By: Paul Adepoju
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
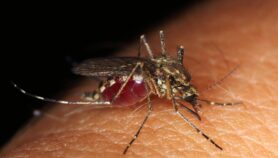
[IBADAN, NIGERIA] The WHO and partners have launched country-led and country-owned response to increase the uptake of malaria control strategies following a “wake-up call” report that shows that progress on the disease has stalled for a second consecutive year since 2010.
The progress has particularly stalled in Sub-Saharan Africa, the new WHO report says.
Malaria is one of the world’s major health problems, with Sub-Saharan Africa alone accounting for 92 per cent of cases and 93 per cent of malaria deaths, according to the WHO.
Experts have been expecting increasing decline of malaria cases because of investments into controlling the disease over the years but after steady decline from 2010 to 2015, there were increased cases in 2016 and 2017.
“This is a massive wake-up call that has refocused attention on the countries hardest hit by malaria.”
Pedro Alonso, WHO Global Malaria Programme
“Nobody should die from malaria but the world faces a new reality,” says Tedros Adhanom Ghebreyesus, director-general of the WHO, adding that the world is at risk of squandering years of toil, investment and success in fighting malaria.
The World Malaria Report 2018 released last month (19 November) reveals that there were about 219 million cases of malaria in 2017, about two million more cases than that of 2016.

Malaria cases worldwide, 2010-2017. Source: WHO
The report shows that India and ten countries in Sub-Saharan Africa — Burkina Faso, Cameroon, Democratic Republic of the Congo, Ghana, Mali, Mozambique, Niger, Nigeria, Tanzania and Uganda — accounted for about 70 per cent of all malaria cases and 274,000 deaths.
But improvements were recorded in Ethiopia and Rwanda that recorded 240,000 and 430,000 fewer cases respectively in 2017 than in 2016.



Source: WHO
The WHO calculated estimates of malaria cases from routine data from 91 countries. The findings of the report threaten the Global Technical Strategy for Malaria 2016–2030 which calls for reducing malaria cases and deaths by at least 40 per cent by 2020, 75 per cent by 2025 and 90 per cent by 2030.
Abdisalan Noor, WHO Global Malaria Programme’s team leader for surveillance, tells SciDev.Net that the slowed progress could be attributed to insufficient funding.
“Inadequate funding has resulted in major gaps in coverage of core malaria control tools that prevent, diagnose and treat malaria,” says Noor. “In 2017, for example, an estimated half of the population at risk of malaria in Africa did not sleep under a treated net.”
Pedro Alonso, director of the WHO Global Malaria Programme, adds that the report underscores the need for an immediate change in approach against malaria.
“This is a massive wake-up call that has refocused attention on the countries hardest hit by malaria,” Alonso notes.
To speed up malaria control efforts in the worst hit countries to achieve goals of the global technical strategy, the WHO and the RBM Partnership to End Malaria launched a response called ‘High burden to high impact: a targeted malaria response’ in Mozambique last month (19 November). The response is expected to be country-owned and country-led.



Source: WHO
Its key elements are political will to reduce malaria deaths; strategic information to drive impact; better guidance, policies and strategies; and a coordinated national malaria response.
Victoria Feyikemi, executive director of the African Development and Empowerment Foundation, an initiative that provides free malaria testing and treatments in Nigeria, especially in rural areas, says that efforts to combat malaria in Sub-Saharan Africa should also include tackling self-treatment.“Self-treatment remains an issue affecting even well-educated people. In many cases, we have seen people treat malaria with paracetamol. Many will not seek medical services until the disease has become life-threatening with severe anaemia setting in,” explains Feyikemi, adding that such cases often result in death.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.
References
World Malaria Report 2018 (WHO, 19 November 2018)