By: Amzath Fassassi
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
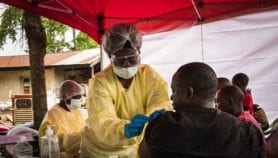
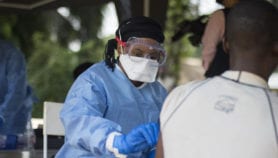
As the number of reported Ebola cases in the Democratic Republic of the Congo surpasses 1,000, efforts to respond to the outbreak continue to be hampered by violent conflict.
According to the Congolese Health Ministry on 24 March, 1,009 cases have been reported since the start of the outbreak in August 2018, of which 944 are confirmed. There have been 629 deaths, 564 of them confirmed as caused by Ebola, the rest probable.
The virus has been contained in 11 of the 28 areas affected, according to the World Health Organisation. However, Butembo and Katwa districts, in North Kivu province, remain hotbeds of contagion, with Katwa accounting for more than half of all new cases.
In an interview with SciDev.Net earlier this month, Congolese health minister Oly Ilunga Kalenga said restoring public trust was key to fighting Ebola, as he announced new research initiatives to tackle the disease.
Minister, when can we expect the Ebola outbreak in the DRC to come to an end?
Soon, I hope: the results we are getting in the field give us grounds for optimism. Look at the figures published by the Ministry of Health. You'll see that the groundwork is being done with patience and determination. All parties are contributing, from international response teams to local communities.
The pockets of resistance, where things are difficult, are areas where external factors unrelated to the outbreak itself are holding us back. Having said that, the government is now taking measures to deal with these issues in order to guarantee the security of patients and response teams.
International organisations contributing to the response say force has been used against communities to detrimental effect. What is the Congolese government doing to address this?
I don't share the view of the international organisations. I would like to make it clear that we are not forcing people to comply with public health directives. We have never used force to ensure compliance with sanitary measures.
The circumstances surrounding the outbreak are unprecedented: it is affecting areas controlled by around 100 armed groups in a part of the country where military operations are under way.
Providing security in this zone is a priority and this does not equate to militarising our response. If we want to put an end to the Ebola outbreak, we have to guarantee the security of patients and healthcare workers.
“If we want to put an end to the Ebola outbreak, we have to guarantee the security of patients and healthcare workers.”
Oly Ilunga Kalenga
Aid operations have also been hampered by what NGOs describe as local communities' lack of trust in international staff. What can be done to address the concerns of local people?
Context is key here. As you know, the outbreak is under control in 18 of the 20 areas that are affected. We have only been able to do that through being embedded in local communities.
This strategy has been proven to work across the country. What is different here is that the flare-up of inter-community violence in the Butembo district is undoubtedly linked to local actors.
To restore trust, we have to continue to engage with communities and deliver interventions alongside them, in order to successfully combat the outbreak.
There have been reports of unscrupulous individuals asking for sexual favours from local people in exchange for anti-Ebola therapy. Can you confirm this has happened?
To date, no cases of abuse or sexual exploitation have been brought to our attention. This allegation was made in the media following the publication of an article by The Guardian.
It's true that gender-based violence is a major social issue, but the Ministry of Health would like to make it clear that services related to Ebola are entirely free of charge. We've also put in place reporting mechanisms to avoid this sort of situation.
What, in the view of the Congolese government, are the main obstacles to bringing the outbreak to an end?
One of the main obstacles is the lack of engagement of community leaders. There have been attacks on response teams and Ebola treatment centres, but we noted that most local community leaders failed to speak up. Many fear becoming unpopular or are reluctant to commit themselves to supporting the response.
Some states bordering the DRC, Zambia notably, have taken measures to counter a possible spread of the outbreak to their territory. What is your assessment of the risk of a spread to other countries?
This risk has been present from day one. Since last August, we have been working with public health authorities in neighbouring countries. We regularly share information and are strengthening control points and entry points leading to other countries.
While authorities work to bring the current outbreak to an end, what is being done to put in place a strategy for dealing with future outbreaks?
I'm pleased to be able to announce that we have initiated a project to establish an Ebola Centre of Excellence, drawing on all of the DRC's experience in managing outbreaks of Ebola.
This centre will provide training to future generations and include a dedicated department for research; we are working to document all of the scientific advances made in the course of the outbreak.
The plan is to gradually transform this into a Centre for Disease Control, which will enhance the Ministry of Health's capacity to monitor outbreaks, identify public health threats, and formulate a response.
This piece was produced by SciDev.Net’s Sub-Saharan Africa French desk and edited for brevity