By: Claudia Caruana
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[NEW YORK] The first-ever UN high-level meeting on tuberculosis last week (26 September) placed its hopes in new technologies as it lent its weight to the SDG goal of eradicating TB by 2030.
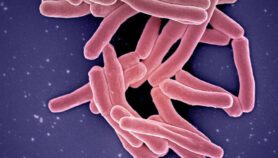
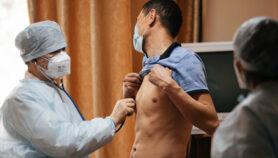
TB remains the world’s deadliest infectious disease, killing 1.6 million people in 2017, including 300,000 people with HIV. Last year, some 10 million people fell ill with TB with the largest number of new cases occurring in South-East Asia and Western Pacific. The five countries with most TB cases are from the Asia Pacific region namely, India, China, Indonesia, the Philippines and Pakistan.
The meeting, part of the UN General Assembly, was preceded by finger pointing by NGOs and other stakeholders about low interest on the part of some governments and lack of access to available drugs because of high costs that hamper efforts to tackle a disease responsible for two million deaths annually.
“It’s important that we take advantage of these tools to detect latent TB so we can prevent it from becoming a dangerous, contagious disease,”
Lee Reichman
Nonetheless, presentations by countries such as China and South Africa described committed strategies to end TB. The Indian government, for example, described how it had tripled its budget to eradicate it.
Bill Gates, chair of the Bill and Melinda Gates Foundation, noted that although the percentage of TB patients “receiving quality care has tripled since 2000, saving 54 million lives, millions more were falling through the cracks”.
Heads of state and government attending the New York meeting agreed to mobilise US$13 billion a year by 2022 to implement TB prevention and care, and US$2 billion for research. They also committed to take firm action against drug-resistant forms of the disease, build accountability and to prioritise human rights issues such as the stigma that prevails around TB in many parts of the world.
Lee Reichman, professor of medicine and the founding executive director of Global Tuberculosis Institute at Rutgers, believed that “historically, there is a perception that people with TB are unimportant or powerless. As a result, TB has been tolerated and hasn’t been a focus of mainstream public health programmes”.
New technologies are the game changers in TB elimination, said Reichman, citing the example of Interferon Gamma Release Assay blood test, an immense improvement over the traditional 100-year-old skin test. “It’s important that we take advantage of these tools to detect latent TB so we can prevent it from becoming a dangerous, contagious disease.”
Multi-drug resistant TB (MDR TB), Reichman said, is in the news a lot because of its low 50 per cent cure rate. “But if TB is detected and treated while in its latent form, we don’t have to worry about people getting TB, let alone people getting a life-threatening form.”
Els Torreele, executive director of Médecins Sans Frontières’s Access Campaign, said that diagnosis, treatment, and prevention of TB are difficult using today’s options, and new, better medical tools are urgently needed.
“We need short-course oral drug regimens with high cure rates and that are well tolerated; point-of-care, rapid, accurate, child-friendly diagnostic tests, and drug susceptibility tests to know which drugs are effective in patients who may have resistant infections; and ideally an effective vaccine,” Torreele said.
Torreele believed that open, collaborative research instead of proprietary research, including joint development of combination regimens, would be the way forward, as also the sharing of promising therapeutic molecules and preclinical and clinical trial data and enforcing fair pricing and licensing policies.“Last year, BRICS (Brazil, Russia, India, China, and South Africa) announced the BRICS TB Research Network to prioritise and coordinate collaborative TB R&D,” said Torreele.
Adrian Thomas, vice-president, Global Public Health, Johnson & Johnson, said a new, special effort price is effective immediately in countries currently purchasing bedaquiline — and will go into effect March 2019 for countries currently accessing the medicine through the donation programme. Bedaquiline is approved in 56 countries, including the ones with the highest burden of MDR TB.
“Beyond where we have formal regulatory approval, bedaquiline is available in many more countries procuring via the Stop TB Partnership's global drug facility. To date, we have provided nearly 70,000 courses of treatment to patients in 107 countries,” Thomas said.
This piece was produced by SciDev.Net’s Asia & Pacific desk.
* This piece was amended on October 9th 2018 to correct the spelling of Dr Lee Reichman’s name throughout.