By: Abhilasha Karkey
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Research partnerships tend to be dominated by the priorities and agendas of the global North.
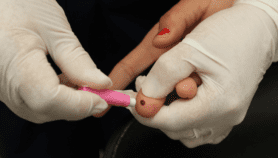
[KATHMANDU] Last year, some 200 doctors and paramedics waded through floods from overflowing drains caused by Nepal’s monsoon to vaccinate 20,000 children as part of a trial to assess the impact of a new typhoid vaccine.
The new vaccine, the first-ever that can be administered to children younger than two years of age, could potentially be rolled out as part of the national vaccination schedule to reduce the burden of this deadly diarrhoeal disease.
While vaccination can greatly reduce the number and spread of infectious diseases, having access to clean water is a cheaper and more effective solution when trying to prevent the spread of diseases in poor communities. Locally developed water filtration systems requiring no electricity or fuel are better at fighting disease, cheaper than vaccines and enable low-income households to treat and maintain the quality of their drinking water.
“Why do international health organisations prioritise vaccine development? Often, it is because the health research agenda is set by organisations outside the concerned community or those with the greatest resources.”
Abhilasha Karkey
If vaccines are expensive and target only one disease at a time, why do international health organisations prioritise vaccine development? Often, it is because the health research agenda is set by organisations outside the concerned community or those with the greatest resources. To people who grew up with consistent access to clean drinking water, local water filters are not top of mind.
Global North dominates research agendas
The global scientific community is heavily dominated by high-income countries with resources, researchers and scientific publications. This gap remains despite a dramatic rise in collaborative global health research over the last two decades. The result is that researchers, donors and governments from the global North act on their own priorities, interests and budgets. Due to pervasive inequalities, researchers from low-income countries do not have an equal voice in shaping research agendas.
The well-intentioned but misguided focus on universally applicable technological solutions often come at the expense of simpler tools that meet the unique needs of a developing country. Further, talented local researchers are pushed to follow international agendas instead of local needs. The gatekeepers at scientific publications and funding groups are overwhelmingly from rich countries and, because of previous scientific discoveries or publications, play a significant role in securing research funding.
A popular approach to bridging this gap has been to send more scientists from wealthy countries to work in poorer parts of the world. These researchers, working closely with local partners, gain knowledge and experience while also boosting the capacity of their poor country partners. This kind of partnership can be powerful, but it requires humility.
Researchers from the North must appreciate that language and cultural barriers can lead to fundamentally different interpretations of the same data. They must also view their local collaborators as true partners, as there have been instances where a local collaborator had concerns about interpretations offered, but did not know how to raise objections (or if they could be raised) to their international counterparts.
Frustration over this power imbalance results in local researchers declining to take part in future research projects with international researchers. This threatens to bring successful global health research networks to a grinding halt, just as we need to address new and re-emerging global diseases.
Avoid ‘parachute science’
To improve the long-term health of the global population, we need more than long-term technical, scientific and material support — we need trust and respect in local collaborations. We must also move away from ‘parachute science’ in which investigators from developed countries merely collect samples and data, return home and publish papers. This presents no opportunity for a two-way discussion with local collaborators. To prevent this, collaborators should share information, analysis and drafts of manuscripts prior to publication.
True international collaboration requires investment of time from all participants. Balanced agendas interest both partners, and it is, therefore, imperative that Southern partners are able and willing to collectively assess their own needs and advocate their priorities. While scientists from the North can contribute in terms of knowledge, technologies and resources, in return they can gain from local expertise and knowledge of diseases.
Better and deeper collaboration is essential if we want to tackle some of the most stubborn threats to health globally. But it has to start before a study or trial launches. We need collaboration even when decisions are being made to identify the most pressing challenges and the most useful tools to tackle these challenges in a local context. While we vaccinate, we also need to take care of the overflowing sewage systems. We need solutions that work for those who need them the most.
Abhilasha Karkey, medical microbiologist and vice-director of the Oxford University Clinical Research Unit-Nepal, has worked extensively on the growing problem of antimicrobial resistance and has conducted studies on the epidemiology and evolution of enteric fever.
This piece was produced by SciDev.Net’s Asia & Pacific desk.