04/12/19
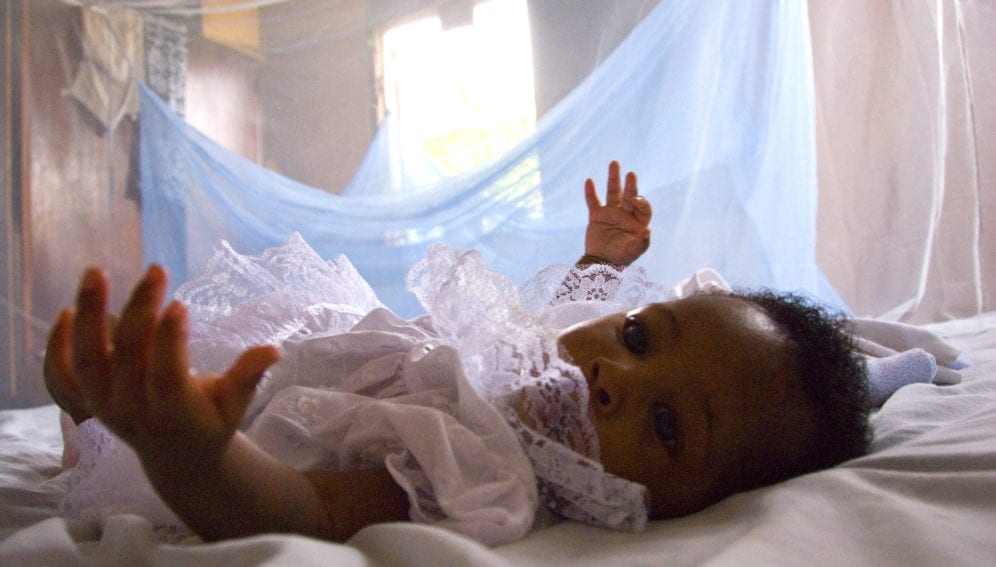
Augmented bed nets cut malaria cases by 25 per cent
By: Esther Nakkazi
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
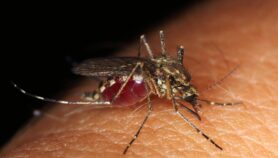
[KAMPALA] Insecticide-treated bed nets combined with a new chemical could cut malaria cases by about 25 per cent, a study in Uganda shows.
Researchers say that despite widespread use of long-lasting insecticidal nets in Sub-Saharan Africa, their impact on malaria control is lower than expected because mosquitoes are increasingly becoming resistant to insecticides called pyrethroids used to treat the bed nets.
The WHO has endorsed the new chemical called piperonyl butoxide (PBO) in the interim to augment existing treated bed nets in areas where resistance is common, the researchers add.
“PBO long-lasting insecticidal nets were more effective than conventional nets in Uganda, where resistance to pyrethroid insecticides is high.”
Martin Donnelly, Liverpool School of Tropical Medicine
In a large-scale trial in Uganda that was launched in February 2017 and is expected to end in April 2020, the researchers are comparing the effectiveness of bed nets with the standard chemical and those with the new chemical in reducing malaria cases.
“PBO long-lasting insecticidal nets were more effective than conventional nets in Uganda, where resistance to pyrethroid insecticides is high,” says Martin Donnelly an expert in the genetics of insecticide resistance at the UK-based Liverpool School of Tropical Medicine and a co-leader of the trial in Uganda.
Researchers presented the preliminary findings of the study last month (21 November) at the 68th annual meeting of the American Society of Tropical Medicine and Hygiene in the United States.
Researchers say that the new chemical blocks the resistance of mosquitoes to the insecticide in the bed net.
According to the researchers, households supplied with the PBO-treated bed nets had 80 per cent fewer malaria-carrying female mosquitoes compared to households using conventional nets.
“Less female Anopheles mosquitoes mean less infective bites to community members, which in turn leads to reduced transmission of malaria infection,” Donnelly explains.
According to Donnelly, the number of children testing positive for malaria parasites in a 12-month period after the nets were distributed was 25 per cent lower than for those under nets treated with PBO.
Researchers randomly selected about 23,000 children between two and ten years old in 5,200 households in Uganda, and divided them into two groups, with one group sleeping under bed nets augmented with the new chemical while the other group are sleeping under nets treated solely with pyrethroid insecticides.
The findings after 12 months show that malaria parasite resistance was 10.7 per cent in the PBO arm compared to 14.5 per cent in the group not having the new chemical.
Medard Rukaari, the officer in charge of universal bed net distribution at the Uganda National Malaria Control Programme, tells SciDev.Net that when “PBO-impregnated nets were distributed massively in February 2017, a drastic malaria reduction was achieved within six months of its distribution”.
Rukaari adds that the government is already distributing PBO-impregnated bed nets as part of the Uganda’s malaria control strategy.Donelly says that the contribution of conventional bed nets to malaria control should not be ignored.
“The results highlight that conventional [bed nets] provide protection and may still have a role in vector control programmes in settings where insecticide resistance and malaria transmission are low,” Donnelly explains.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.