By: Neena Bhandari
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[SYDNEY] Doctors treat and heal patients, but they are seldom seen as people who may themselves require care or accommodation. Medics with disabilities are now calling for a paradigm shift in this mindset to make medical education and the profession more inclusive.
“Being a doctor is a privilege. We have the opportunity to play a part in a person’s most significant of journeys. We have the sacred trust of the public. We have also been thought leaders on many historical issues. For these reasons the medical profession needs to lead the way in inclusivity,” says Dinesh Palipana, a Sri Lanka-born Australian doctor who was left severely disabled after a road accident.
“Being a doctor is a privilege. We have the opportunity to play a part in a person’s most significant of journeys. We have the sacred trust of the public. We have also been thought leaders on many historical issues. For these reasons the medical profession needs to lead the way in inclusivity”
Dinesh Palipana
The understanding and evaluation of disability, in recent years, has moved away from a physical or medical perspective. The UN Convention on the Rights of Persons with Disabilities (UNCRPD) recognises that “disability results from the interaction between persons with impairments and attitudinal and environmental barriers that hinders their full and effective participation in society on an equal basis with others”.
Disability includes having an impairment, such as difficulty in seeing, hearing, walking, or problem solving, which results in participation restrictions in normal daily activities, such as working, engaging in social and recreational activities.
As many as 690 million people, accounting for 15 per cent of the total population in the Asia Pacific region, live with some form of disability, according to the UN Economic and Social Commission for Asia and the Pacific (UNESCAP). Persons with disabilities were two to six times less likely to be employed compared with other people.
Dearth of data
There is a dearth of specific data on the prevalence of disability in the medical profession. “We’ve checked across multiple technical departments in WHO and we do not hold data on doctors and medical personnel with disabilities. Also, WHO does not have guidelines on this specific issue,” a WHO spokesperson tells SciDev.Net. via email.
Apart from the lack of guidelines, pervasive underlying biases, prejudicial attitudes and misconceptions about disability may be hampering education and employment opportunities for the disabled in the field of medicine.
Medicine tops the list of most respected professions, followed by law and engineering, according to research conducted by the global education charity Varkey Foundation, which surveyed a thousand members of the general public in 35 countries in 2018.
“Our workforce needs to reflect the diverse society that we serve. This approach will not only make the medical profession richer but also encourage other areas of our society to celebrate inclusivity,” says Palipana as he prepares to begin another busy night shift as senior resident in the emergency department of Gold Coast University Hospital in Australia.
“Our workforce needs to reflect the diverse society that we serve. This approach will not only make the medical profession richer but also encourage other areas of our society to celebrate inclusivity”
Dinesh Palipana
Palipana was in the third year of medical school when he lost the use of his lower body and hands in a car accident. “You can’t become a doctor” was a refrain he repeatedly heard. The disheartening remarks only strengthened his resolve to follow his passion. To recuperate from his injury, he returned to Sri Lanka where he began raising awareness and funding for spinal cord injury.
After nearly five years of hospitalisation and rehabilitation, he returned to Griffith University’s School of Medicine, Australia, in 2015. Some of his colleagues, now his seniors, accepted his new reality, but others treated him as inferior and ignored or even bullied him.
“There were confronting moments, but my new peers were welcoming and supportive,” says Palipana. He found it extremely difficult to get an internship, a guaranteed position for a medical student. “If you find your own money we could have you as an extra,” he was told.
“Hospitals were reluctant to have a quadriplegic doctor as a resident. It took a lot of advocacy to get a placement. My mother was my rock during this very challenging time,” says Palipana, who today sits on the council of the Sri Lanka Spinal Cord Network and is a founding member of Doctors with Disabilities Australia, an advocacy group for physicians with disabilities.
Doctors who become disabled while in medical school face several obstacles in medical practice. Samitha Samanmali, a bright third-year medical student in Colombo, Sri Lanka, was arranging a faculty exhibition at a conference hall when a stall collapsed on her in February 2008. She sustained a spinal cord injury that left her partially paralysed.

Samitha Samanmali. Image credit: Samitha Samanmali.
