By: Heng Min Sern
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[SINGAPORE] Babies exposed to hepatitis B virus (HBV) in the womb have a more developed immune system against bacterial infections than babies born to healthy mothers, says a Singapore-led study.
The surprising result showed that while causing diseases later in life, HBV might actually be helpful in early life, according to scientists based at the Duke-National University of Singapore (NUS) Graduate Medical School in a study published in Nature Communications (25 March).
Hepatitis B is one of the world’s most common and serious infectious diseases, affecting about one-third of the population, mostly in Asia. A quarter go on to develop serious liver diseases, causing about a million deaths each year.
Previously, it was thought that infants born from mothers with HBV are immune tolerant to HBV, which means they have no protective response to the virus and are unable to react to treatment.
However, failure of this hypothesis to explain, among other things, the efficacy of HBV vaccination in infants born to HBV positive mothers prompted researchers to investigate further.
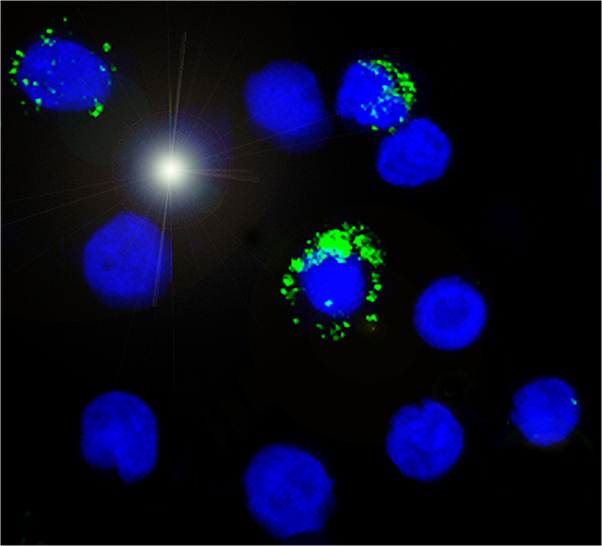
The research team looked at umbilical cord blood taken from new born child in HBV positive mothers and found cytokine (proteins produced by immune cells to regulate immune responses) profiles similar to those found in the blood of mature adults.
Their findings indicated that exposure to the virus in the uterus induces a phenomenon called “trained immunity”, which is when innate immune cells display adaptive characteristics, and are more activated and mature, responding better to bacteria challenge.
The study raises questions whether current treatment practices are the most effective approach to combatting the disease. Currently, treatment is focused on those who experience active liver disease as a result of the infection, which usually occurs past the age of 30.
But Michelle Hong, a co-author of the paper, says that in an earlier study by their same research group, they found chronically infected adolescents did not display tolerogenic T cell features (capable of producing immunological tolerance), and in fact had an active immune profile.
“This indicates that you could consider starting the treatment programme much earlier instead of later, if they already have a protective immune response against the virus, and just need a boost,” Hong says.
Stephen Locarnini, a medical professor and co-chair for the Coalition to Eradicate Viral Hepatitis in Asia Pacific (CEVHAP) tells SciDev.Net: “The study completely reverses current thinking on the relationship between human hosts and the hepatitis B virus.”
“That isn’t to say that HBV exposure is ‘desirable’ from a public health perspective,” he explains. “Mother-to-child is the most prominent mode of transmission in Asia, which means many infants in Asia are at risk of being infected with HBV that can have life-long consequences on health if the newborn does not receive vaccination at birth.”
“As such, universal infant immunisation programmes are critical,” Locarnini stresses.
He adds that while the paper is an important study challenging the current concepts on hepatitis B pathogenesis, “it won’t necessarily impact on current treatment guidelines per se, but may in the medium term have an impact on how treatments could be shaped.”
>Link to full paper in Nature Communications
This article has been produced by SciDev.Net's South-East Asia & Pacific desk.
References
Nature Communications doi: 10.1038/ncomms7588 (2015)