By: Fatima Arkin
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
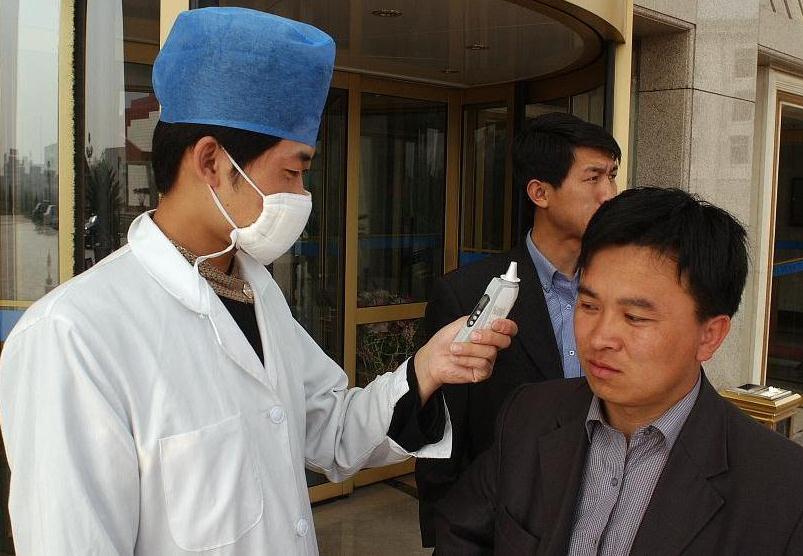
[SEOUL] The lack of capacity in many South-East Asian healthcare systems could exacerbate the ongoing MERS outbreak in South Korea, say observers.
The large number of migrants and travellers in the region means South Korea may not be able to contain MERS (Middle-East respiratory syndrome), whose rapid spread across the country was only revealed this week.
China, India, the Philippines and Singapore have issued alerts to their border staff and health workers because of the many tourists, businesspeople and economic migrants travelling to or through South Korea.
“This is a very critical issue,” Daesub Song, a specialist on MERS in South Korea and a microbiologist at Korea University, tells SciDev.Net. “I was really worried about the Korean government’s response. They underestimated the transmissibility of the MERS virus and were not prepared for it.”
“Because of the living conditions and the number of people in close contact, this can obviously be a big problem.”
Mike Osterholm, Center for Infectious Disease Research and Policy, University of Minnesota in the United States.
From January to March, for example, more than 361,000 South Koreans went to the Philippines on holiday, according to the Philippine’s tourism department. South Korea’s government only revealed details about the outbreak on 7 June, even though the first diagnosis was made more than two weeks earlier.
“We are all very concerned about the potential for MERS to spread in the Philippines,” says Rontgene Solante, a doctor at the San Lazaro hospital in Manila, which specialises in infectious diseases. “If MERS did spread in the country, we would definitely not be properly equipped in all aspects of MERS containment.”
Migrants in poorer South-East Asian countries are especially vulnerable, since they often lack access to local health systems, which may already be struggling to care for their own citizens. In addition, many are not registered with local authorities and live in slum conditions where the virus could spread rapidly, according to healthcare authorities.
“Because of the living conditions and the number of people in close contact, this can obviously be a big problem,” says Mike Osterholm, an epidemiologist and the director of the Center for Infectious Disease Research and Policy at the University of Minnesota in the United States.
Arguably, however, rural communities have been at greater risk of contracting and transmitting MERS. The disease emerged in 2012 in Saudi Arabia and many of those first infected were camel herders and people who visited camel farms or drank unpasteurised camel milk.
A scientific study of MERS published in The Lancet this April, found that the virus spread quickly to the Saudi Arabian city population, which had less resistance due to a lower exposure to camels. The virus then moved to many other Middle Eastern countries through international travel.
The virus causes symptoms similar to bronchitis and can be deadly — the South Korean outbreak had already killed 11 people when this story went online.
As the MERS outbreak continues, health NGOs and watchdogs have urged governments and international agencies to provide more robust preventative measures to protect rural and poor communities from the disease.
Last week, the World Health Organization published a list of recommendations that healthcare centres with only basic facilities can implement, such as changing and disinfecting bedsheets, cleaning floors and equipment regularly and improving clinical waste management.