By: Mićo Tatalović
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
New TB vaccines are facing a major funding shortfall, says Mićo Tatalović, and some countries seem resistant to accepting a future vaccine.
International tuberculosis (TB) experts are gathering today — World TB Day — in France to discuss advances in research into vaccines.
But the reason there is no effective vaccine to prevent the roughly ten million new cases and two million deaths from TB each year has little to do with the science. There are already 11 vaccines in clinical trials whose progress has slowed or stalled because the funding has dried up.
That is why the TuBerculosis Vaccine Initiative (TBVI), an independent organisation that promotes the development of TB vaccines, is launching a new funding model today.
Joris Vandeputte, senior vice-president of advocacy and resource mobilisation at TBVI, tells SciDev.Net that US$1.5 billion is urgently needed to translate basic research into market-ready vaccines over the next decade. A single TB vaccine can cost up to US$300 million to develop.
Funding gap
Basic research has been adequately funded, he says, resulting in around 40 candidate vaccines because of a huge research effort over the past decade. In addition to the 11 in the faltering trials, a further 30 are languishing in laboratories, some of them in developing countries, waiting to be tested.
But the "second chunk" of funding, needed to get the candidate vaccines through clinical trials, is missing — so vaccine development has effectively stopped, he says.
Under the new funding model, the European Union would provide loans to fill the gaps, possibly through the European Investment Bank. The loans would be administered by the TBVI and paid back once the vaccines start making money.
The model takes into account various logistical difficulties facing the researchers, such as the bottleneck caused by the lack of capacity in clinical trials, by calculating in the costs needed to tackle such issues.
"We will have to look to the east — China, India, Russia — to do more clinical trials," he says, in an attempt to overcome this bottleneck. But he maintains that once there is a new vaccine, it will attract a huge market.
Around 90 per cent of countries currently vaccinate their children against TB with the Bacillus Calmette-Guérin (BCG) vaccine, using 100 million doses each year. BCG protects children from severe forms of TB but does not protect adults from pulmonary TB — the most common and infectious form of the disease.
A more effective vaccine would save huge amounts on treatment, which costs European countries alone about US$3 billion a year.
Low take-up
But even if the money for trials becomes available and an effective vaccine emerges, further problems may await. Data to be published later this year in a special vaccines issue of the journal Tuberculosis show that some developing countries may be reluctant to accept new TB vaccines.
Several factors seem to determine whether countries are prepared to shoulder the costs of a new vaccine campaign, including whether the vaccine has been tested in their own country.
The study’s authors conducted 86 structured interviews with public health clinicians, politicians and senior civil servants from health and finance ministries in countries with the highest burden of the disease: Brazil, Cambodia, China, India, South Africa, Mozambique, Romania and Russia.
Lew Barker, senior medical advisor at the Aeras Global TB Vaccine Foundation in the United States, says their study sought to gauge the opinions of people in high-burden countries who are likely to be involved in making decisions about whether to adopt TB vaccines when they become available.

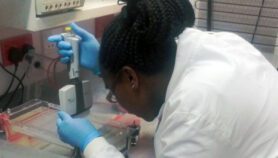
US$1.5 billion is needed to get the new TB vaccines on the market
WHO/TDR/Crump
"None of the respondents, when asked about the most important public health issues and needs of their country, spontaneously mentioned TB," Barker says. Instead, primary, rural and mother-and-child healthcare, as well as HIV/AIDS, were identified as the most pressing issues.
"However, when TB was mentioned [by the interviewer], they uniformly said this is a very serious problem and, by and large, they said it’s also a neglected problem that needs and deserves more attention then it gets," Barker adds.
Respondents in the survey welcomed the development of better TB vaccines, but around 20 per cent said it was unlikely that such vaccines would be taken up in their countries, and many more were undecided. In most of the vaccine roll-out scenarios presented, less than half said they were willing to commit to a new vaccine and provide funding. One of the main reasons was that they wanted to see strong efficacy data from clinical trials in their own country.
Political priorities
Vaccine deployment might take 20–30 years to reap healthcare benefits because 95 per cent of cases are latent and may take years to show up, and most vaccines only target people who have not been exposed to TB (around one third of the world’s population has been exposed), so there will be a long tail of cases before the hoped-for elimination of TB in 2050, Barker says. This explains why other issues such as HIV are given political priority.
Barker concludes that robust data showing efficacy of 90 per cent, rather than a more realistic 60 per cent, and from studies in the countries concerned, are likely to be needed for the introduction of new TB vaccines.
Opokua Ofori-Anyinam, senior clinical development manager at GSK Biologicals, a vaccine manufacturer, said researchers should engage with policymakers to make sure that, after spending millions of dollars on trials and testing vaccines in thousands of individuals, they end up with vaccines that policymakers will want to deploy.
"These are the things we have to think about ahead of time," Ofori-Anyinam tells SciDev.Net.
Vandeputte says the TB research community must engage with the media and policymakers to put TB onto national political agendas.
But he points out that Aeras’ market research, presented by Barker, found a mixed response and that the proportion of decision-makers who would go for a new vaccine is bigger than those who would not. Engagement and advocacy before a new vaccine reaches the market may also help convince the undecided.
Focus on the vaccine
Michel Greco, chair of the working group on new TB vaccines at the Stop TB Partnership, says: "I am not one of those people who think that as soon as we have a good TB vaccine it would be taken up. Countries are very wary of potential problems, so they go slowly."
But he adds that although studies are needed to address uptake issues and pave the way for the future deployment of TB vaccines, the priority should be on designing and testing vaccines rather than worrying about their subsequent uptake.
Helen McShane, a TB vaccine researcher at the University of Oxford, United Kingdom, whose vaccine MVA85A is currently in phase IIb clinical trials, told SciDev.Net: "The more effective a vaccine is, the more likely that it will be taken on. It will also depend on cost — I think if you have a very effective vaccine at affordable prices for the developing areas of the world then it will be taken on."
She adds: "There may be certain countries where you have to do some studies in that country to get some safety data but, although those are all important factors, I don’t see them as the biggest challenge — the biggest challenge is that we need to get a vaccine that works."