By: Janet Kilby
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
It is a hundred years since the discovery of Chagas disease — but progress in eliminating it has been marred by lost opportunities, say campaigners.
Of all the forgotten diseases, Chagas is one of the least well known. Much of the world has never heard of it. Yet 14 million people are affected and 15,000 die from it. So it was hardly surprising that advocacy groups were delighted when Chagas was included on the agenda for last May’s World Health Assembly in Geneva, Switzerland — a meeting of health ministers organised by the WHO.
Here, at last, was the chance for countries to step up their commitment to tackling this insect-borne disease. The timing was providential — 2009 is the 100th anniversary of the disease’s discovery by Brazilian doctor and scientist, Carlos Chagas.
Shelved for swine flu
But the meeting ended in anticlimax for Chagas campaigners. The WHO reduced its agenda so that officials could discuss pandemic readiness and then return home five days early to prepare for the spread of swine flu. As a result, discussions on Chagas were shelved until 2010.
Roger Teck, director of operations for Médecins Sans Frontières (MSF), was dismayed.
"We had expected that the WHO would adopt a resolution where all affected countries agree to integrate care of acute and chronic Chagas patients into their primary healthcare systems, and to invest more in research," he said. His colleague, Gemma Ortiz, told Reuters she was "completely amazed and gutted at the same time".
Chagas: a neglected disease
Chagas disease is a debilitating and often fatal disease resulting from infection with the protozoan parasite Trypanosoma cruzi. T. cruzi passes to humans via triatomes — a subfamily of predatory insects endemic to Mexico, Central America, and South America. These insects, sometimes known as ‘kissing bugs’ because of their attraction to human faces, thrive in straw and clay homes, taking shelter in cracks in the walls during the day and emerging at night. Typically, an insect will jump and glide until it lands on a sleeping person. It will then proceed to bite the flesh — often near the eyes or mouth — and defecate. The disease spreads when a victim scratches the site of a bite and unknowingly rubs parasite-laden faeces into the blood system.
It has become increasingly clear in recent years that T. cruzi can also be transmitted in blood and organs from infected donors. And women can infect their children during pregnancy, delivery or while breastfeeding.

The disease was discovered by Brazilian doctor and scientist, Carlos Chagas
Wikicommons/J Pinto
There is no vaccine against Chagas disease. Patients are generally treated with one of two drugs, nifurtimox and benznidazole, both of which are old, toxic and lacking in specificity. They are, however, relatively successful at treating early-stage (acute) infections.
But there’s the rub — the early phase of infection often goes undetected as symptoms are usually mild. Sometimes patients note a fever, headache or diarrhoea but often symptoms go no further than a swelling at the site of infection. It is usually many years later — as many as 15 — that the chronic phase of infection sets in and it is at this stage that infected people experience serious symptoms. An estimated 30 per cent develop heart disease and gastrointestinal tract disease, usually leading to disability and death. Drugs are generally ineffective at this stage.
Chagas is the disease with the highest impact in Latin America. It is probably causing over two-and-a-half times more lost years of healthy life than malaria, leprosy, bilharzia and leishmaniasis combined. Yet little is being done to improve its treatment or prevention. Why?
A disease of the poor
The main obstacle appears to be the population profile of those most burdened by the disease. Chagas affects the poor in remote rural areas, making it a commercially unviable candidate for drug development. The WHO categorises Chagas as a neglected tropical disease, recognising that more research is essential — there are gaps in medical knowledge at the most basic level. Even the optimum length of treatment remains unknown.
Better drugs with fewer side-effects are urgently needed, says Luis Eugenio Portela Fernandes de Souza, former director of the Science and Technology Department of the Brazilian Ministry of Health. It is also vital to create an infrastructure in Central and Southern America that allows populations to be screened for the condition, and treatment to be delivered effectively. But such an infrastructure poses an enormous challenge as many afflicted communities have no access to health care systems.
Another area that needs urgent attention is diagnosis, de Souza says. There is no standardised diagnostic test on the market, says the UK medical journal The Lancet.
