By: Priya Shetty
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Priya Shetty looks at the prevalence and distribution of tuberculosis in the developing world, outlining the truths — and myths — about this disease.
The facts show undeniably that tuberculosis (TB) is a major problem for the world's poor. Over two billion people worldwide carry the bacterium that causes TB, with approximately 15 million people suffering from an active infection at any one time.
The disease burden is highest in developing countries where people are especially vulnerable to TB because of poor underlying health, adverse living conditions and limited access to treatment.
Although the disease is often treatable, for many people in these nations it is fatal. TB kills 1.6 million people every year; 4,400 people every day; one person every 20 seconds. 98 per cent of all TB deaths occur in developing countries [1].
The economic implications of this devastation are huge: fighting the disease drains US$12 billion from the annual incomes of the world's poorest communities. The loss of productivity attributable to TB is estimated to be 4–7 per cent of gross domestic product. [1]
Figure 1 shows the ten countries with the highest numbers of TB victims — all are in the developing world.

Figure 1: Countries with highest numbers of people living with TB (2005). [2]
But it is important to put overall numbers into context, relative to a country's population size. Figure 2 shows the countries that have the highest prevalence of TB sufferers per 100,000 of the population — a different picture from Figure 1. Almost all of these countries are in Africa, where resources for TB treatment and control are limited.



Figure 2: Countries with the highest numbers of people living with TB per 100,000 of the population (2005). [2]
About the disease
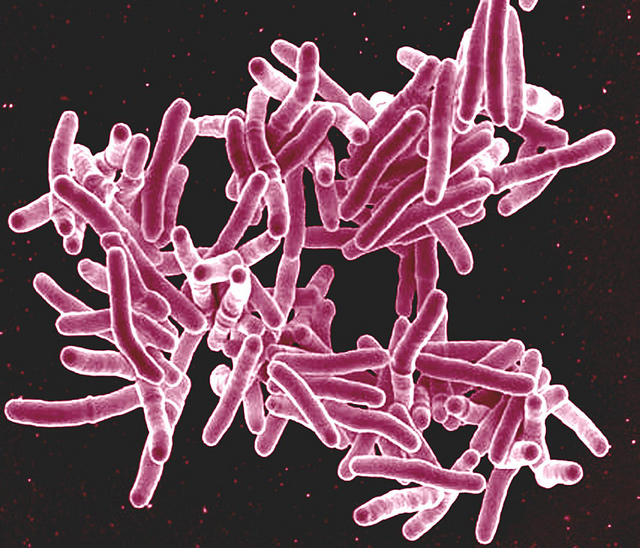
TB is an infectious disease caused by the Mycobacterium tuberculosis bacterium, which most commonly affects the lungs. There are two forms of TB: active, where a patient has symptoms and an abnormal chest X-ray; and latent, where a person has no symptoms and their chest X-ray is normal, but a skin test gives a positive result for TB.
The symptoms of active TB of the lungs include coughing — sometimes with sputum or blood — chest pains, weakness, weight loss, fever and night sweats. It is spread through the air when infected people cough, sneeze or speak.
Despite its prevalence, many people are unaware of the complexities of TB — for example, that it can lie dormant in seemingly healthy people. Accurate information is key to tackling any major disease epidemic and unless people know what the symptoms of TB are, they are unlikely to get treatment before reaching the infectious stage of active disease.
Strategies for controlling TB increasingly include education aimed at informing people of the key symptoms of TB and dispelling the common myths that surround this disease (see Box 1).
|
Box 1: TB myths In many developing countries, people with TB suffer from discrimination and stigma, which can affect the uptake of screening or treatment. Often this comes from a lack of understanding about the disease and its treatment. For example, many people in the developing world believe that they will die if they go on TB treatment and so are unwilling to begin medication. Such views are fuelled by the high death rates among patients who only start treatment when they are in advanced stages of the disease and there is little chance of saving them. A study undertaken by healthcare workers in Zambia in 2005 found there are a range of misconceptions about TB. [3]. These include the common beliefs that:
The study also found that people often identified factors that can exacerbate TB — such as smoking or cold weather — as being the actual causes of the disease. But at the same time, a large number of people do not recognise the extent to which overcrowding and poor ventilation help spread TB. |
TB and HIV/AIDS
TB is the leading infectious killer of people with HIV/AIDS, and a particular problem in sub-Saharan Africa, where a third of people with HIV are also infected with TB. In most of these countries, over half of patients presenting with TB are co-infected with HIV (see Table 1).
| Country | Per cent adult TB patients co-infected with HIV |
|
|
|
|
Swaziland |
75% |
|
Botswana |
70% |
|
Lesotho |
64% |
|
Zimbabwe |
60% |
|
South Africa |
58% |
|
Namibia |
56% |
|
Zambia |
55% |
|
Malawi |
50% |
|
Mozambique |
50% |
|
Central African Republic |
42% |
|
Gabon |
34% |
|
Uganda |
30% |
|
Tanzania |
29% |
|
Kenya |
28% |
|
Cameroon |
26% |
|
Congo |
25% |
|
|
|
Table 1: Top 15 countries with highest HIV/AIDS prevalence in adults with TB (2005) [2]
Because of their weakened immune systems, HIV/AIDS patients are up to 20 times more likely to develop TB than people without HIV. [4] TB is also more fatal in HIV/AIDS patients, with up to half of all deaths of HIV/AIDS patients due to TB. A person with both diseases can be four times more likely to die during TB treatment than someone with TB alone.
Yet effective treatment of HIV/AIDS patients infected with TB is still possible, principally through the addition of an antibiotic, cotrimoxazole, which can reduce the death rate during TB treatment by 40 per cent [4].
Still, stigma related to both diseases can mean that patients infected with one disease are reluctant to voluntarily be tested for the other. The lack of integration across national HIV/AIDS and TB control programmes also means that routine screening of TB patients for HIV, and vice versa, is not in place for many developing countries (see Collaboration to kill: HIV/AIDS and TB).
TB treatment
Current treatment consists of 6–9 month courses using a combination of two or more of the four first-line drugs: isoniazid, ethambutol, pyrazinamide and rifampin. These regimens work for active, drug-susceptible TB — as long as the course is completed.
Not completing the course can lead to relapse, continued transmission and the development of drug resistance — a growing concern in the fight against TB.
One strategy that has been adopted by the World Health Organization (WHO) to help ensure that patients complete TB treatment is directly observed therapy (DOT), where a health worker watches the patient swallow each dose of TB medication (see Figure 3).



