13/05/21
India’s COVID-19 second wave yet to peak

By: Ranjit Devraj
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[NEW DELHI] Perhaps no experience can be as mortifying as having COVID-19 and being wheelchaired past other victims of the virus gasping for breath to the safety of a hospital room equipped with oxygen supplies.
But at that time, I needed a bed with oxygen connections fast and was too exhausted to think of the fate of those squatting on hospital floors, struggling to breathe.
Leaving the hospital on 2 May after five days of intense medication involving steroids, antibiotics, blood-thinners, oxygen and nebulisers I felt utterly drained, but glad to be alive. The new occupant was already in as I was being wheeled out. The doctors warned me to stay on saline nebulisers to prevent development of mucormycosis, a black fungus that appears to be stalking patients on prolonged oxygen and steroids. Many cases have required surgery, including for the removal of infected eyes.
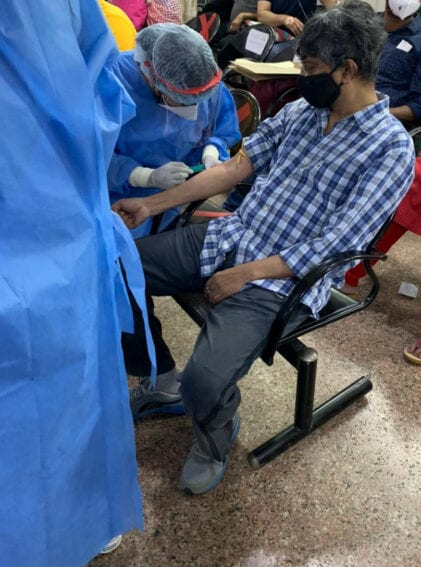
The author, Ranjit Devraj, gets his blood taken prior to being admitted in a hospital for COVID-19. Credit: Ranjit Devraj.
The government, which allowed the mass bathing rituals of Kumbh Mela in Haridwar (9 April to 8 May) and election rallies in states like West Bengal, appeared to be sending out signals that the virus had been tamed. Even now the government appears to be keener on controlling the narrative rather than the virus. People who have asked for help with emergency oxygen over Twitter have been arrested and cases have been filed against hospital administrations for putting up signs declaring shortages.
As a second wave of the COVID-19 pandemic swept across India in April and May, it was the acute lack of oxygen that exposed the totally unprepared state the country was in. The virus raged through the capital city of New Delhi and across swathes of the country, prompting lockdowns in at least 16 major states.
However, once the enormity of allowing super-spreader events for political gains came home, the central government appeared to lose its nerve and asked the states to fend for themselves — buy medicines, vaccines and the all-important oxygen supplies. Such was the chaos that the Supreme Court stepped in to form a committee of its own to supervise the distribution of oxygen across the country. Private charities have set up concentrators to fill oxygen cylinders free of charge.
Manu Raj, a leading Indian epidemiologist, says: “The message coming in from other countries was simple — there will be a lull followed by heavy downpour. If you think it’s all settled, you’ll be drowned in no time. Isolated voices from several corners warning the government against unrestricted elections and mass festivals fell on deaf ears.”
India has now recorded over 23.34 million confirmed cases and 250,000 deaths as of 12 May. Estimates suggest a trebling of mortality rates by the time the second wave is over. Roughly 3.5 million active cases need care right now with close to 9,000 in a critical state. The seven-day rolling average for new cases stands at 390,000 and for deaths is 3,886. The death count average has already crossed the 4,000 mark this week, according to Manu Raj.
But even now, top officials are already talking of a third wave.
According to estimates by the Institute for Health Metrics and Evaluation, an independent global health research centre of the University of Washington, the cumulative deaths from COVID-19 in India could reach nearly 1.5 million by 1 September.
It’s almost as if the virus was wreaking vengeance on India for daring to declare ‘endgame of pandemic’ early in March. That came as an announcement from health minister Harsh Vardhan.
Now, an overall lack of credibility has set in and the general sense is that things will get better only after they turn worse. People are also bracing for the economic devastation that will inevitably follow the current round of lockdowns.
This piece was produced by SciDev.Net’s Asia & Pacific desk.