By: Yao-Hua Law
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
Chikungunya is often misdiagnosed as the better-known dengue fever, says a study, suggesting that the disease’s worldwide burden is underestimated.
Both diseases are transmitted by the same mosquitoes and trigger symptoms of fever, headache and rashes.
“There is a lot of misdiagnosis happening,” says coauthor Laith Yakob, an infectious disease ecologist at the London School of Hygiene & Tropical Medicine in the United Kingdom. This means patients might receive inappropriate treatment and epidemiologists might be using inaccurate data, the paper says.
“Because [both diseases] have similar symptoms, our study suggests that a lot of what is reported as dengue is chikungunya.”
Laith Yakob, London School of Hygiene & Tropical Medicine in the United Kingdom
Yakob tells SciDev.Net that doctors tend to rely on clinical symptoms alone for diagnosis instead of using more expensive, but definitive laboratory tests. “Because [both diseases] have similar symptoms, our study suggests that a lot of what is reported as dengue is chikungunya,” he says.
The study, published in BMC Infectious Diseases last week (3 March), drew on international public health databases to establish the distribution of chikungunya, dengue and their vector mosquitoes, Aedes aegypti and Ae. albopictus.
The distribution map shows that 154 countries have reported dengue and 99 have reported chikungunya. Almost all countries with chikungunya also reported dengue. In contrast, only two-thirds of countries with dengue also reported chikungunya.
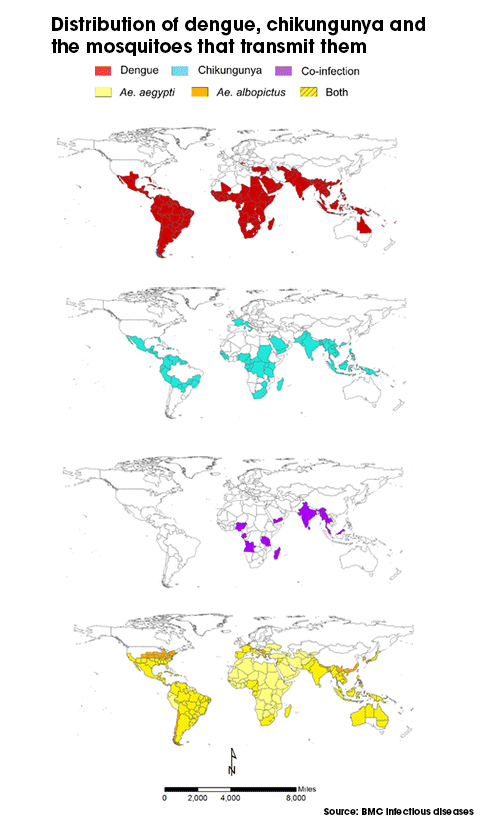
The authors also reviewed the scientific literature to estimate the extent of coinfection in patients. Out of 30 reviewed studies that documented such coinfection, only one started as a dengue examination. The rest were cases where the researchers first suspected chikungunya and checked for dengue later.
“Coinfections are typically identified only during a chikungunya outbreak,” says Yakob, but few reports of chikungunya were found during a dengue outbreak. “There is an intrinsic bias towards looking for dengue which is also going to skew the [reported] distribution of chikungunya.”
However, recent chikungunya outbreaks are raising awareness of the disease among the public and health workers, the paper says.
Sazaly bin Abu Bakar, a microbiologist at the University of Malaya in Malaysia, downplays the significance of misdiagnosis in his region. “Most countries in South-East Asia largely use laboratory tests and misdiagnosis is not a concern,” he tells SciDev.Net.Sazaly says dengue might be more widespread than chikungunya because people worldwide lack immunity against the various types of dengue virus. In contrast, a single exposure to chikungunya provides immunity, “hence re-exposure is not likely to spread the disease”, he says.
But Yakob says he hopes the study will encourage countries that report dengue but not chikungunya to increase their surveillance. “I am suggesting that chikungunya is not in just 99 countries, but it is much closer to the 154 countries that report dengue.”
References
Luis Furuya-Kanamori and others Co-distribution and co-infection of chikungunya and dengue viruses (BMC Infectious Diseases, 3 March 2016)