By: Alice Hazelton
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
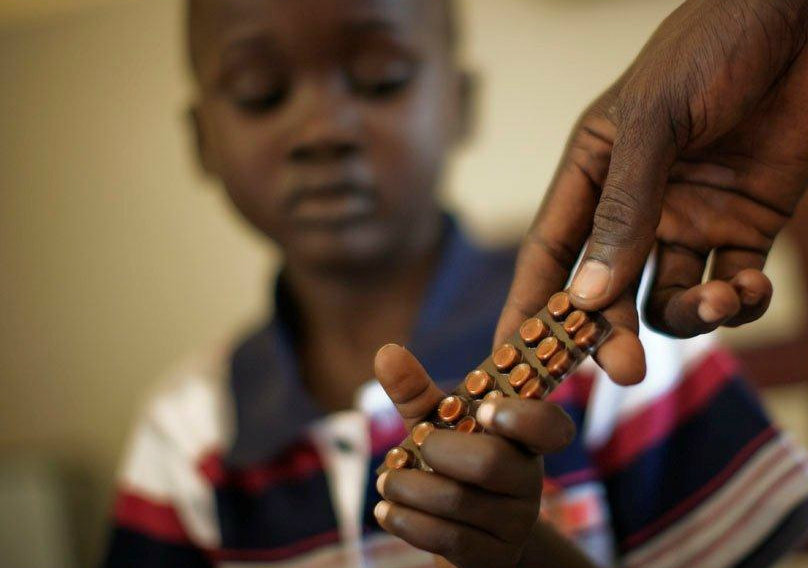
A new genetic test for tuberculosis (TB) could dramatically improve the accuracy of diagnoses of infected children in developing countries, although a simple diagnostic kit could be some way off.
The research, published last month (1 May) in the New England Journal of Medicine, examined the DNA of more than 2,800 children admitted to hospitals in Kenya, Malawi and South Africa with TB symptoms. It identified specific gene sequences that appear more frequently during a TB infection — providing scientists with a genetic signature for the disease.
Although the technology currently needed to detect this signature is too advanced for use in most resource poor settings, the researchers say it should be possible to develop a diagnostic test that can be used in such places.
The WHO estimates 530,000 children were infected by TB in 2012, the majority in developing countries.
“There’s a big difference between diagnosing TB in children and diagnosing it in adults.”
Brian Eley, University of Cape Town
“Every single day we face the problem of diagnosing TB in children and there’s a big difference between diagnosing TB in children and diagnosing it in adults,” says Brian Eley, a paediatric infectious diseases specialist at the University of Cape Town who led the clinical study in South Africa.
In adults, the TB-causing bacterium can often be detected in coughed-up mucus, but Eley says that such methods — and even scans and skin tests — only identify the bacterium in children at best about a fifth of the time in the developing world. This leaves doctors relying on often misleading symptoms, meaning that an accurate diagnosis is often only made when a child is critically ill.
In the study, researchers took blood samples from children in Malawi and South Africa and examined them to see which genes were activated as part of the immune response to a TB infection. Using a ‘DNA chip’, which measures the expression of large numbers of genes simultaneously, a ‘signature’ of 51 genes was identified, allowing TB to be distinguished from both latent TB and other diseases that mimic the disease’s symptoms.
Eley says this is the first study to identify the minimum set of genes that could be used with a high degree of certainty to identify TB.
A ‘risk score’ for TB developed from these was tested in Kenya, accurately diagnosing the disease in more than 80 per cent of children.
The next step is to take this high-tech method and convert it into something that can be used at the bedside or under the laboratory constraints in which many African clinicians work, says Eley.
Yet the results are “still quite a long way from being turned into a diagnostic test suitable for use in a resource-poor setting,” says Ruth McNerney, a TB expert at the London School of Hygiene & Tropical Medicine, United Kingdom.
McNerney says the team’s procedure involved freezing samples at minus 80 degrees Celsius. “That’s a million miles away from what you could do in a lab in Africa,” she says.
She adds that looking at host responses for diagnosing TB is problematic because people respond differently to TB in different parts of the world, bacteria are different in different parts of the world and TB is a complex disease with several growth stages within the body.
References
New England Journal of Medicine doi: 10.1056/NEJMoa1303657 (2014)