03/02/21
Drug cocktail tested on extremely drug-resistant TB

By: Neena Bhandari
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[SYDNEY] A new three-drug, all-oral, six-month treatment is providing hope to patients in Tajikistan with highly drug-resistant forms of tuberculosis, which until now had limited treatment options and poor prognosis.
Tajikistan is the first country in Central Asia and second in the world after Ukraine to provide access to the novel ‘BPaL’ regimen to patients suffering from the extensively drug-resistant (XDR-TB) form of tuberculosis under operational research conditions from December 2020. The regimen consists of three drugs — bedaquiline, pretomanid and linezolid.
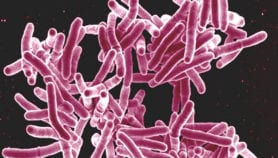
XDR-TB is caused by bacteria resistant to some of the most effective anti-TB drugs and these strains develop from mismanaged treatment of patients with multidrug-resistant TB (MDR-TB).
“The BPaL regimen offers the shortest possible treatment course for XDR-TB patients, excludes injectable drugs, is easy to use and more affordable,” says Veriko Mirtskhulava, senior epidemiologist at KNCV Tuberculosis Foundation, an international NGO devoted to eliminating TB.
“Conventional treatment regimen for patients with XDR-TB consists of 7—8 antibiotics for a minimum of 18 months, including any of the injectable drugs, which not every patient can tolerate.”
The BPaL regimen, developed by the non-profit organisation TB Alliance, is being implemented in Tajikistan by the National Tuberculosis Programme with support from the KNCV Tuberculosis Foundation.
“As the regimen is still a novel anti-TB treatment, it is essential to closely monitor its feasibility, acceptability, safety and effectiveness, and ensure systematic and standardised data collection,” Mirtskhulava tells SciDev.Net.
“Tajikistan has the human resource capacity and infrastructure for it. After analysing the operational research data on the regimen’s safety and effectiveness, a decision will be made about scaling up the BPaL treatment under regular health service delivery conditions.”
While TB is preventable and mostly curable with early detection and proper treatment, conventional drugs do not work in drug-resistant strains of TB. MDR-TB is resistant to the two most powerful first-line TB drugs— isoniazid and rifampicin. In addition, XDR–TB has resistance to second-line TB drugs — any fluoroquinolone and any of the three injectable drugs— amikacin, capreomycin and kanamycin.
According to the World Health Organization, there was a ten per cent increase in MDR-TB in 2019 compared to the previous year, and the cure rate of XDR-TB worldwide is only 43 per cent. However, the BPaL regimen has shown success in treating 90 per cent of XDR-TB patients in TB Alliance’s Nix-TB trial, which was conducted at three sites in South Africa. The results were published in the New England Journal of Medicine last year.
“We now have preliminary evidence that with the right drugs and drug regimens, highly resistant forms of TB might be able to be treated with similar number of drugs and similar duration as that needed for the treatment of drug sensitive TB”
Sandeep Juneja, TB Alliance
“We now have preliminary evidence that with the right drugs and drug regimens, highly resistant forms of TB might be able to be treated with similar number of drugs and similar duration as that needed for the treatment of drug sensitive TB,” says Sandeep Juneja, TB Alliance’s senior vice-president of market access.
The BPaL regimen was first approved in August 2019 in the US and it has been recommended by the WHO under operational research conditions. Many more countries are expected to begin operational research soon including South Africa and Nigeria, as well as through efforts like the TB Alliance’s LIFT-TB programme, which is supported by South Korea, enrolling patients in Indonesia, Kyrgyzstan, Myanmar, The Philippines, Uzbekistan and Vietnam.
“Our priority is to rapidly enable the widespread rollout of the BPaL regimen to those in need, no matter where they live. For countries where pretomanid is not yet approved, our global commercialisation partner Viatris has established a named patient access programme,” Juneja tells SciDev.Net.
All three drugs in the regimen are available to approximately 150 low- and middle-income countries through the Stop TB Partnership’s Global Drug Facility at a cost of under US$1,000 per six-month treatment course.
“The approval of this regimen [under operational research conditions] is a major step forward for people affected by XDR-TB. However, there is an urgent need for the scale up of laboratory capacity to test for resistance to these newer drugs. A recent small study from South Africa has already found worrying levels of resistance to bedaquiline in rifampicin- resistant TB,” says Khai Lin Huang, infectious diseases physician at the Burnet Institute in Melbourne, Australia.
Khai Lin tells SciDev.Net that resistance to antimicrobials will almost certainly occur with increasing use, but the risk and impact can be managed with appropriate systems in place.
“Currently, the evidence for the BPaL regimen comes from a single trial in a single country, but more experience and data are needed. It is important that countries have a framework and capacity to be able to conduct operational research and adapt quickly,” he adds.
Ending the TB epidemic by 2030 is among the health targets of the UN’s Sustainable Development Goals. Globally, 1.4 million people died and an estimated ten million people, including 1.2 million children, fell ill with TB in 2019. Eight countries accounted for two-thirds of the total new cases, with India leading the count, followed by Indonesia, China, the Philippines, Pakistan, Nigeria, Bangladesh and South Africa, according to WHO.
This piece was produced by SciDev.Net’s Asia & Pacific desk.