Figure 3: Percentage of population nominally serviced by health facilities implementing DOTS. [2]
One of the Millennium Development Goals set for 2015 is to reduce the prevalence of and deaths due to TB by 50 per cent of 1990 figures. DOT can lead to more successful treatments of infectious TB, which can in turn help prevent the spread of the disease (see Figure 4).



Figure 4: Percentage of DOT treatment success, indicating the percentage of new smear-positive patients are cured, plus the percentage that complete a course of treatment.
Drug resistance
About 450,000 new cases of multidrug-resistant TB (MDR-TB) occur every year, with the highest prevalence in China, India and the countries of the former Soviet Union.
These patients cannot be treated with first-line drugs and often require extensive chemotherapy for up to two years. In 1999, the WHO launched the DOTS-Plus programme to manage MDR-TB with second-line drugs in resource-limited settings. This includes integrating drug resistance surveillance into TB control strategies and scaling up MDR-TB treatment.
The major barrier to treatment of MDR-TB in developing countries is the high cost of second-line drugs, which are between 300 and 3000 times more expensive than first-line drugs. Other barriers include the limited number of laboratories equipped for drug susceptibility testing and the fear of developing extensively drug-resistant TB (XDR-TB) — where the disease is resistant to second-line drugs as well as first-line ones.
Cases have been confirmed in KwaZulu-Natal, South Africa — where 52 of 53 patients diagnosed with XDR-TB died within 25 days of sputum collection — and worldwide.
The resistance to second-line drugs makes XDR-TB extremely difficult to treat. But new drugs are in the pipeline (see Table 2) [5].
| Drug |
Development stage |
Coordinator/funder |
|
TMC 207 (previously R207910) |
Early bactericidal activity |
Johnson and Johnson (Tibotec) |
|
OPC-67683 |
Early bactericidal activity |
Otsuka Pharmaceutical |
|
PA-824 |
Phase I |
TB Alliance |
|
LL-3358 |
Phase I |
Lupin |
|
Moxifloxacin |
Phase II/III |
Bayer, TB Alliance, Centers for Disease Control and Prevention, University College London, Johns Hopkins University |
|
Gatifloxacin |
Phase III |
European Commission/OFLOTUB consortium, Institut de Recherche pour le Développement, WHO TDR, Lupin |
Table 2: Tuberculosis drug clinical development pipeline (2006)
Further information
Further information on the epidemiology of TB and statistics on the disease in countries worldwide can be found at the following websites:
WHO TB data and country profiles
The WHO links to detailed country profiles and estimates of TB burden, as well as interactive maps and data annexes of major relevant WHO reports.
TB Alliance
The Global Alliance for TB Drug Development is a non-profit organisation working with public and private laboratories to develop new, effective and affordable TB drugs. It publishes information on its current portfolio of TB drug candidates and links to policy documents and resources.
TB Alert: frequently asked questions
TB Alert has gathered together some commonly asked questions about TB to provide basic facts and figures about the disease. Questions include 'what is TB?', 'how is it spread?' and 'can it be prevented?' among others.
References
[1] TB Alliance. The threat of TB.
http://www.tballiance.org/why/tb-threat.php
[2] Globalhealthfacts.org
http://www.globalhealthfacts.org/bytopic.jsp?cat=2
[3] Alcorn, K. Stigma and myth still harming TB fight. AIDSMAP news, October 25 (2005)
http://www.aidsmap.com/en/news/F1064B98-5293-4636-85F0
-14D07AA15DD2.asp
[4] Médecins Sans Frontières. TB and HIV: the failure to act. March (2007) www.msf.org/source/annual/tbday/2007/tb-hiv-failure-to-act.pdf ![]()
![]()
![]()
[5] Spigelman, M. and Gillespie, S. Tuberculosis drug development pipeline: progress and hope. Lancet, 367, 945-947 (2006)