31/01/20
Study turns HIV transmission assumption on its head
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
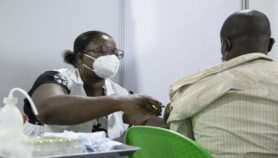
[NAIROBI] A study debunks the prevailing assumption that HIV spreads from hotspots to areas with low prevalence, and suggests that interventions in such hotspots are unlikely to help control transmission in low-risk areas.
Researchers say that understanding HIV transmission dynamics is essential for effective deployment of HIV prevention tools, particularly in resource-limited settings such as Sub-Sharan Africa, which in 2017 had 1.2 million new HIV cases or 60 per cent of all new cases worldwide.
The study published in The Lancet HIV this month (14 January) focused on fishing communities on the shores of Lake Victoria in Uganda as hotspots and their surrounding low-risk areas.
Findings show that cross-community HIV transmissions between hotspots and surrounding inland populations were infrequent, with the virus more commonly flowing into rather than out of hotspots when they occur.
“Our study findings caution against equating and stigmatising HIV hotspots as populations that drive disease spread.”
Kate Grabowski, Johns Hopkins Bloomberg School of Public Health
“These data provide new insights into the factors that give rise to the spatial distribution of HIV within Africa, which can be used to more effectively deploy interventions for maximal population benefit,” says Kate Grabowski, a co-author of the study and an assistant professor at the US-based Johns Hopkins Bloomberg School of Public Health.
“Our study findings caution against equating and stigmatising HIV hotspots as populations that drive disease spread.”
According to the study, interventions directed to only the hotspots only will not control the epidemic in inland populations.
Grabowski explains that the lower prevalence areas, which have substantially more numbers of HIV cases because of their larger population size, seed more infections to the high prevalence fishing communities.
Researchers assessed HIV genes and their functions — an approach called viral genomics — from 2,439 people in hotspots around Lake Victoria and 2,703 people in surrounding inland communities.
The HIV-positive individuals were identified through population-based surveys conducted among more than 25,000 individuals between 2010 and 2015. Information from the genetic analysis was used to track disease spread in a highly mobile population.
“An estimated 80 per cent of transmissions were within inland communities or within fishing communities, 7.8 per cent were from inland to fishing communities, [and] 3.5 per cent were from fishing to inland communities, ” the study says.
The study, according to Grabowski, can help policymakers develop strategies for reducing transmission while scientists can benefit from its innovative methodologies, including viral genomics, to study the flow of infection across communities and to study other infectious diseases.
The general public can learn that neighbouring areas with high HIV prevalence do not necessarily fuel transmission in their communities and that people in high prevalence communities should not be blamed or stigmatised for the HIV epidemic.
Halima Dawood, an honorary senior scientist at the Centre for the AIDS Programme of Research in South Africa, says that HIV transmission dynamics is more complex.
“I think this is a single study and as such may just be a signal to suggest different factors at play,” Dawood adds. “Targeting hotspots will have the added indirect benefit of reducing new HIV infections in the wider population.”
Francois Venter, deputy executive director of the Wits Reproductive Health and HIV Institute at the University of the Witwatersrand, South Africa, tells SciDev.Net that the study provokes a need to re-visit who to focus on in terms of prevention programmes.
“This new data may not hold for other areas but we need to check,” he says. “I think it is a provocative study — so much we know about HIV has been turned on its head by good studies — and this is a good study.”
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.
References
Kate Grabowski and others Quantifying HIV transmission flow between high-prevalence hotspots and surrounding communities: a population-based study in Rakai, Uganda (The Lancet HIV, 14 January, 2020)