And the challenges do not end there. Where Chagas disease is endemic, it must also be a top priority to methodically kill the insect vector so that treated people don’t become re-infected.

It must be a top priority to methodically kill the ‘kissing bugs’ that carry the disease
Flickr/gauchocat
There are positive precedents for insect-control programmes. In Uruguay, Chile, and Brazil, for instance, the main vector that transmits the disease has been virtually eliminated.
Unrealistic aims
But with 50,000 new cases of Chagas reported every year, these examples of disease prevention are clearly not enough.
"The focus on prevention ignores the needs of those who are already infected and are suffering in silence. In endemic countries, governments should do active screening, diagnose and treat many more patients," says Ortiz, MSF’s senior advocacy officer for Chagas.
The WHO appeared to acknowledge the problem in 2007 when it launched its Global Network for Chagas Elimination — an initiative that aims to coordinate global efforts to eliminate the disease by 2010.
But cellular biologist Rick Tarleton is not holding his breath. Setting deadlines without properly understanding the scale of the problem and the potential impediments is simply wishful thinking, he says.
Tarleton, a researcher from the Center for Tropical and Emerging Global Diseases at the US-based University of Georgia, says of the 2007 initiative: "Although 2010 is a laudable goal, it seems doomed to failure from the start — how can a disease be eliminated in two and a half years when there is no good estimate of the full impact, no real plan for how elimination would be achieved, and no truly effective tools for diagnosis, treatment and assessment of the effectiveness of interventions?".
Global spread?
Writing in The Lancet, Ricardo Pereira Igreja, from the Universidade Federal do Rio de Janeiro, in Brazil, notes that Chagas is no longer simply a bug-transmitted disease endemic to rural areas of Latin America, but an urban, globalised disease with new clinical presentations.
Growing human migration and mobility have increased the geographic distribution of Chagas in recent decades and the disease now has the potential to become an international threat.
Cases are being seen in travellers to North America, Europe and Japan.
What’s more, new means of Chagas transmission are emerging — infections from contaminated food and even fruit juice have been reported. Sharing intravenous needles is another relatively new means of transmitting T. cruzi infection. The insect vectors appear to be developing resistance to pesticides.
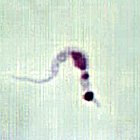
There is hope that new drugs will be developed once the T.cruzi genome is completely sequenced
Wikicommons/CDC
Joseli Lannes, researcher at the Oswaldo Cruz Institute at Fiocruz in Brazil, and a coordinator of the Institute’s Integrated Programme on Chagas Disease, told SciDev.Net that new species of insects starting to spread the disease.
This has resulted from human actions, says Lannes. Environmental destruction has reduced the pool of wild animals from which insects would traditionally feed, forcing a wider variety of kissing bug to turn to humans for food.
To Tarleton, the challenges posed by Chagas disease are frustratingly plentiful, both from an operational standpoint — how to make use of accessible resources to prevent new infections or treat existing ones — and from a research perspective.
New treatments, new money?
For those who can afford it there are glimmers of hope. Direct stem cell therapy of the heart muscle using bone marrow cell transplantation shows promise as a way to reduce heart failure in patients with chronic Chagas disease.
There is also hope that new drugs will be developed once the T. cruzi genome is completely sequenced. Several experimental treatments have shown promise in animal models and a number of potential vaccines are being tested.
Lannes is optimistic that drugs being developed for leishmaniasis and African trypanosomiasis (African sleeping sickness) may also be useful for treating Chagas disease. All three conditions are caused by parasites from the Trypanosomatidae family, and in recent years there has been a degree of consolidation in international efforts to find treatments for these diseases.
But arguably the most significant development for victims of Chagas disease is the recent establishment of a Therapeutics for Rare and Neglected Diseases programme in the United States. This initiative, launched in May by the US National Institutes of Health (NIH), aims to speed up drug development and to stimulate research collaborations. With the NIH pumping US$24 million into this year’s budget for the programme and Chagas disease on the agenda, perhaps there is a chance that this vexing condition will finally receive the attention it so desperately needs.

