Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
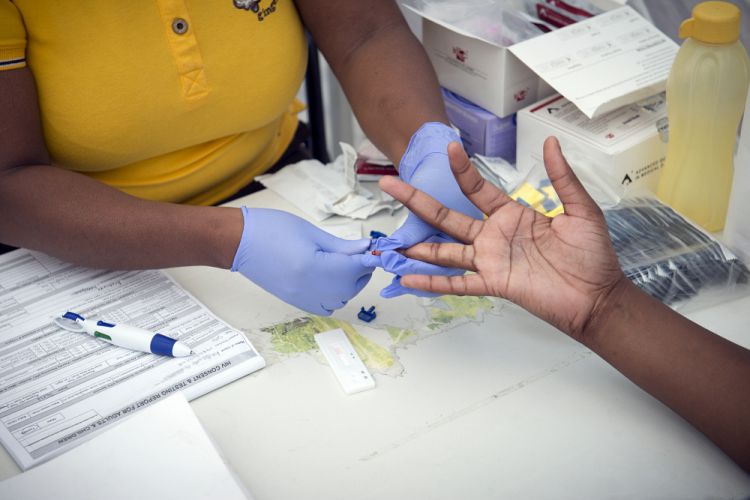
[DURBAN] Several studies show that people at high risk of HIV infection who take anti-retroviral (ARV) medicines regularly — an approach called pre-exposure prophylaxis (PrEP) — could reduce the risk of getting infected.
The studies were presented at the 21st International AIDS Conference in South Africa last month (18-22 July).
The ASPIRE trial, being undertaken by the Microbicide Trials Network, is testing the efficacy and safety of delivering a monthly vaginal ring having dapivirine, an ARV, in 2,600 young HIV-negative women from Malawi, South Africa, Uganda and Zimbabwe.
“More than half of the women in the communities the trials took place will likely be infected within ten10 years without PrEP.”
Zeda Rosenberg, International Partnership for Microbicides
Earlier this year, results showed the monthly ring reduced the risk of infection by 25 per cent. After further analyses, that figure has now risen to over 50 per cent.
Jared Baeten, a professor of global health at the US-based University of Washington in Seattle, and ASPIRE chair, says the ring could offer significant protection.
“It’s reduced the risk by half in women over 21…There’s also a correlation between protection and dosage. The higher the dosage and use, the higher the protection.” Baeten explains.
Results from the Partners Demonstration Project, which integrated PrEP and anti-retroviral treatment in 1013 Kenyan and Ugandan high-risk, heterosexual couples, with one partner having HIV and the other being negative, found that HIV transmission could be almost entirely eliminated.
Baeten reported that only five new HIV infections had been observed.
Plus Pills, a PrEP study involving oral use of Truvada, a combination drug with the ARVs tenofovir and emtricitabine, among South African adolescents at high risk of HIV, found no new HIV case, said Katherine Gill, a medical officer at the South Africa-based Desmond Tutu HIV Centre.
According to Gill, PrEP could be a viable alternative to condoms.
Zeda Rosenberg, CEO of the International Partnership for Microbicides, says they intend to submit the vaginal ring for regulatory approval in the United States by 2017, and that the product could be available for public use by 2018.
Rosenberg calls for an urgent need to expand PrEP for women: “More than half of the women in the communities the trials took place will likely be infected within ten years without PrEP.”
Linda-Gail Bekker, president-elect of the International AIDS Society and deputy director at the Desmond Tutu HIV Centre, says that PrEP could change the tide of HIV.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.