By: Alice Hazelton
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
A cheap and simple way to obtain the main type of disease-suppressing antibody in human blood could help save the lives of patients in the developing world with malfunctioning immune systems.
The method of collecting immunoglobulin G (IgG) may enable more patients with primary immunodeficiencies (PID) to get the regular antibody doses they need.
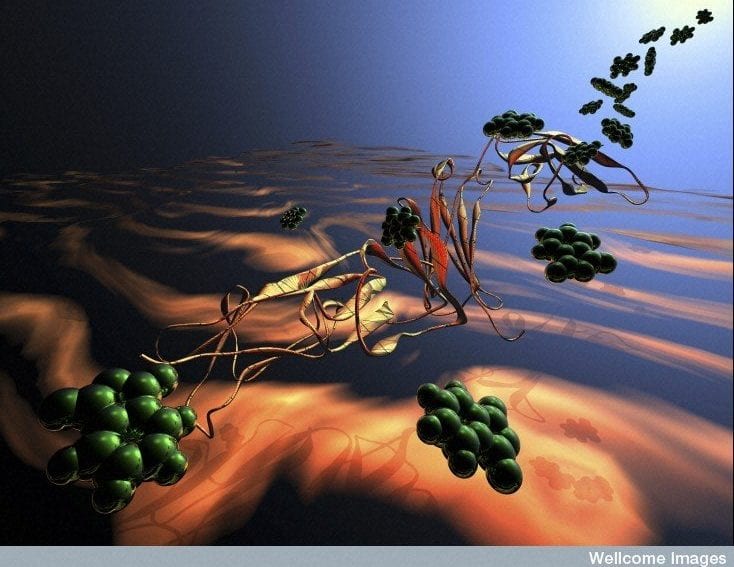
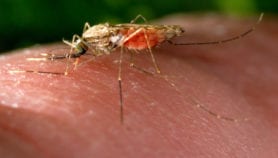
Immunoglobulins bind to bacteria and viruses in the blood, fighting infections such as Ebola. Doses of the antibodies are normally prepared in sophisticated laboratories. These labs require blood plasma donations from around 30,000 people to produce economically viable amounts of antibodies.
The method was developed by Thierry Burnouf, who runs the Graduate Institute of Biomedical Materials and Tissue Engineering at Taipei Medical University, Taiwan. A description of the method appeared in PLOS Neglected Tropical Diseases last month (26 February).
Burnouf says that the World Health Organization uses antibodies harvested from convalescent plasma to treat Ebola patients in West Africa. “But you cannot fractionate the plasma from 30,000 donors in affected countries so the concept of using a small pool of Ebola plasma makes complete sense,” says Burnouf.
The new process can be done outside the lab as it needs only a centrifuge, some disposable equipment such as blood bags and filters, and around 20 plasma donations to produce economically viable amounts of immunoglobulins.
Pooled plasma donations undergo two phases of separation. In the first, the frozen plasma is thawed and centrifuged while still in its original bag to maintain a sterile environment. The leftover blood constituents can be used to treat haemophiliac patients, for example.
In the second phase, the remaining liquid is mixed with an inexpensive chemical called caprylic acid to liquefy the antibodies. This mixture is then purified and filtered to remove any bacteria.
A patient affected by PID requires around 400 milligrams of immunoglobulin for every kilogram of bodyweight each month. This currently costs around US$1 a gram, but Burnouf says the new system halves this cost.
Burnouf says that IgG produced using the new method is being trialled for safety in Cairo, Egypt, in a small group of children affected by PID. He hopes it will be available for wider distribution by early 2016.
Paul Strengers, president of the International Plasma Fractionation Association, agrees it should be easy to implement the new technique in blood centres in the developing world. “This is a major step forward and a completely new approach in the manufacturing of these important plasma-derived medicines,” he says.
But a tropical medicine professor, who spoke to SciDev.Net on the condition of anonymity, says the technique may face legal challenge, potentially making it more expensive than Burnouf expects. “Caprylic acid purification of IgG has been patented, so there may be serious legal challenges to its widespread use, even in Africa,” the source says.
> Link to the full study in PLOS Neglected Tropical Diseases
References
PLOS Neglected Tropical Diseases doi: 10.1371/journal.pntd.0003501 (2015)