmed their feelings and enabled us to avoid serial contamination of the population. That’s how the principle of secure burials was accepted.”
Exception to the rule
Another illustration of the difficulties the response teams faced in containing the epidemic was when, a few months ago, after the death of a pregnant woman, they ran into opposition from the population concerning the conditions of her burial.
Among the Kissi ethnic group of the nation’s southern forests, where the incident occurred, it is forbidden to bury a woman with a baby inside her. Instead, tradition requires that the foetus be extracted so that mother and baby can be buried separately.
But during an Ebola epidemic, it would have been extremely dangerous to carry out a surgical operation on the dead woman to remove her baby. Without an agreement between the medical teams and the population, the woman could not be buried, and her body began to decompose.
“We need to respond appropriately and with tact, taking account of the sensitivity of the population but also of the pressing need to bring to an end the suffering caused by the disease.”
Sylvain Landry Faye, Cheikh Anta Diop University
Faye’s team of anthropologists intervened to understand local people’s reticence to burying her without the operation and to try to find a solution.
“There is a principle in anthropology that says that, whenever there’s a rule, there’s an exception,” he explains. “Therefore we just needed to find this exception within the specific framework of Kissi society. After discussions with the elders from the young woman’s village, we came to an agreement. In short, if it was impossible to remove the foetus from the mother’s belly, for one reason or another, there had to be a reparation ritual, consisting of offerings and various ceremonies. So we asked the WHO to pay for the reparation ritual, and that’s how the burial took place.”
But the most serious incidents requiring the anthropologists’ mediation took place in the town of Tekoulo in the prefecture of Gueckedou in the south of the country, where a group of prominent citizens, who had come to raise public awareness of the situation, were beaten up by a gang of young people and where humanitarian workers’ vehicles were damaged.
At the villages of Kolo Bengou and Wabengou in the same prefecture, staff from Médecins Sans Frontières were also held, and the elders who were accompanying them attacked.
After being called in to help, the anthropologists mediated and tried to understand the reasons behind the attitude of the gang of youths. The anthropologists discovered that the young people had decided to protect themselves from Ebola by living on the edge of society. They also explained that they feared the elders and humanitarian teams would spread the virus to them.
Since then there have been reports that a small team of health workers and journalists visiting the village of Womey in the South-East of Guinea were stoned to death by angry residents. So the anthropologists’ work looks set only to become more important.
“Our work consists of understanding the mechanisms of these behaviours and the reasons behind them,” says Faye. “We need to respond appropriately and with tact, taking account of the sensitivity of the population but also of the pressing need to bring to an end the suffering caused by the disease.”
A version of this article was originally produced by SciDev.Net’s Sub-Saharan Africa (French) desk.














