25/02/21
Ebola: 20,000 vaccine doses to tackle Guinea outbreak

By: Julien Chongwang
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
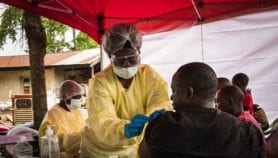
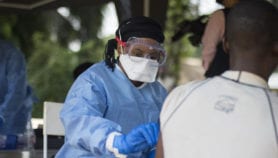
As the first shipment of COVID-19 vaccines arrived in Africa this week, another vaccine was being rolled out in Guinea, in a bid to stop a fresh outbreak of Ebola in its tracks.
Mass immunisation got under way on Tuesday (February 23) after 11,000 doses of the Ebola vaccine landed in the West African country as part of an emergency response to the outbreak, the World Health Organization (WHO) confirmed on Twitter.
The Ervebo vaccines (rVSV-ZEBOV-GP) are the first to be drawn from an emergency stockpile housed in Basel, Switzerland. The stockpile, announced by the WHO, the vaccine alliance Gavi, and partners last month will eventually offer low and lower middle-income countries access to 500,000 doses of the Ebola vaccine.
“We must avoid falling into the trap of thinking that because we have a vaccine we can pay less attention to the traditional responses to Ebola …”
Anja Wolz, Doctors Without Borders (MSF)
Around 9,000 additional doses were also due to arrive in Guinea from the United States, the WHO said.
Drawing on experience of the latest Ebola outbreak in the Democratic Republic of Congo (DRC), experts believe that the vaccine rollout, which began nine days after the first cases were confirmed, is a crucial part of the emergency response.
Georges Ki-Zerbo, WHO representative in Guinea, said: “The vaccine can help us manage the situation by protecting communities exposed to reported cases.”
Doctors Without Borders (MSF), sounded a note of caution, however. Anja Wolz, coordinating MSF’s emergency response to the outbreak, said: “It’s true that a major difference with the 2014-2016 outbreak is that we now have treatments and vaccines. [But] the best use of the vaccine will depend on the quantities available and transmission modes.
“We must avoid falling into the trap of thinking that because we have a vaccine we can pay less attention to the traditional responses to Ebola, such as contact tracing, safe funeral practices, and community engagement, as well as the treatment and isolation of patients.”
According to Wolz, if communities are involved in and support the response, the benefit is “huge”. Conversely, if the community is afraid or antagonistic, things can become a lot more complicated, whether vaccines are available or not.
Response teams are already on the ground in Guinea where questions remain about how the outbreak started.
Ki-Zerbo told SciDev.Net that the causes of the outbreak were being investigated by scientists using the “One Health” approach encompassing the health of people, animals, and the environment. This approach targets public health risks emerging from the human-animal-environment interface.
The WHO released a statement on 17 February tracing the movements of the first known victim, a nurse who had originally presented at a health centre in the town of Gouecke on 18 January with symptoms including headache, vomiting, abdominal pain, and fever. She was initially diagnosed with typhoid and later, at a second health facility, with malaria. She died on 28 January.
Six other cases of the virus were subsequently confirmed – five family members of the nurse and a traditional medicine practitioner she had visited.
“The fact the first recorded case was a health care worker does suggest community transmission may have already been occurring,” said Wolz. “But we need to piece together a detailed history of contacts to establish the antecedents to this first recorded case.”
‘Complex’ crisis
According to the WHO, 192 contacts had already been identified by 17 February and there was no indication at that date that contacts had travelled to neighbouring countries (Liberia and Ivory Coast).
“Everything is being done to stop this outbreak becoming as widespread as the one we witnessed from 2014-2016,” stressed Ki-Zerbo.
“The lessons learned from the 2014-2016 outbreak must be fed into this intervention while bearing in mind the complexity related to the COVID-19 response, the complexity of the cross-border dynamics and community engagement,” he added.
The rollout in Guinea comes as Ghana became the first country outside India to receive COVID-19 vaccines via the COVAX facility, established during the global pandemic to ensure equitable access to the vaccines.
Wolz believes the Ebola response in Guinea must be rapid and well thought through in order to minimise the risk of the outbreak becoming as severe as that of 2014-2016. She hopes the availability of treatments will make it easier to encourage people to access health care and to quickly self-isolate.
“If the messages are appropriately communicated, we have o a much better chance of being able to conduct effective contact tracing and break the chains of transmission,” she added.
During West Africa’s first outbreak of Ebola, between 2014 and 2016, 28,000 people were infected and around 11,000 died in Guinea, Liberia, and Sierra Leone.