08/04/20
Rich countries ‘raiding’ developing world’s nurses

By: Fiona Broom
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Rich countries are ‘raiding’ nurses from their lower-income neighbours, a global nursing organisation says, leaving parts of the global South with less than 900 nurses for every one million people.
The first-ever State of the World’s Nursing report, timed to coincide with World Health Day, paints a stark picture of the disparities between rich and poor countries’ health systems.
Global imbalances of critical nursing staff are being exacerbated by the failure of developed countries to educate and train their own nurses, say the report’s authors.
“Retention is as important as recruitment. And retention means that we have to take much more seriously improving working conditions.”
Howard Catton, chief executive, International Council of Nurses
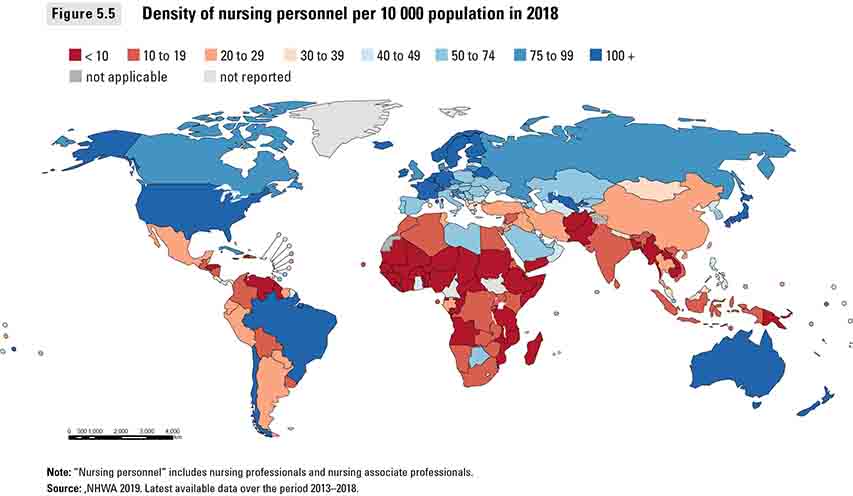
Europe and the Americas average about 81 nurses per 10,000 people. In the Western Pacific the ratio is 36 nurses to every 10,000 people.
But in Africa there are just 8.7 nurses for every 10,000 people, and in South-East Asia and the Eastern Mediterranean about 16 per 10,000.
“Eighty per cent of the world’s nurses only currently serve 50 per cent of the world’s population,” says Mary Watkins, alternate chair at Nursing Now, which co-produced the report with the International Council of Nurses (ICN) and the World Health Organization.
These under-staffed regions will be short of 5.7 million nurses by 2030, the report estimates.
“That’s over a 20 per cent shortage, but we know that it’s even higher in certain areas because of the maldistribution that we have,” says ICN chief executive Howard Catton.
Data from the OECD (the Organisation for Economic Co-operation and Development) shows the number of foreign-trained nurses in wealthy states increased more than 20 per cent between 2006 and 2016.
“We have an over-reliance in high income countries on migration,” Catton says.
“We know migration has been a problem for a while, and it looks like it could be set to be worse, also because of the ageing populations in the EU and America.
“If they raid low- and middle-income countries it will exacerbate shortages and maldistribution."
The report provides evidence needed for investment in the health workforce and nursing, and can help inform where the money should go to have the biggest population health impact, says the WHO’s Carey McCarthy.
The data point to major inequities and stumbling blocks, she adds.
Working conditions in many countries “range from woeful to shameful”, says Catton. Nurses in Zimbabwe earn about US$60 a month, he says, while exhausted nurses in under-resourced systems suffer high levels of stress and burnout, making migration more attractive.
“Retention is as important as recruitment. And retention means that we have to take much more seriously improving working conditions,” Catton says.
Resourcing, recruitment, retention and ongoing training are brought into sharp focus by the report, Nursing and Midwifery Council chief executive Andrea Sutcliffe says, particularly as COVID-19 frontline nurses and midwives are “laying down their lives while doing their utmost to care for the rest of us”.A Lancet editorial describes the nursing report, and the third State of the World's Midwifery report due next year, as essential, giving a foundation to global conversations about caring, well-being, the value of work, and equality.
“As much as nurses and midwives are vital for delivering health for all, it seems clear that the full potential of nursing and midwifery is not being used by the global health and medical communities,” The Lancet says.
“An inescapable conclusion is that this is due to gender bias and the low value placed on women's work, which characterises these so-called feminised professions.”

