17/06/19
WHO under pressure over Ebola response

By: Ruth Douglas
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
The International Health Regulations (IHR) Emergency Committee met Friday in Geneva following the deaths from Ebola of a five-year-old boy and his grandmother in Uganda – the first confirmed cases of the virus in the East African country.
The outbreak which started in the DRC’s North Kivu province in August 2018 has claimed at least 1,346 lives and is the second largest in history.
“Declaring this a PHEIC would have raised the levels of international political support which has been lacking to date, enhanced diplomatic, public health, security and logistic efforts as well as released more financial resources to support the incredibly brave and committed teams working in North Kivu, DRC,”
Jeremy Farrar, director Wellcome
He added: “It was the view of the committee that there is really nothing to gain by declaring a PHEIC, but there is potentially a lot to lose.”
WHO director-general Tedros Adhanom Ghebreyesus said he accepted the committee’s decision but the outbreak remained “very much an emergency” for the families affected.
The WHO has been widely criticised for holding off on declaring the outbreak a PHEIC and effectively pulling the emergency chord to prompt international action. The committee had reached the same conclusions on two previous occasions.
Marianne Comparet, director of the UK-based International Society for Neglected Tropical Diseases, told SciDev.Net that, should the disease spread further, declaring a PHEIC would be “hugely beneficial in galvanising attention and resources as well as coordinating the response to this outbreak.”
What makes a PHEIC?
According to the WHO, the definition implies a situation is “serious, sudden, unusual or unexpected”, “carries implications for public health beyond the affected state’s national border”, and “may require immediate international action”.
“It was the view of the committee that the outbreak is a health emergency in DRC and the region but does not meet all the three criteria for a PHEIC under the IHR,” the WHO said in a statement. It advised against any travel of border restrictions, which a PHEIC would likely have prompted.
Jeremy Farrar, director of UK-based medical research charity Wellcome, said he respected the IHR’s decision but felt a PHEIC “would have been justified”.
“Declaring this a PHEIC would have raised the levels of international political support which has been lacking to date, enhanced diplomatic, public health, security and logistic efforts as well as released more financial resources to support the incredibly brave and committed teams working in North Kivu, DRC,” he said.
“A step up in the response with full international support is critical if we’re to bring the epidemic to an end and ensure protection for the communities at risk.”
Comparet stressed that she supported the IHR’s “rigorous assessment”, but said international attention must continue, given the cross-border spread of the outbreak.
“The international community can assist with supporting health systems with things such as improved diagnostics, increasing vaccine stockpiles, and an excellent and growing body of research on Ebola,” she said, adding: “Both countries affected shouldn't have to deal with this on their own."
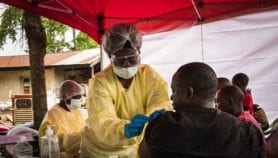
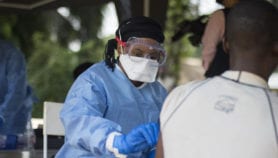
Ebola is a life-threatening illness that is spread through contact with the body fluids of an infected person, with symptoms including fever, fatigue and muscle pain.
The outcome of the last epidemic shows the urgency of preventative action. In 2014-2016, 11,000 people died in what became the world’s worst Ebola outbreak on record.
Gayle Smith, president and CEO of the ONE Campaign, a non-profit organisation which advocates to end extreme poverty and preventable disease, told SciDev.Net: “Although there have been extraordinary responses from NGOs, and the WHO is very focused on it, it’s striking that we’re missing the same urgency we saw with the 2014/5 Ebola outbreak in West Africa. Back then, the world collectively realised the scale of the situation and came together, this time it almost feels like it’s optional.”
Vaccine rollout
Uganda’s health ministry and the WHO announced the five-year-old as the first confirmed case of Ebola in the country last Tuesday (11 June).
A Congolese woman and her five-year-old grandson from Uganda both died from the virus, Uganda’s health ministry confirmed in a situation update Thursday, adding that the boy’s three-year-old brother had also tested positive and was being treated in hospital.Ugandan health minister Jane Ruth Aceng said authorities were “well prepared” for the new outbreak and had moved quickly to detect and isolate cases.