With grit and support from her family and friends she resumed her studies approximately ten months after the accident and completed her post-graduation in community medicine. Her colleagues were helpful, but she found it nearly impossible to work effectively in a clinical setup.
Lack of accessibility
“I was working at a national hospital where it was difficult to manoeuvre my wheelchair in the narrow space between the beds in the ward. Also, the beds couldn’t be lowered to the wheelchair level, so I found it difficult to examine patients,” says Samanmali, whose biggest challenge continues to be lack of accessible toilets even in health institutes.
“My choice of work is dictated not by my preference for the job, but accessibility. I had to give up my aspiration to be a practicing physician and moved to public health,” says Samanmali, who now works at the Ministry of Health’s Youth, Elderly and Disability Care Unit. She enjoys her current job which involves preparing guidelines, policies, awareness and advocacy programmes.
Hospitals generally sprawl over different levels and large areas, which can pose a challenge for doctors with disabilities. In many developing countries, elevators often do not work due to power shortages, doors are not automated and the ramps are dirty and crowded.
Romi Syofpa Ismael, who completed her dentistry course at the Universitas Baiturrahmah, Indonesia, was three years into the profession when she had paraplegia following a Caesarean section. She was posted to a remote community health centre in South Solok Regency in Indonesia’s West Sumatra Province, where only a narrow dirt road linked her home to the centre.
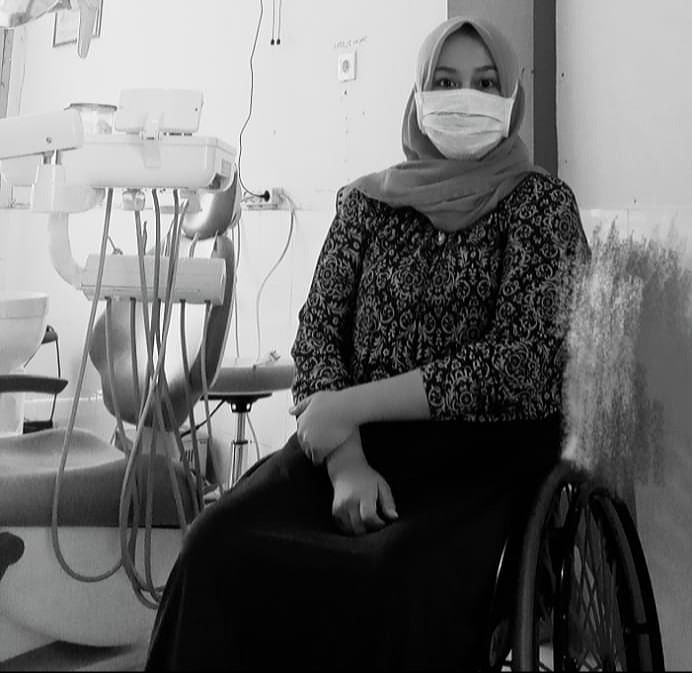


Romi Syofpa Ismael. Image credit: Romi Syofpa Ismael.
“It required a lot of effort to roll the manual wheelchair, especially during rains when the path would turn muddy and dangerously slippery,” says Ismael, who was shocked when, in 2018, despite achieving the highest score in the country’s coveted civil service test, she was rejected on grounds of disability.
Rejection on grounds of disability
In Indonesia, a dentist is ineligible to work if she/he has severe impairment in the upper body under the 2006 Indonesian Medical Council guidelines. As Ismael’s disability was in the lower body, she could not be disqualified according to the same guidelines.
“I had to really fight for my rights. Finally, at the behest of the central government, my position as a civil servant was restored by the local government,” adds Ismael, who is now working in a more accessible general hospital in South Solok Regency and also runs her own private dental practice.
Indonesia’s disability prevalence rate of 8.6 per cent is the highest in South-East Asia (UNESCAP 2019), accounting for over 21 million persons with disabilities, according to the Indonesia Convention on the Rights of Persons with Disabilities State Report, 2017.
Some doctors, who had a disabling disease early in their childhood, were motivated by their own disability and parents’ encouragement to pursue a career in medicine. They have taken their physical limitations in their stride.
