By: Anatoli Kamali
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
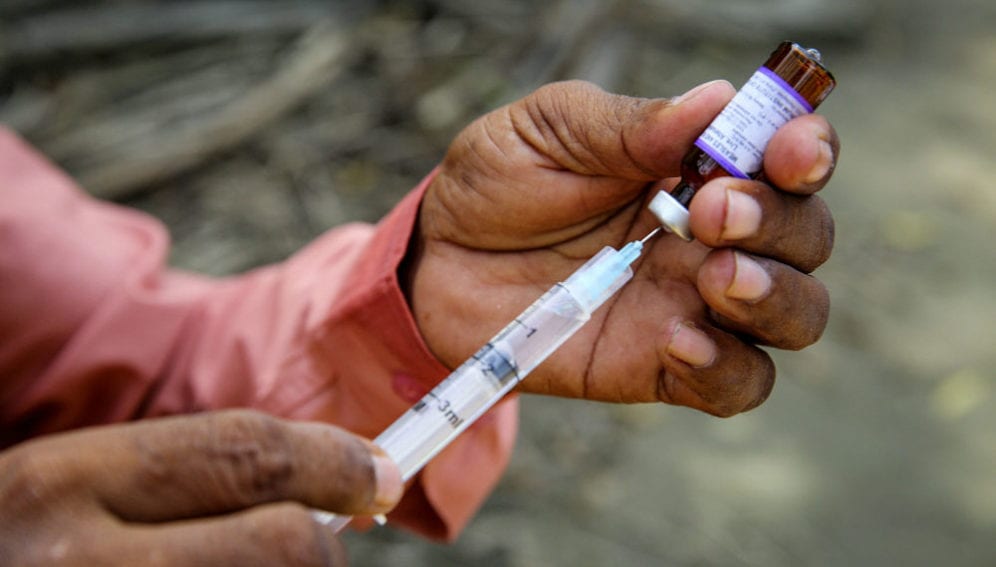
As the world commemorates the 21st anniversary of the World HIV Vaccine Awareness Day (HVAD) today (18 May), I want to turn the spotlight on the growing role of African scientists in the race towards HIV prevention research and ending AIDS epidemic.
Over the past 25 years, I have been privileged to contribute to, and be a part of a growing critical mass of African researchers providing leadership in HIV/AIDS prevention research globally.
Earlier HIV prevention efforts
My own journey began in 1986 as a graduate of medicine and surgery at the Makerere University Medical School in Kampala, Uganda. The end of my undergraduate training had coincided with the appearance of the first patients of “Slim” disease – the beginning of AIDS epidemic in Uganda. As a young medical officer, I found myself at the centre of an epidemic that was ravaging the country with one in every ten people infected with HIV in the rural areas and up to five times more along the Trans African highway within Uganda.
“I find it most encouraging that research led by African scientists has contributed to the global evidence informing policies for HIV prevention today.”
Anatoli Kamali, International Aids Vaccine Initiative
Caring for terminally sick patients with limited impact – a scenario that was playing out in many Sub-Saharan African countries – was very challenging. I soon faced the reality that without a preventative HIV vaccine, medical care and public health approaches alone would not end the epidemic.
My postgraduate training at the UK’s London School of Hygiene and Tropical Medicine in the late 80s provided me with a great opportunity to focus on HIV/AIDS epidemic as a public health threat. I was aware of the urgent need for research that would give a clearer understanding of the epidemic and inform policies to guide prevention and treatment interventions.
Upon returning to Uganda, I joined a team composed largely of expatriates to start one of the first major rural population-based epidemiological and clinical research at the Uganda’s Medical Research Council/Uganda Virus Research Institute. This research provided an initial understanding of HIV transmission dynamics and offered opportunities for testing and counselling in rural Africa as a first HIV prevention pillar.
Towards ending HIV/AIDS threat
A quarter of a century later, the AIDS epidemic is still a huge public health threat in many Sub-Saharan African countries, despite major achievements from HIV prevention and treatment research. With high mortality rates and close to 1.1 million new infections in 2016 in Sub-Saharan Africa, it is as clear to me now as it was when I was a young medical officer that we need to accelerate the search for an HIV vaccine if we are to end AIDS epidemic for good.
Recent modelling analyses project that even with stepped-up efforts to implement current treatment and prevention programs, hundreds of thousands of new HIV infections would still occur annually in the Sub-Saharan Africa region.
In the face of this continuing challenge, I find it most encouraging that research led by African scientists has contributed to the global evidence informing policies for HIV prevention today. Over the years I have had the opportunity to lead several studies in HIV epidemiology and studies which engage populations at higher risk of HIV/AIDS including young women and adolescent girls and fishing communities.
I have also led trials to evaluate the impact of behavioural change interventions alone or in combination with improved management of sexually transmitted infections on HIV transmission. I have also been leading early and late phase trials of vaginal microbicides, and preparations for HIV vaccine research and early HIV vaccine trials.
Value of research partnerships
Research partnerships have provided opportunities to build African capacity in HIV research. For example, high-level laboratory and clinical facilities are now in place to support the conduct of current and future trials that would have only been done in developed countries, and there is a growing number of highly trained African scientists in different areas of research for HIV prevention including vaccine development.
“With continued commitment from governments, international agencies, researchers and many other partners, we will find an HIV vaccine and end the HIV/AIDS pandemic.”
Anatoli Kamali, International Aids Vaccine Initiative
One outstanding example of the developing continuum of African research capacity in the HIV/AIDS research is Accelerating the Development of Vaccines and New Technologies to Combat the AIDS Epidemic (ADVANCE), a partnership between International Aids Vaccine Initiative and research partners in clinical research centres in five African countries in Southern and Eastern Africa: Kenya, Rwanda, South Africa, Uganda and Zambia . Through this USAID-supported partnership, nearly 50 staff from clinical research centres have been awarded master’s, doctorates or postdoctoral fellowships, with 20 junior staff advancing to the position of principal investigator or trial director.
Supporting women scientists
More importantly, the focus on supporting women scientists has resulted in 50 per cent of these awardees being female researchers. Beyond the fellowships, the ADVANCE partnership is building on, and linking African scientists’ competencies in HIV vaccine research and development to Indian, UK and US researchers and institutions through the Vaccine Immunology Science and Technology for Africa programme. These opportunities are attracting Western-trained African scientists back to Africa to pursue cutting-edge HIV vaccine research.
Such developments truly motivate me and give me the confidence that with continued commitment from governments, international agencies, researchers and many other partners, we will find an HIV vaccine and end the HIV/AIDS pandemic.
As HVAD comes of age, we must not lose the momentum gained through African-driven research.New investments towards controlling the epidemic should aim at sustaining the gains made in HIV vaccine research and development, and focus on equipping and resourcing African scientists and research institutions to take the lead in the design and assessment of the next generation of HIV vaccine candidates for Africa.
Anatoli Kamali is the Africa regional director for the International Aids Vaccine Initiative (IAVI), and lead for the Accelerating the Development of Vaccines and New Technologies to Combat the AIDS Epidemic (ADVANCE) partnership, and an Honorary Professor at the London School of Hygiene and Tropical Medicine’s Department of Infectious Disease Epidemiology. He can be reached at [email protected]
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.
References
[1] Global HIV statistics (UNAIDS, 2017)
[2] Thomas M. Harmon and others Exploring the potential health impact and cost-effectiveness of AIDS vaccine within a comprehensive HIV/AIDS response in low- and middle-income countries (PLoS ONE, 5 January 2016)