By: Esther Nakkazi
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
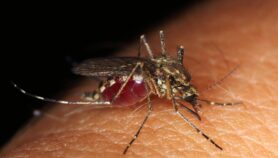
[KAMPALA] African governments are expecting a European Medicines Agency (EMA) and World Health Organisation (WHO) policy recommendation approving the first malaria vaccine candidate – RTS, S/AS01.
The final results of the phase III clinical testing showing that the vaccine, whose developers say is the most clinically advanced to date globally, could partially protect children against malaria, were published in The Lancet, in April 2015.
“We still have several steps to go. We might get a recommendation from WHO this year paving the way for national governments to accept to adopt the vaccines to be deployed by 2017,” says Lucas Otieno, a principal investigator at the Kenya Medical Research Institute (KEMRI)/Walter Reed Project in Kombewa, Kisumu County, Kenya.
“For the sake of the children, I would be very happy for an effective vaccine against malaria to become routine and cut out the suffering and death in our society.”
Shima Kaimom Gyoh, College of Health Sciences, Benue State University, Nigeria
According to the researchers, EAM will consider the safety, quality and efficacy as well as the non-bacterial meningitis and the convulsive seizures that occurred during the trial.
Mary Hamel, an epidemiologist, principal investigator at KEMRI/CDC and senior technical advisor of the malaria branch at the Center for Global Health at the CDC, says that if the vaccine is licensed, phase IV studies would follow to find out why the meningitis cases happened.
“For the sake of the children, I would be very happy for an effective vaccine against malaria to become routine and cut out the suffering and death in our society,” says Shima Kaimom Gyoh a professor of surgery at the College of Health Sciences, Benue State University, Nigeria.
“Access to this vaccine will depend on cost, stability, and an effective distribution chain. Unfortunately the poor are often right at the end of the queue,” notes Maureen Duggan, a retired paediatrician on the Healthcare Information for All (HIFA) forum.
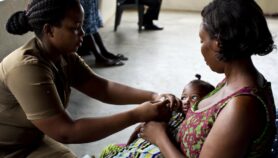
In the study, the RTS, S/AS01 malaria vaccine candidate averted 1,774 cases of clinical malaria in every 1,000 older children aged 5 to 17 months who received a booster dose and the three RTS, S/AS01 vaccines after four years of follow up.
The large phase III efficacy and safety trial enrolled 8,922 younger children (5 to 17 months) followed up for 48 months or four years and 6,537 young infants (6 to 12 months) and followed them up for 38 months.
From March 27, 2009 until January 31, 2011, they were enrolled at 11 centres in seven countries – Burkina Faso, Gabon, Ghana, Kenya, Malawi, Mozambique, and Tanzania.
Peter Waiswa, a lecturer in the department of health policy, planning and management at Makerere University’s School of Public Health and a leader for maternal and new-born health research, INDEPTH Network, urges Africa to first scale up insecticide-treated bednets, good quality medicines, and indoor spraying as better alternatives.
“Let us first concentrate on what we have because it works. When will the vaccine come? We can change people’s attitudes and make the options that are available work first,” concurs Nuwa Anthony, the technical coordinator, Malaria Consortium, Uganda.
This article has been produced by SciDev.Net's Sub-Saharan Africa desk.