06/04/21
Hospital superbug traced to remote island beach

By: Ranjit Devraj
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[NEW DELHI] Researchers confirmed the presence in the wild of Candida auris, a multidrug-resistant fungus commonly found infesting hospitals. The findings could provide scientists insights into a pathogen that threatens inpatients, including those being treated for COVID-19.
Bursting onto the medical scene a decade ago, C. auris is now recognised as a ‘recently emerged multidrug-resistant fungal pathogen’ that causes severe infections in hospitalised patients, said the study. However, the origins of C. auris in nature and its rapid acquisition of multidrug resistance have remained a mystery.
Significantly, samples taken from the salt marshes and beaches of India’s remote Andaman and Nicobar Islands, in the Bay of Bengal, showed up both multidrug-resistant and drug susceptible isolates of C. auris, according to the study, published March in mBio. The samples from the ‘wild’ establish C. auris as an environmental organism.
Anuradha Chowdhary, professor of mycology, Vallabhbhai Patel Chest Institute, University of Delhi, and corresponding author of the study, says that while C. auris isolates found on the beach were multidrug-resistant, those found in the remoter salt marshes of the Andaman islands were not resistant to ordinary anti-fungal drugs.
“So far, no environmental studies to explore the presence of C. auris outside hospital settings have been conducted — this study will prompt future studies in different geographical areas to undertake screening for C. auris,” Chowdhary tells SciDev.Net. “Isolation of the yeast in the tropical, coastal environment suggests that it has an association with the marine ecosystem.”
“This study will prompt future studies in different geographical areas to undertake screening for C. auris”
Anuradha Chowdhary, University of Delhi
“In hospital settings C. auris is typically found in immunocompromised patients under prolonged admission and those requiring the use of invasive devices such as catheters, feeding and breathing tubes are especially vulnerable to infections by the fungus or yeast,” says Chowdhary.
Dinesh Raj, consultant at the Holy Family Hospital, New Delhi, and medical researcher tells SciDev.Net that C. auris is increasingly being found in intensive care units of hospitals in India. “This is a matter of grave concern in the current COVID-19 pandemic. Among the severe cases of COVID-19, about two-thirds of hospitalised patients who develop C. auris fungemia do not recover.”

According to Chowdhary, it is vital to strictly implement hospital infection control strategies to curtail infections with C. auris. “Thorough screening of patients and their environment is required as also cohorting (putting together) of patients who are colonised by C. auris — since they continuously shed viable yeast cells from their skin and contaminate hospital environments.”
Chowdhary says that because COVID-19 patients tend to develop respiratory distress that requires mechanical respiratory support, this opens the way to secondary infections.
“Even before the arrival of SARS-CoV-2, C. auris was considered a major global health threat due to high rates of drug resistance and ease of transmission in hospital settings. Indeed, multidrug resistant C. auris has been reported from over 40 countries across six continents since its first description a decade ago,” says Chowdhary.
Both C. auris and SARS-CoV-2 are found on hospital surfaces including on bedrails, beds, air conditioner ducts, windows and floors, says Chowdhary. “So, COVID-19 critical care, involving the use of ventilators and catheters makes patients potentially susceptible to C. auris infection.”
COVID-19 patients often share co-morbidities, such as diabetes and chronic kidney disease, with those infected by C. auris. Treatments may also be similar and involve systemic steroids and broad-spectrum antibiotics, apart from ventilation and intubation, according to the study in the Journal of Global Antimicrobial Resistance.
As with SARS-CoV-2, medical researchers have been trying to determine the natural origins of C. auris but with little success so far. Experts suspect that it emerged from the wild possibly as a result of climate change. The present study notes that a hypothesis published July 2019 in mBio suggests that C. auris might be native to wetlands and that its emergence as a human pathogen may be linked to the effects of global warming effects on wetlands.
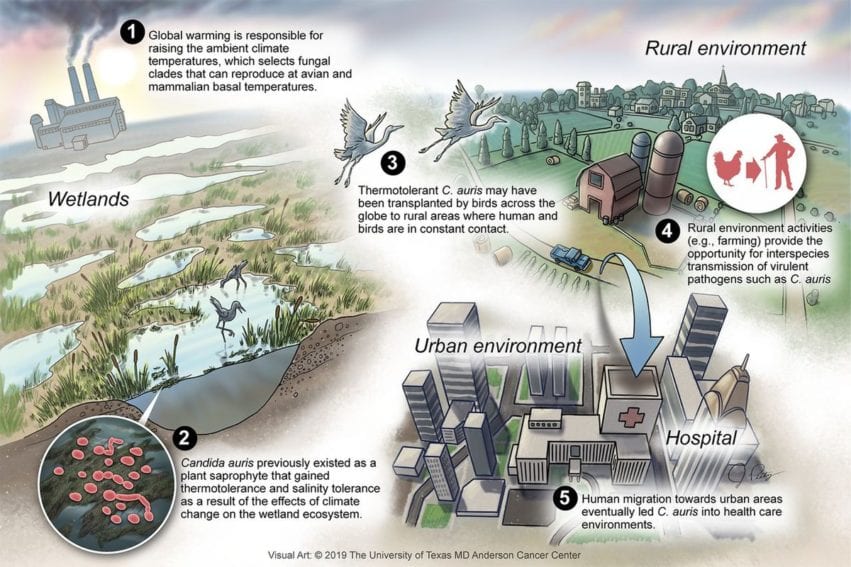


Proposed scheme for the emergence of Candida auris. Image credit: Arturo Casadevall, Dimitrios P. Kontoyiannis, Vincent Robert/mBio (CC BY 4.0).
“It is to understand the mystery of environmental niches of C. auris that we explored the coastal wetland habitat around the very isolated Andaman Islands,” Chowdhary and her colleagues write in the new study. “The isolation of C. auris from uninhabited marine wetlands suggests that prior to its recognition as a human pathogen, it existed as an environmental fungus.”
Chowdhary says that despite the findings of the study the link to human infections remains to be investigated. “So far, no implications can be derived as to how it is transmitted to humans.”
This piece was produced by SciDev.Net’s Asia & Pacific desk.