“When you are a doctor, your own disability is never a consideration. It is about giving the best care and treatment to your patients,” says Anjani Kumar Sharma, who had poliomyelitis in his left lower limb before his first birthday. He has been able to work 12 hours a day for over three decades.
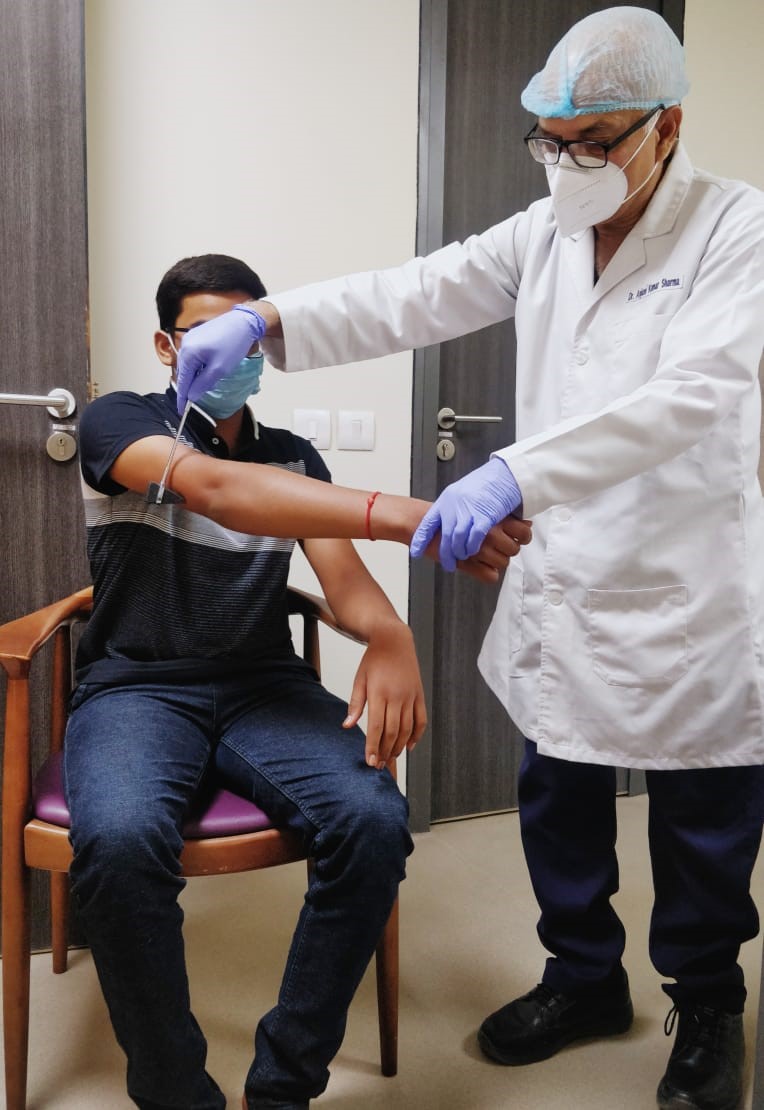


Anjani Kumar Sharma. Image credit: Anjani Kumar Sharma.
“I was not treated any differently by my peers, seniors or patients in teaching or clinical side of the medical profession,” says Sharma, who is director of neurosciences at the CK Birla Hospital in Jaipur, India.
Echoing similar sentiments, Paresh Kumar Sukhani, a professor in the department of radiology at the Mahatma Gandhi Medical College and Hospital, Jaipur, says, “In India, in recent years even the nomenclature for ‘disabled’ has changed to ‘specially-abled’. This enthuses respect rather than sympathy for disability.”
