By: Fatima Arkin
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
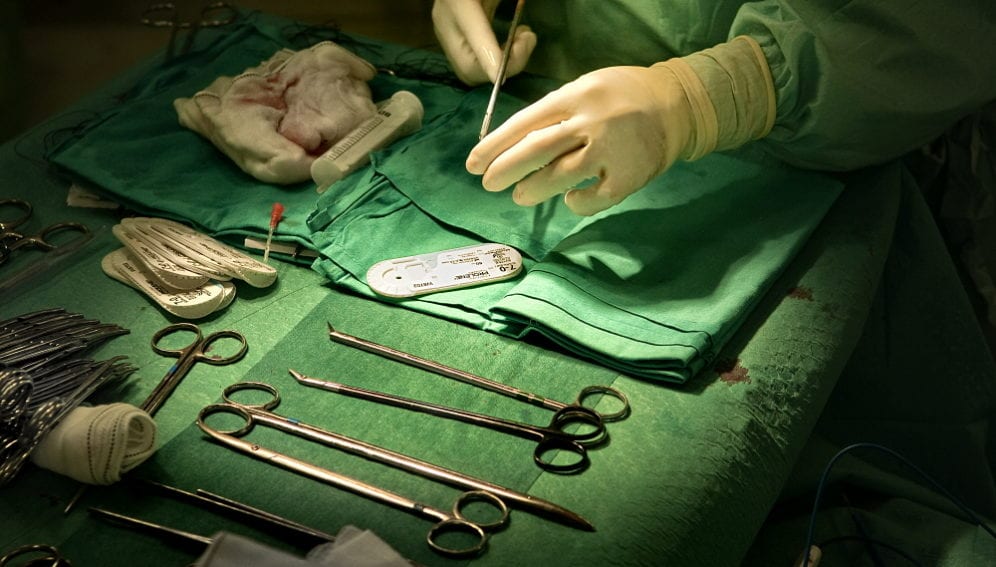
[MANILA] Basic surgeries such as delivering babies via caesarean section are some of the most cost-effective health measures in developing countries, potentially averting 1.5 million deaths each year.
“There are people who still equate surgery with expensive tertiary care but the data show otherwise,” says Haile Debas, a surgeon and one of the editors of Essential Surgery, the first of nine volumes of the disease control priorities series published last month (24 March) by the World Bank Group.
The book lists 44 operations as crucial to developing countries, including cataract surgery, in which advances largely came from those very countries, says Debas, who is also founding director of the University of California Global Health Institute.
Debas tells SciDev.Net that in India alone, the Aravind Eye Care System — a network of hospitals, factories, research institutes and community outreach efforts — performs roughly 60 per cent as many eye surgeries annually as the UK National Health System, at one-thousandth of the cost.
Aravind is able to do this partly by making payments voluntary and enabling paying patients to subsidise non-paying ones, while still paying substantially less than they would at other Indian hospitals.
Debas hopes decision-makers in developing countries will make surgical services a priority. Many of the 44 operations listed in the book can be done in district hospitals, which are cost effective because of the assistance of other health professionals and nurses as well as the patients’ families who bring food to their sick members.
Investing in surgical services also has unexpected yet positive spillover effects. “The quality of care in those hospitals improve because there are more activity, more equipment, more personnel, better infection control, and so on,” adds Debas.
Debas says that developing countries need to address the deficit in the surgical workforce and to form more alliances with healthcare professionals, health NGOs and universities in the developed world.
But Jose Acuin, a clinical epidemiologist at the Asian Hospital and Medical Center in the Philippines, tells SciDev.Net that when it comes to surgeons and anaesthetists in his home country, “it’s not just a problem of quantity, but also of geographic distribution and accessibility”.
One resource that Acuin sees a lot of potential is telemedicine: the use of satellite technology, video conferencing and data transfer through phones and the internet to connect doctors to patients located far away.
But while the cost of telemedicine has gone down and made inroads in some South-East Asian countries like Malaysia and Singapore, he says medical professionals in the Philippines are nervous about making a decision on a patient they have not really seen. Another challenge is the absence of electronic medical records.
Still, Acuin sees that in ten years’ time, telehealth will have “already arrived” and hopefully brought along with it, increased access to essential surgeries.
>Link to the book in Open Knowledge Repository of the World Bank
This article has been produced by SciDev.Net's South-East Asia & Pacific desk.