31/12/21
New link between sickle cell and severe malaria found

By: Ijeoma Ukazu
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
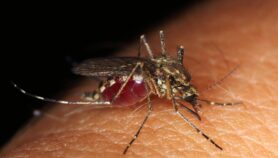
[LAGOS] Malaria parasites may have adapted so that they can cause severe malaria in people with sickle cell disease, a study suggests.
Sickle cell, a group of conditions which can cause red blood cells to become sickle shaped, is become common in Africa because the genes responsible for the disease can help prevent malaria during early childhood, according to the World Health Organization (WHO).
However, a study published in the December edition of Nature, found that specific changes in three regions of the malaria parasites’ genome could be responsible for malaria infections in people with sickle cell disease.
“Now basically we want to flag this up that sickle cell disease patients could still have malaria.”
Wellington Oyibo, University of Lagos
“The [malaria] parasites that cause disease in people who carry sickle haemoglobin are almost always the specific types of parasites,” explains Gavin Band, lead author of the study and statistician at the Wellcome Center for Human Genetics, University of Oxford.
“They have these specific alleles [two or more forms of genes] in these three regions of the parasite genome. That is an exciting finding not known before.”
The researchers looked for genetic variants in over 3,000 children from Gambia and Kenya children who had developed severe malaria.
Their findings suggest that the deadly malaria parasites seem to have evolved to be able to attack people with normal haemoglobin and sickle haemoglobin, with the potential of causing severe disease in those normally thought of as unlikely to bear the brunt of malaria in Sub-Saharan Africa.
“Parasites have big genomes,” says Band. “They evolve on much quicker timescales than humans and we know actually that they can evolve very quickly in response to selection pressures we have seen with response to antimalarials in the past.”
The findings are a step towards developing treatments for the problem, but there is still a lot of work to do.
“It would be great if, in future, this might lead to something for people with sickle cell, but that is not where we are now,” Band tells SciDev.Net. “The next step would be that we need functional studies to find out what these variants do.”
Wellington Oyibo, a professor of medical parasitology at the University of Lagos in Nigeria, commends the researchers for identifying an association between severe malaria in people with sickle cell disease and different regions of malaria parasites’ genome.
“The belief that patients with sickle cell disease … are protected from malaria is not completely true,” he says.
“We have vulnerable groups described as children under five, pregnant women and children. Now basically we want to flag this up that sickle cell disease patients could still have malaria and require special care and special protection including early diagnosis and household prevention,” Oyibo adds.This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.