By: Imogen Mathers
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
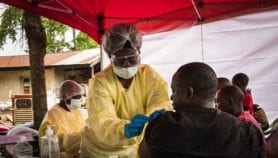
In the 18 months since Guinea confirmed its first case of Ebola, those involved in emergency response have faced tough questions. Accusations have been levelled at the WHO and others in the global health sector for their slow response, at national governments and their failing health systems, at journalists for scaremongering and distorting debates, and at donors for their tight purse strings.
Now the dust has hopefully settled, it is fascinating to hear which criticisms remain at the forefront of discussions. This week, at a pandemics conference at the Chatham House think-tank in London, United Kingdom, epidemiologists, aid workers, academics and policymakers agreed that communication failures still top the list.
Joanne Liu, director of health NGO Médecins Sans Frontières, spoke of communication problems at different stages of the epidemic — highlighting the “wrong messages” and clumsy approach to raising awareness of the disease among vulnerable local people. “I really don’t believe it was the right message to say: ‘There is a deadly disease, 50 per cent of people will die, we have no treatment, come and die alone in our Ebola centre’,” she said. “It doesn’t work for other diseases, and it doesn’t work for Ebola.”
Liu and others stressed the urgency of reviewing how health teams communicate with local people. As one speaker put it: “The monumental failure to coordinate with the people who matter most and to understand why communities were behaving as they were” carried a devastatingly high price.
Ways of improving how health teams draw on the knowledge and insights of traditional healers and social scientists — a frequent subject at Ebola-related events this year — also cropped up frequently.
The brutal cuts to the WHO outbreak budget and the disbanding of its communication and behavioural information group came in for some harsh criticism too.
Communication “across borders” — of nations and geopolitics, of scientific disciplines, of sectors — was another compelling subject. The event heard that Ebola was a “multidimensional crisis”, covering development as well as health, with roots in often disastrous development policies and IMF-driven public spending cuts. One solution offered to improve the world’s response to outbreaks was to create robust and flexible partnerships between sectors, organisations and governments, particularly in today’s cash-strapped climate.Time will tell whether these lessons reshape future crisis response. As one speaker said, perhaps one can only really talk about lessons learned when they’ve actually been applied.
This could start with conferences themselves. Throughout the debates, the lack of speakers from affected countries was ever more obvious. The panellists at Chatham House were predominantly European and North American, and unmediated local perspectives were almost entirely absent from the debate.
As Emmanuel d’Harcourt, senior health director at the International Rescue Committee, told me, one solution would be to hold more meetings in affected countries themselves. His organisation had a meeting to discuss Ebola response in Liberia, he said. “It was expensive [and] inconvenient, but it was crucial because [it] meant the majority of people in that room were Sierra Leoneans and Liberians,” d’Harcourt said. “So we learned a lot more than we would have if we had had the meeting in New York or London.”