By: Imogen Mathers
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
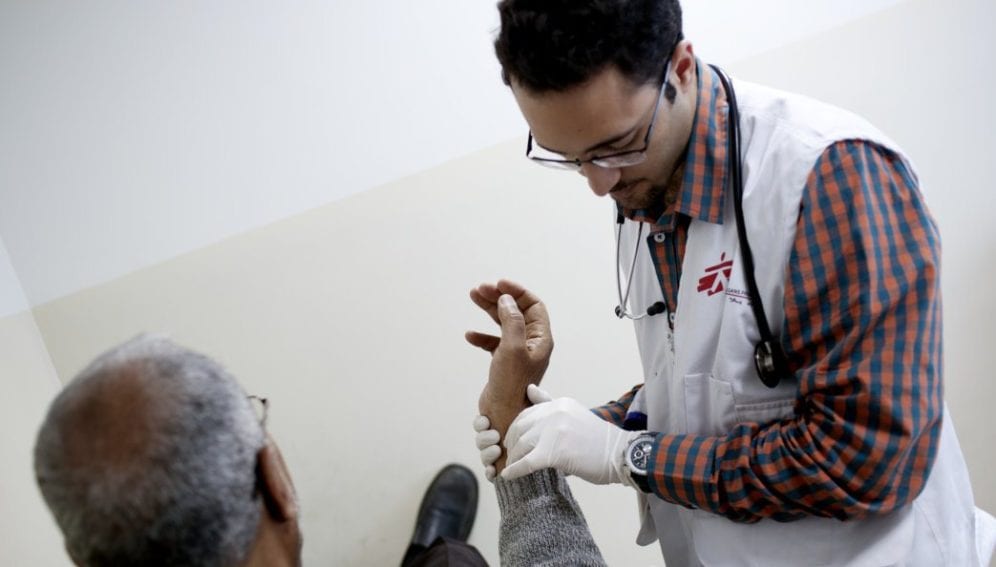
“Syrian refugees are not dying from pneumonia, they’re dying from diabetes and heart problems”, says Jon Gunnarsson of Médecins Sans Frontières. “Seventy-seven per cent of all mortality is due to non-communicable disease.”
Gunnarsson, who works with refugees in Jordan, says that non-communicable diseases (NCDs) represent one of the most urgent yet underfunded health crises facing Syrian refugees displaced by the country’s civil war.
There are 600,000 Syrian refugees registered in Jordan, 84 per cent of them living outside of refugee camps. Many are afflicted by NCDs such as hypertension, heart disease, asthma, smoking-related illnesses, and diabetes — indeed the Middle East and North Africa region has the highest prevalence of diabetes in the world, Gunnarsson says. These conditions are exacerbated by risk factors linked to the stress and trauma of displacement, as well as lack of access to treatment. For example, smoking and inactive lifestyles are widespread among those displaced, while high rates of depression can make treatment adherence more difficult for patients, he says.
So great is the problem, that MSF — an organisation that does not usually focus on NCDs — has been building NCD clinics and testing out new treatment programmes for refugees. Underpinning these is a ‘patient-centred model of care’, that includes health education, counselling, peer support sessions and motivational interviewing.
In this interview, Gunnarsson, who heads up an NCD nurse team in Irbid province in northern Jordan, explains why NCD care is so effective and vital for Syrian refuges, and outlines some of the results from their work in Jordan.