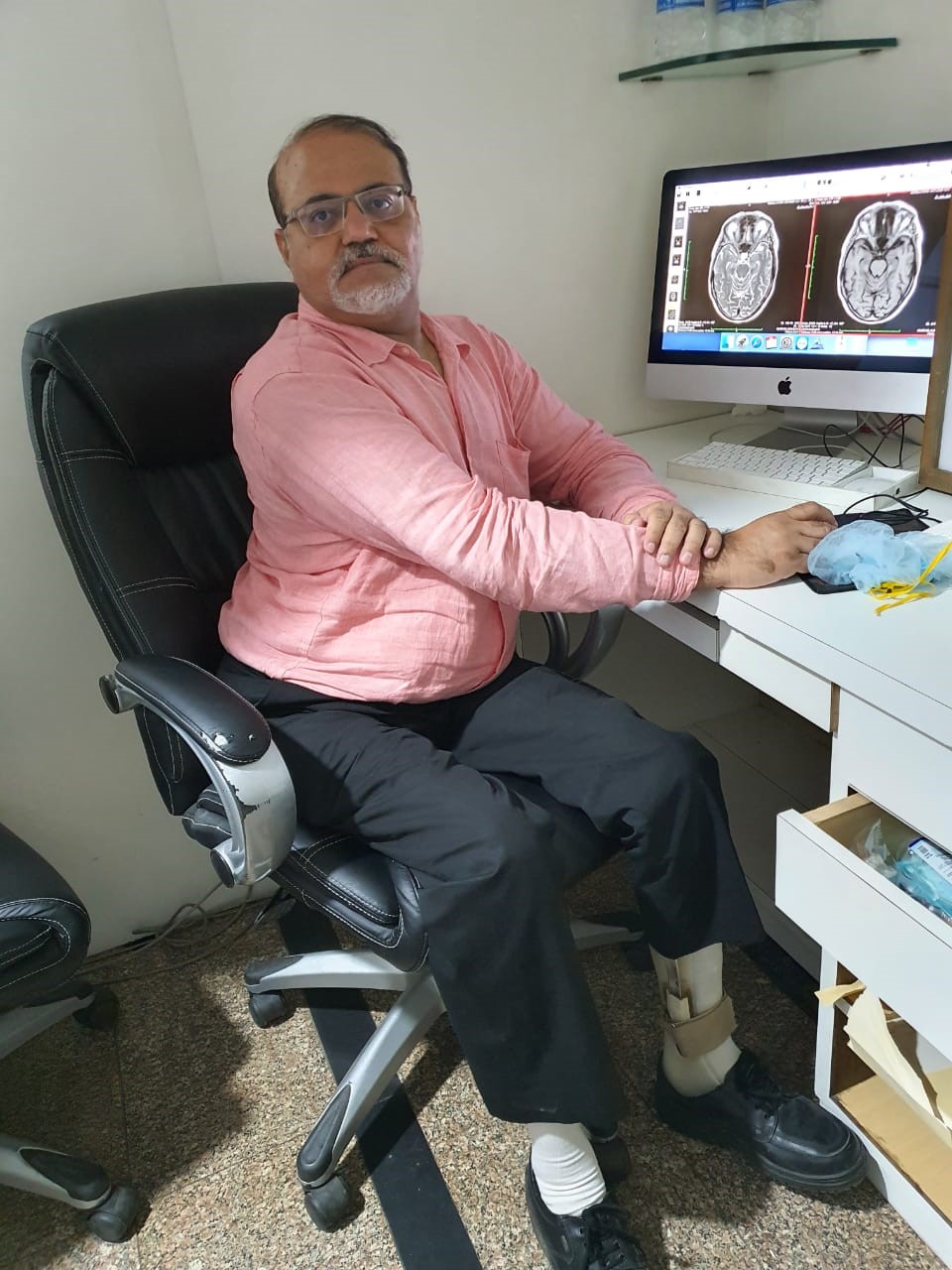


Paresh Kumar Sukhani. Image credit: Paresh Kumar Sukhani.
When Sukhani, who suffers from paraparesis or partial paralysis of the lower limbs, joined Jaipur’s Sawai Man Singh Medical College in 1986, there were four other students with disabilities in his batch.
Grace Anne Herbosa, chair of the Department of Anesthesiology at University of the Philippines College of Medicine in Manila, notes that during her 35 years of service she has not come across any case of discrimination against doctors with disabilities.
“In the anesthesia community, we have resident doctors with polio who finished residency as their physical disabilities did not compromise patient safety. We have an anaesthesiologist who recently had a stroke, he now works with an assistant,” Herbosa tells SciDev.Net.
