Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
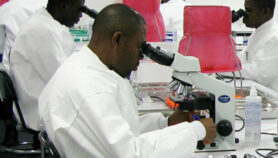
[JOHANNESBURG] The implementation of biosafety practices is being hampered by inadequate laboratory equipment and training across Africa, a conference has heard.
African countries need to develop this area so they can reap the benefits derived from biotechnology while avoiding the potential risks associated with it, according to Paul Okemo, chief executive officer of the African Biological Safety Association (AfBSA).
Speaking last week (26 June) at AfBSA’s third annual conference in Johannesburg, South Africa, Okemo said that across the continent, biological materials in laboratories continued to be carelessly handled. He blamed inadequate equipment and poor laboratory practices, such as the fact that biosafety cabinets were rarely checked for efficacy.
Governments must develop biosafety regulatory frameworks, said Julius Mugwagwa, programme officer at the African Biosafety Network of Expertise, an initiative established by the New Partnership for Africa’s Development and African Union’s Office of Science and Technology.
Of Africa’s 56 countries, only six — Burkina Faso, Egypt, Kenya, Nigeria, South Africa and Uganda — have effective biosafety policies in place, while at least 30 have no biosafety frameworks at all, or are still developing them.
Mugwagwa blamed a lack of consistent government funding, saying biosafety was not seen as a pressing concern.
"[Africa] lacks the political and social environments conducive to encouraging such practices," he told SciDev.Net. "There is a strong desire for biotechnology and its use in socioeconomic development, but a disconnection with implementing the necessary frameworks."
Another major challenge outlined by the conference was the safety of hospital patients because of poor biosafety procedures and lack of equipment.
"In some hospitals, the same gloves are used when treating multiple patients, thus transferring infective agents between patients and even to doctors and nurses," contributing to a rise in disease infections, Okemo said.
A survey conducted in 2011 by Edith Lem, an AfBSA member working at Cameroon Baptist Convention Health Institution (CBCH), which runs five hospitals and over 70 health centres, revealed that 17 out 23 laboratories in Cameroon had unacceptable health standards.
Furthermore, CBCH staff members were unable to understand or define the concept of biosafety, Lem said. And over two thirds of staff stored food and beverages in the same refrigerators as specimens.
But Lem also said measures had now been taken to implement biosafety training at these laboratories. Outgoing AfBSA president, Willy Tonui, told SciDev.Net that AfBSA’s member organisations, such as CBCH, were helping to strengthen biosafety capacity and knowledge.