By: Sten Vermund and K. M. Venkat Narayan
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Chronic disease among HIV positive people has been overlooked, say K. M. Venkat Narayan and Sten Vermund.
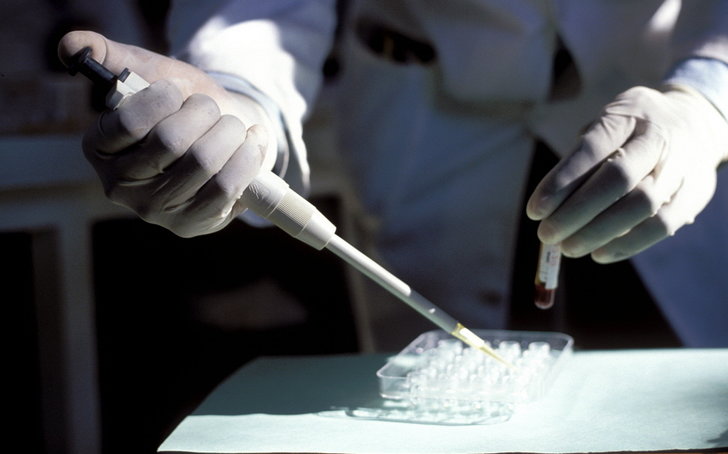
Over 35 million people worldwide are living with HIV. Massive global efforts and investments to deliver combination antiretroviral therapy (ART) have transformed a fatal infectious disease into a chronic, treatable disease.
HIV-infected people who comply with ART now have near-normal lifespans — but as a result they may face the new threat of chronic noncommunicable diseases (NCDs). Stress, stigma, aging and HIV-related inflammatory changes increase the risk of some cancers as well as diabetes, heart disease, stroke, chronic kidney disease and mental health problems.
The huge gains made from implementing ART globally — 13 million people now get this treatment, nearly 90 per cent of whom live in low- and middle-income countries (LMICs) — will be lost unless the rise of NCDs in HIV survivors is addressed. High-income nations have been tackling this challenge since 1996, and it is time to do the same in LMICs too.
Uncertain risk
The problem of NCDs in HIV positive people in LMICs has been under-appreciated. This is partly due to scarce data and patchy evidence.
The extent to which HIV positive people who live in LMICs are at higher risk of NCDs than people who are HIV negative is unclear — as are the factors that might put them at higher risk. We also don’t fully understand whether HIV positive people differ from the general population in the disease patterns for various NCDs, either due to HIV itself or its treatment.
For example, some studies have suggested that certain ART treatments may increase the risk of diabetes. There are also concerns about how ARTs may interact with drugs commonly used to manage NCDs. Some conditions, such as infectious myocarditis and other heart conditions associated with opportunistic infections, may be of special concern in countries where the prevalence of infectious disease, malnutrition and other poverty-related conditions is relatively high.
But a more important question is this: how must effective systems be developed to deal with NCDs among HIV survivors in regions facing severe resource constraints?
Multipronged research
Answering these pressing questions will require a multipronged research agenda.
First, it will take sound public health surveillance — data from good systematic collection systems and from studying groups over long periods — to measure the burdens of NCDs and their risk factors in HIV positive populations, and to compare them with HIV negative people.
“The battle against HIV has taught us that pharmacological approaches need to be combined with behavioural interventions.”
K. M. Venkat Narayan and Sten Vermund
These data will also enable estimation of the health and economic impacts of NCDs in HIV infected populations such as the cost to individuals, families and society, and the cost-effectiveness of managing disease. Such economic estimates can help with advocacy and to inform policy on where to invest scarce resources.
The second element is basic and clinical research. This is needed to investigate how inflammation, coagulation and immune mechanisms affect how NCDs develop among HIV infected people. Such research can also inform the development of diagnostics and treatments.
For resource-poor countries, it is important to have access to low-cost tools to diagnose and treat NCDs. Some tools, such as point-of-care testing and combination drug therapy, are already available; others could be developed through collaboration between academic institutions and industry.
Finally, implementing science and health systems that can deal with the rise of NCDs in HIV survivors will be crucial. This will involve generating data on the efficiency, cost-benefit ratio and feasibility of screening tests, affordable diagnostics and drug delivery tools.
It will also involve testing innovative models of integrated HIV and NCD prevention and care. Such models might include better trained health workers, and use of telemedicine and mobile phone technologies for health education, prompts to encourage treatment compliance and to connect various parts of the health system. Innovation is needed because few health delivery systems are currently integrated to allow coordinated management of NCDs and infectious diseases.
Lessons from HIV
There are lessons to be learned from the successful global fight against HIV, which was made possible through major advances in implementing treatment protocols, improving diagnostics and drug delivery, and strengthening health systems.
For example, the global health community collaborated to lower the cost of combination therapy for HIV (taking two or more drugs at a time), and to finance it in LMICs with support from organisations such as the Clinton Foundation. Collaborative work was also crucial for developing tests to identify NCD risk factors early on and low-cost combination therapy for NCDs using generic drugs, such as statins or anti-hypertensive drugs. The development and marketing of such polypills (drugs combined in a single formulation) requires firms that are interested in collaborating with academic institutions to deliver low-cost treatments.
The battle against HIV has also taught us that pharmacological approaches need to be combined with behavioural interventions, for example through promoting condom use. The same principle can be applied to NCDs.
In an era of finite resources, leveraging the global HIV infrastructure to tackle the rising NCD burdens in HIV survivors is the obvious way forward. This will require active interdisciplinary collaboration.
There is some low-hanging fruit. Establishing studies to compare the incidence of NCDs between HIV positive and negative people, for example, can leverage existing surveillance or clinical trials data on groups of HIV positive people. Other immediate steps forward could be to evaluate integrated delivery interventions for combined HIV and NCDs, and to test how mobile technologies can help enhance compliance with treatment and train healthcare staff.
Building on HIV control platforms developed from internationally funded initiatives such as PEPFAR (US President’s Emergency Plan for AIDS Relief) and the Global Fund to Fight AIDS, Tuberculosis and Malaria would serve as a good start.
K. M. Venkat Narayan is the Ruth and O. C. Hubert Chair of Global Health, professor of epidemiology and medicine, and director of the Emory Global Diabetes Research Center at Emory University, United States. Sten Vermund is director of the Institute for Global Health and professor of paediatrics, medicine and health policy at Vanderbilt University School of Medicine, United States. Narayan can be contacted at [email protected] and Vermund at [email protected]