Disparities in education
Disparities in education play a major role in the absence of doctors with disabilities in the profession, Charlotte McClain-Nhlapo, global disability advisor to the World Bank Group, Washington DC, tells SciDev.Net.
“Medical schools need to be more inclusive in their intake of students — including those with disabilities, and they also need to have more expertise and better teaching on the medical needs of persons with disabilities. This needs to be accompanied with the practice of medicine being appropriately equipped with accessible medical devices and instruments and overall being more disability inclusive,” adds McClain-Nhlapo.
“Medical schools need to be more inclusive in their intake of students — including those with disabilities”
Charlotte McClain-Nhlapo, World Bank Group
In 2019, there were a total of 437 medical graduates in three medical schools in Singapore. “Regrettably, all three medical schools do not have an inclusive policy on the admission of persons with disabilities for training as medical doctors,” says Lim Puay Tiak, chair, ASEAN Disability Forum, and board member, International Disability Alliance.
Some South-East Asian countries have reservations or quotas for people with disability in employment and education. For example, Indonesia’s Law on Disabilities ensures the right to work for persons with disabilities with a quota system.
“However, these are not typically related to specific courses and I am not aware of designated places for students with disability to enrol in medicine and surgery,” says Nathan Grills, an international expert on public health and disability inclusion at University of Melbourne’s Nossal Institute for Global Health in Australia.
“In fact, quite the opposite. Many countries, for example Australia, India, Thailand and Fiji have excellent anti-discrimination laws, but there are many exemptions and clauses around what is ‘reasonable accommodation’ and ‘fitness to practise.’ Often, implementation of such laws, and admission into medicine, depend on the persons with disability themselves taking on large bureaucracies and institutions,” Grills tells SciDev.Net.
Regulations and laws
The Asian and Pacific Decade of Persons with Disabilities, running from 2013 to 2022, is guided by the Incheon Strategy to ‘Make the Right Real’ for Persons with Disabilities in Asia and the Pacific, building on the UNCRPD and supporting the achievement of the 2030 Sustainable Development Goals Agenda.
In India, the Medical Council of India screens for disabilities at the entry level for graduate and post-graduate medical education. A set of 21 medical conditions have been recognised as stipulated in the Rights of Persons with Disabilities Act 2016.
However, Sharad Philip, a practising psychiatrist in Bangalore, India, tells SciDev.Net, “It’s like I slipped through the cracks as an anomaly because the whole set of restrictions does not account for those with progressive health conditions.”



Sharad Philip. Image credit: Sharad Philip.
He has retinitis pigmentosa in both eyes. The degeneration in this rare, inherited eye disease progresses over time and can lead to blindness. His visual disability is 70 per cent and is permanent. Philip notes that this degenerative progression can also be seen in persons with multiple sclerosis, Wilson’s disease, blood disorders and other diseases.
“Disability here is synonymous with impairment. Hence, fitness is determined as an inverse of the extent of impairment. This is in itself regressive and not in keeping with the UNCRPD and the International Classification of Functioning, Disability and Health. The situation is similar in all South Asian countries,” he adds.
Invisible disabilities
Besides obvious physical disabilities, there are many doctors with “hidden” disabilities, such as diabetes or Crohn’s disease. “Unfortunately, in most developing countries, doctors with disabilities are more likely to conceal their disability due to stigma and discrimination, particularly if it is an invisible disability,” says McClain-Nhlapo.
The challenges doctors with disabilities face are not a developing country problem alone, but they exist in developed countries as well.
A leading expert on disabilities in medical education and assistant professor of family medicine at the University of Michigan Medical School, Lisa Meeks says: “Despite best efforts for reform and positive changes happening in the US, there are still reports of discrimination at every level (students, residents/trainees and physicians in practice). Our colleagues across the country are fighting to eradicate the stigma and stereotypes that lead to this way of thinking.”
Reasonable accommodation, assistive technologies
In the age of high tech gadgetry and modern medicine, doctors with disabilities can have a rewarding career with appropriate support and reasonable accommodation, which refers to modifications, supports or changes in the work environment or in the way a job is performed that enables an employee with a disability to equal employment opportunities and benefits.
