16/03/26
Why sleeping sickness pill is raising hopes in Africa
By: Gilbert Nakweya
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[NAIROBI, SciDev.Net] Sleeping sickness has been killing people across Africa for generations. A disease with no vaccine, spread by the bite of a tsetse fly, it was once treated with injections of an arsenic derivative, a cure that could be as dangerous as the illness itself. By 1998, it was infecting 40,000 people a year.
Last month, the single oral-dose medicine Acoziborole Winthrop (acoziborole) became the newest and simplest weapon against the disease when it was given the nod for approval by European regulators.
The treatment was developed by French pharmaceutical company Sanofi in partnership with the Geneva-based Drugs for Neglected Diseases Initiative (DNDi), with human trials in West and Central Africa.
Now researchers are pushing further: a paediatric trial, ACOZI-KIDS, is now underway in Democratic Republic of Congo and Guinea to find out whether the same drug can work for children aged one to 14, the one group the current approval does not yet cover.
Here is what the breakthrough means, and why the work is not yet finished.
What is sleeping sickness?
Sleeping sickness, or human African trypanosomiasis (HAT), is a parasitic infection spread by tsetse flies.
Without treatment, it is usually fatal. The most common form of the disease caused by the parasite Trypanosoma brucei gambiense is found across Central and West Africa.
Around 40,000 cases were reported across the continent in 1998, with more than 300,000 others estimated to have gone undetected and untreated, according to the World Health Organization (WHO).
Sustained efforts over the past two decades have reduced those numbers dramatically. By 2024, confirmed cases had fallen to fewer than 600. But those remaining cases are, almost by definition, the hardest to reach.
What was wrong with the old treatments?
“The treatment that was available was an injectable arsenic derivative with serious side effects,” said Wilfried Mutombo, regional head of clinical operations for DNDi in West and Central Africa, referring to the long-standing treatment Melarsoprol.
“We wanted to find something better for the patients,” he added.
While newer, safer alternatives have been developed, existing therapies involve multiple doses, intravenous infusions or intramuscular injections, and hospitalisation. They also require patients to be reached twice: once for diagnosis, once for treatment.
In areas with poor roads and no internet access, that second visit often never happens. A Lack of cold chain infrastructure, trained injectors, and local hospitals are all barriers between a sick person and a cure.
What does the new drug do differently?
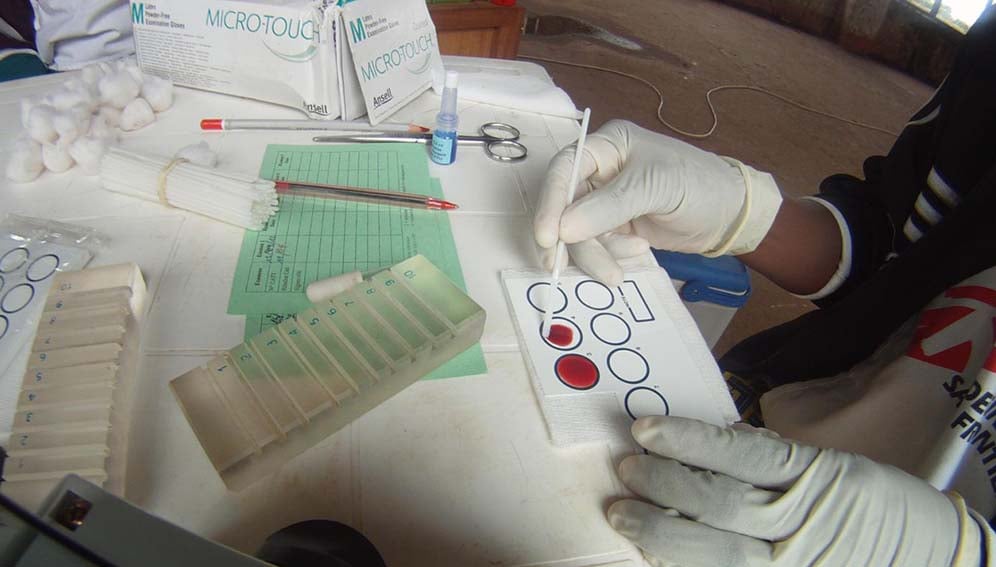
Acoziborole collapses the entire treatment chain. Health workers can now test and treat in a single encounter, in the field, with no specialist equipment. Researchers say it enables “test-and-treat” strategies in remote settings that were previously impossible.
The drug is a single oral dose—three tablets, taken once, in one day. It works across both early- and late-stage disease and removes the need for the lumbar puncture, or spinal tap (a needle inserted into the lower back) previously required to determine disease stage before treatment could begin.
The treatment represents more than two decades of research, building on the injectable NECT regimen introduced in 2009 and the first oral treatment, fexinidazole, in 2018.
Has it been proven to work?
The European Medicines Agency’s Committee for Medicinal Products for Human Use recommended Acoziborole approval on 27 February, based on Phase 2 and Phase 3 clinical trial results published in The Lancet Infectious Diseases.
Trials were conducted in the DRC and Guinea and showed success rates of up to 96 per cent at 18 months across both early and advanced disease stages.
“The journey was hard, difficult and challenging, especially accessing the remote areas with no internet access and poor road network where the patients live,” said Mutombo, who worked on the study.
The drug is currently recommended for adults and adolescents aged at least 12 years and weighing over 40kg.
Sanofi will manufacture and donate doses to the WHO, to be made available free of charge to patients.
What happens now?
The EMA approval paves the way for registration in endemic countries, but each country must complete its own national regulatory process. The DRC, which accounts for around two thirds of all sleeping sickness cases in Sub-Saharan Africa, is the critical first test.
Mutombo added: “We really needed to go as close as possible to the affected people so as to eliminate sleeping sickness, and Acoziborole allows us to do this.” But success, he said, will depend on securing those national registrations and maintaining disease surveillance.
Jean-Mathieu Bart, a research fellow with Guinea’s National Programme for the Control of Neglected Tropical Diseases at the Ministry of Health, told SciDev.Net: “We have seen that it is a very safe and effective drug.
“Guinea eliminated HAT as a public health problem last year. It is obvious that Acoziborole will help us accelerate the elimination of transmission by 2030.”
But he too stresses that the drug alone is not sufficient. Vector control—reducing tsetse fly populations—and community awareness remain essential alongside treatment.
“It is the combination of protect, sensitise, test and treat pillars that we will continue,” he said.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk

