By: Anita Makri
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
As the scramble to deal with Ebola dies down, a long list of challenges about responding to public health emergencies is beginning to come more clearly into focus. Many of the factors that contributed to the scale of the epidemic are more or less familiar: imperfect governance of global bodies like the WHO, reflected in a tardy response to this particular outbreak, is one; the chronic weakness of health systems is another; a lack of incentives for drug R&D is yet another. Others are perhaps more specific to this disease: the race to contain unfamiliar or particularly virulent pathogens, and slowing the environmental degradation that brings people in closer contact with zoonoses (diseases that get passed on from wildlife).
Yet a much less familiar voice in traditional public health circles is that of the anthropologist. Luckily, I heard from two last week (6 February) at an Ebola symposium at the Royal Society of Medicine in London. They took the audience through some lesser known nuances of this epidemic, lending some subtlety to the symposium’s title ‘Ebola: the 21st century plague?’.
The need for a social science perspective became clear from an early stage in the outbreak in West Africa. Some of the interventions typical of Western medicine and science clashed, at times violently, with social norms and traditional beliefs. But when the Institute for Development Studies’ director Melissa Leach took the podium she was quick to dispel any notion that this has to do with exotic, traditional cultures that, from a distance, might seem difficult to understand. People are human, practical and pragmatic, she said, and proceeded to lay out how responses to the epidemic show this.
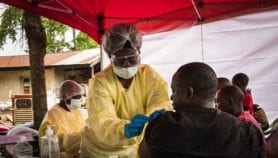
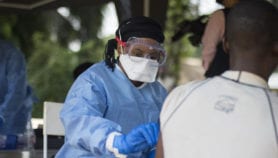
“Ebola is deeply linked with social life”, she said. Because the main routes of transmission of the virus are linked to everyday life, and especially people like health workers or caregivers, public health recommendations can appear antisocial. The fact that women are often the main carers also has an impact on the epidemiology — a point reinforced later on by Heidi Larson of the London School of Hygiene & Tropical Medicine, who stressed the need to engage with women when implementing interventions.
By the time the international response scaled up there was already an epidemic of fear in West Africa, said Leach. But this intensified when the global response came in. Many incidents of violence were about fear and distrust of not just the virus but of control efforts.
The social turmoil came to a head in September when villagers attacked and killed eight health workers and journalists who visited a remote village in Guinea to raise awareness about the disease. Here Leach pointed to slavery and extraction of natural resources by colonial powers as examples of a long history of exploitation that “give a logic, if not exoneration”, to violence that might otherwise be interpreted as a sign of a backward region.
Even when it comes to healthcare systems, usually discussed in terms of poor staffing and equipment, anthropology emphasises the other side of the coin and forces us to look at how people respond. People in rural areas affected by Ebola hardly visited clinics before the outbreak because there was nothing there, Leach explained — so the default response to Ebola is to practise home care.
Similarly, caring for the dying and the dead involves a lot of social interaction, Leach explained. Mass cremation policies in response to the outbreak led to burial practices being kept secret, and a market for fake certificates listing causes of death other than Ebola. Eventually, burials were adapted to allow some contact with the dead body without putting others at risk.
But adaptations also had a positive impact on infection control. In her talk Larson mentioned the production of fabrics and music that contain messages about Ebola as examples.
“I have been very impressed by the innovation that’s happened around the Ebola response,” she said. “Listening to everyday life has to happen, and has to happen early.”
Adaptations, it seems to me, can go both ways: they can fuel outbreaks, or help control them. Either way, spotting them can make a difference. So talks about reforming health systems might need to look beyond the traditional disease control paradigm. To deal with similar crises, chances are that doctors and epidemiologists will need to work with insights from social science and local learning.