By: Maha Rafi Atal
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
India makes lifesaving medicine that Africa can afford — and US pressure mustn’t cripple that, says Maha Rafi Atal.
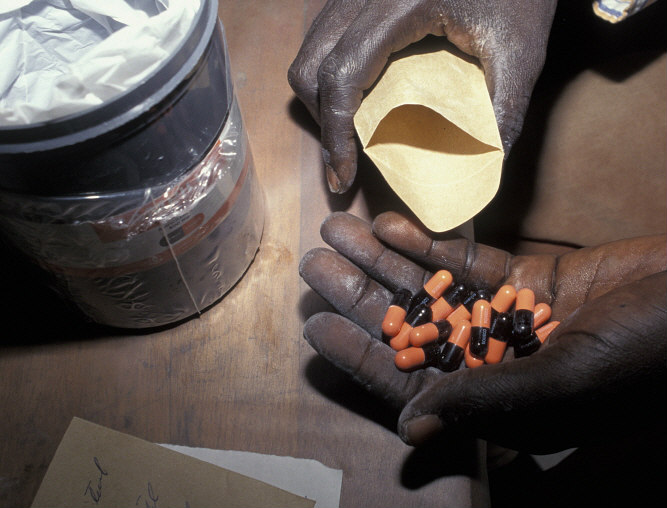
Aaron Motsoaledi, South Africa's health minister, recently fired up debates on global drug policy by warning that proposed changes to Indian patent law could spell death for Africans who depend on cheap, Indian-made drugs. “We regard India as the pharmacy of the developing world,” Motsoaledi said. “They were our heroes, and if they change their laws now, we will be in big trouble in Sub-Saharan Africa.”
Indian companies provide cheap generic drugs to countries across the world and account for 80 per cent of donor-funded HIV treatment — a set-up now threatened by US pressure. But Big Pharma should work with Indian companies and could even benefit by doing so.
India’s longstanding battle with Big Pharma over generic drugs dates from the 1970s, when it began only recognising patents for drug-making processes, rather than products. This allowed local companies to ‘reverse engineer’ expensive medications using different processes, and then offer drugs cheaply. In 2005, the country became party to the WTO TRIPS (Trade-Related Aspects of Intellectual Property Rights) agreement, which requires members to respect patent rights issued in other members’ markets. India negotiated the ‘compulsory licence’, allowing local companies to produce generic copies of foreign drugs for domestic use if there is a major public health need. These drugs can also be sold to foreign buyers.
Now India is under pressure from the United States to introduce ‘data exclusivity’, which grants IP protection to the data produced while developing a drug, as well as the drug itself. In practice, this would mean banning compulsory licensing, and might even restrict generic versions of off-patent drugs.
India’s prime minister Narendra Modi, eager to attract foreign investment, has indicated he is open to such reforms.
This is alarming for India and for countries and customers across Africa. In the 1990s, India’s Cipla Pharmaceuticals began offering HIV/AIDS anti-retrovirals in Africa at less than US$1 a day — far less than Pfizer’s US$33 a day. Now Médecins Sans Frontières estimates that nearly 80 per cent of anti-retrovirals in Africa come from India. And it’s not just HIV drugs: in 2011, India provided 17.7 per cent of all pharmaceutical imports to the continent.
“We regard India as the pharmacy of the developing world. They were our heroes, and if they change their laws now, we will be in big trouble in Sub-Saharan Africa.”
Aaron Motsoaledi, South Africa's health minister
Not only does this relationship deliver lifesaving treatments at prices African countries can afford, but Indian companies also tend to work closely with NGOs to deliver drugs, while Big Pharma usually relies on private buyers. In rural areas where health systems are weak, collaboration with local NGO personnel is crucial for delivering drugs to patients.
The benefits are economic too. The African market, expected to be worth US$30 billion by 2016, has helped the Indian drug industry grow into a business worth 128 crore Indian rupees (US$19.36 million) a year. So successful is India’s model that South Africa is considering remodelling intellectual property law along Indian lines, in the hope of stimulating its domestic manufacturing sector — a move also apparently threatened by US pharma lobbyists.
Meanwhile South African media reports the country is itself facing pressure to backtrack on proposed intellectual property reform geared towards widening drug access.
Beyond Africa, trade between developing countries also drives economic growth worldwide. South-South trade is worth about US$5 billion a year, while South-South aid and investment total US$19 billion. With new research demonstrating links between South-South cooperation and global growth, Western development agencies have begun to restructure their own programmes to facilitate trade between developing countries — by brokering partnerships and providing technical guidance, for example.It is crucial the Indian drug industry isn’t crippled by extreme patent reforms. The country should remind the US that, as India’s generics are largely sold in poor countries, the trade will hardly damage major US pharmaceutical firms in the core markets of North America, Europe and Japan. And there might actually be lucrative partnership opportunities within this generic drug trade, with Indian firms offering expertise about trading in Africa in exchange for Western research and development resources.