By: Gilbert Nakweya
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[NAIROBI] Addressing data gaps and strengthening of health systems could help Sub-Saharan Africa reduce the rapidly rising burden of non-communicable diseases (NCDs), experts say.
This was said during the third anniversary of Healthy Heart Africa (HHA), an initiative that aims to tackle hypertension and cardiovascular disease in Sub-Saharan Africa.
The experts comprising research scientists, health professionals and policymakers from the health sector say that NCDs such as mental illness, hypertension, cancer, diabetes and chronic respiratory diseases are on the rise globally but are not accorded the necessary attention to control them, especially in Africa.
“We need data to attract the necessary funds needed to eradicate NCDs.”
Ephraim Maree, Ministry of Health, Kenya
According to the WHO, NCDs contributed to 38 million (68 per cent) of the 56 million deaths globally in 2012, with almost 28 million deaths from NCDs occurring in low- and middle-income countries, including those in Africa. By 2020, the increase in deaths from NCDs is expected to be 17 per cent globally whereas in Africa it is projected to be 27 per cent.
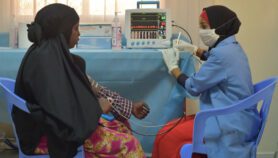
During the event held in Kenya this month (19 January), the experts called for supporting local health systems through increasing awareness of the symptoms and risks of NCDs and offering education, screening, reduced-cost treatment and control in Africa.
The initiative of the US-headquartered pharmaceutical company AstraZeneca also aims to train healthcare providers to implement community-based interventions and to help people get access to affordable medicines.
“We launched this initiative in Kenya and Ethiopia to help reduce the rising burden of NCDs in Africa,” said Ashling Mulvaney, senior director of HHA.
Mulvaney said that the initiative will be expanded to five countries this year to help reach their target of screening ten million people by 2025.
“But we want to go beyond screening and link the patients’ treatment after diagnosis,” Mulvaney told SciDev.Net, adding that HHA had screened almost three million people in Ethiopia and Kenya since its launch in 2014.
Jim Massey, vice-president for sustainability at AstraZeneca, said that public-private partnerships are key to controlling NCDs, the leading cause of death globally.
Partnerships with ministries of health, policymakers, scientists, and research organisations, he said, could help address the challenge holistically and foster sustainability. He added that disease awareness is important for prevention, noting that in Kenya, one in every four people may be hypertensive but they do not know.
Ephraim Maree, a research fellow from the NCDs division of Kenya’s Ministry of Health, explain that NCDs are generally neglected because of data gaps. “We need data to attract the necessary funds needed to eradicate NCDs,” Maree said.
Maree added that Kenya has inadequate baseline data on NCDs, thus making it difficult to persuade the government to allocated money needed to combat the burden of NCDs.
Grace Mugambi, a community health worker from Kikuyu Health Centre in Kiambu county, Kenya, tells SciDev.Net that increased training of local health workers, who interact with patients daily, is important in fighting against NCDs.“Community health workers could help persuade more people to get screened and save lives,” Mugambi adds.
This piece was produced by SciDev.Net’s Sub-Saharan Africa English desk.