Vera Krejcik, who had completed medical school in Calgary, Canada, and was about to begin training in internal medicine, had a stroke following the neurosurgical removal of an arteriovenous malformation. It led to left-sided hemiparesis or weakness on one side of the body.



Vera Krejcik. Image credit: Vera Krejcik.
When she returned to training after two years, she found it challenging to accept that she needed special treatment. She had to advise around possible accommodations, for example, doing overnight calls was unsafe for her and patients because of her seizure disorder, the lack of use of her left hand and difficulty in walking quickly. So she decided to move from internal medicine to psychiatry where her physical limitations were less of a challenge.
“Early in my training, I had to advocate for myself at every step as there was considerably less in place at the time (2013). As a newly practicing psychiatrist, however, I am able to build a practice that allows me and my patients to flourish, but this is not the case for many, if not most, physicians with disabilities in Canada,” Krejcik tells SciDev.Net.
There are also doctors who have adopted their own strategies and adapted tools and machines to cope with and overcome their impairment. For example, Palipana has trained himself to manoeuvre his fingers around a stethoscope and uses the part of his hand that has sensation to examine patients.
Assistive technologies, such as adjustable hospital beds and chairs, customised stethoscopes and dental units, power-assisted manual wheelchairs, standing and electric wheelchairs, smart crutches, voice recognition recorders, dictation software, aids for sensory impairments, option of robotic surgeries are some of the many advancements making a difference.
Perceptions and attitudes
“I feel the macho image that doctors of the past felt they had to live up to – to never take a day off sick and to just keep going whatever the cost – is definitely on its way out, so that’s a good thing,” says Elizabeth Ferris, Foundation Doctor in Dundee, UK, who was paralysed waist down following a spinal cord injury during her second year of undergraduate study.



Elizabeth Ferris. Image credit: Elizabeth Ferris.
“It is about perceptions and attitudes and not the practicality of being a doctor — which can be a challenge sometimes. When people see me as a doctor on wheels and not heels, there is a raised eyebrow or a nod as if asking, “Are you serious?” But when I am with a stethoscope around my neck, patients are very receptive and allow me to do my job,” Ferris tells SciDev.Net.
Patients are occasionally curious and probing, but generally kind and encouraging to doctors with disabilities. As Palipana says, “They probably feel that our lived experience of injury and disability has made us more compassionate towards their pain and suffering.”
COVID-19 driving groundswell for change
The main advocates of making medicine more inclusive have been support groups, for example, the Canadian Association of Physicians with Disabilities (CAPD), which has about 150 members.
CAPD president and co-chief, Public Health and Preventive Medicine at Cumming School of Medicine in Calgary, Canada, Franco Rizzuti says: “There has been a groundswell within the national and global medical community to think about accommodations and inclusivity within medicine. This started with gender, then Black, Indigenous and people of colour, and it is now beginning to include (dis)ability. COVID-19 has accelerated this thinking.”



Franco Rizzuti. Image credit: Franco Rizzuti.
“I think we are at an inflection point within medicine and we are going to see a reconceptualisation of how health care is provided, and how physicians do so,” adds Rizzuti, who has L4-5 disc injury with herniation and suffers from chronic pain with neurologic symptoms in both legs. He had initially faced a lot of stigma and difficulty seeking accommodation to complete medical school.
In India, Satendra Singh, associate professor at University College of Medical Sciences in Delhi, has been advocating for disability rights and justice through Doctors with Disabilities: Agents of Change, a support group he founded in 2015.
“Personally, I take pride in my disabled identity. We can be our own role models. When people see doctors with disabilities excelling, and as our fraternity grows, the biases and prejudices prevalent in society will eventually disappear,” says Singh, who has poliomyelitis in his right leg and walks with the aid of a Knee Ankle Foot Orthosis or long calliper and crutches.
This piece was produced by SciDev.Net’s Asia & Pacific desk.
References
World Health Organization, International Classification of Functioning, Disability and Health (ICF) external icon. Geneva: 2001, WHO.