07/07/20
Can new polio vaccine avert nightmare of resurgence?
By: Aisling Irwin
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
The world is almost wild polio-free, but outbreaks of vaccine-derived polio could bring back the crippling disease.
One day this September — no one is quite sure when — a new vaccination campaign should spring into action. In eight African countries, health workers will mobilise to tackle outbreaks of a newly-emerged, and highly contagious, disease. This disease is like no other, however, because it has been caused by its own immunisation: it is vaccine-derived polio.
The global campaign to eradicate wild polio is facing a setback as this new form of the disease, caused by the virus strains used in polio vaccines regaining their virulence, has emerged. Vaccine-derived polio viruses have been seen in more than 20 countries since 2000 and officials, funders, academics and health workers are racing to stamp them out.
Now, they have a promising tool — a new vaccine that is more stable. But, can it succeed, or does the problem with polio run deeper than any technology can tackle?
Polio battle
More than US$16 billion has been spent on wild polio eradication since the Global Polio Eradication Initiative (GPEI) was set up in 1988. Wild polio is now almost vanquished, lingering in just Afghanistan and Pakistan, and possibly Nigeria.
“There is a sense of exhaustion in the eradication campaign. People have been working on this for 33 years … Now you have a new tool and that can energise the campaign.”
Raul Andino, virologist, University of California, San Francisco
In 2016 the GPEI recorded just 42 paralytic cases, compared with about 350,000 a year in the 1980s. Polio mainly affects children and can lead to permanent paralysis or death.
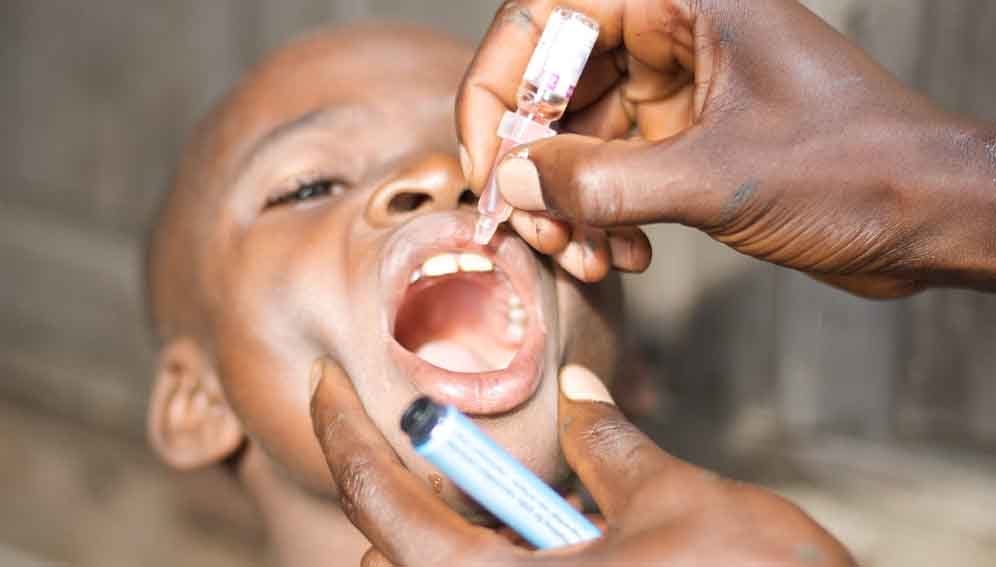
At the heart of this success lie three oral polio vaccines, one for each viral strain. These are live viruses that have been attenuated — made weaker — to become harmless when administered and they have always carried the tiny risk that they could evolve and regain their virulence.
Such mutations were occasionally spotted since 2000, but they died off without infecting anyone, thanks to the immunity conferred by the vaccination programmes.
In 2015, however, things changed. Six years had passed since the last confirmed case of wild polio virus type 2. A global polio commission declared it eradicated and the correlating vaccine was withdrawn, to allay concerns about introducing the virus into populations when it did not exist in the wild (vaccination for types 1 and 3 continued).
New strains emerge
Quickly, however, vaccine-derived cases started to emerge; about 85 cases by 2017, almost 370 by 2019, and 210 cases so far this year — more than three times the number at the same time last year. Four World Health Organization regions are affected, with Africa recording the highest number of cases.
“What we now have is no kids have been vaccinated in routine [type 2] immunisation since 2015 so with all these new births, millions of people essentially have no immunity, and that’s why we’re very concerned,” O’Reilly says.
Precisely how it happened is unclear — the mutated virus may have jumped through gaps in routine immunisation campaigns, or some campaigns may have continued to use the type 2 oral vaccine after the cut-off date, speculates Michel Zaffran, who directs polio eradication for the WHO.
Whenever an outbreak of vaccine-derived type 2 polio is detected, health workers swoop in with a targeted vaccination campaign. But each time the previously-withdrawn oral vaccine is used, there is the risk of releasing a new infectious mutation, which could spread beyond the boundaries of the intervention into unvaccinated communities.
Nevertheless, says Pascal Mkanda, who coordinates WHO’s Africa polio eradication programme from Brazzaville, Congo, these swoops had been fairly successful — until the arrival of the COVID-19 pandemic. Restrictions this year have prevented spot campaigns aimed at 14 million children in Africa, though routine polio immunisations have continued.
The worst fear, says Andrew Macadam of the UK’s National Institute for Biological Standards and Control, is that spot campaigns will be delayed by a “prolonged period”, in which case “type 2 will probably establish itself as an endemic virus in parts of Africa”. Endemic diseases are those that remain present in a population, with outbreaks continuing to occur.
“Months is bad, so a year would be very bad,” Macadam says.
Vaccine type 2, take two
This is why there is excitement about the type 2 novel oral polio vaccine — nOPV2, a modified version of the existing mOPV2 — the fruit of nearly a decade of work by a partnership of researchers with a non-profit and a pharmaceutical company to design flaws into the attenuated virus, so that it cannot evolve.
The project is unparalleled, say Macadam and fellow consortium member Raul Andino, a virologist at the University of California, San Francisco, because it has been one seamless endeavour from concept to field deployment. It is also the first time, says Macadam, that scientists have “rationally” designed a live attenuated virus vaccine. Altered versions of types 1 and 3 are on their way.
The vaccine has raced through human trials in Belgium and Panama. The Indonesian drug firm Bio Farma, in Bandung, is already manufacturing tens of millions of doses. Deployment could start in September, says Mkanda, but only if the WHO grants it Emergency Use Listing in advance of the usual licencing processes.
Mkanda says staff are preparing for “a big assault” once COVID-19 has diminished. “I’m hopeful that we’ll really be able to bring the thing to a halt,” he says.
He is working with national governments, each of which needs to acquaint itself “exhaustively” with the data and consent to be in the first “emergency use” wave. Countries can only participate in this if they have not used the old type 2 vaccine in the last three months, for monitoring reasons. This is why some of those worst-affected by vaccine-derived polio — Angola, Central African Republic, Democratic Republic of Congo — are not included.
Instead, Mkanda is hoping eight countries will agree: Burkina Faso, Cameroon, Cote d’Ivoire, Chad, Mali, Ethiopia, Congo and South Sudan.
Dealing with this setback has increased an already extraordinary price tag. Polio eradication funding for 2021 is $950 million, which includes $110 million for responding to vaccine-derived outbreaks. But it does not include $360 million for supplying the novel vaccine for the next three years.
Securing the money is “a major challenge,” says Zaffran. “The donors have been extremely generous but the continuation of the efforts and the current economic situation is putting us in a very challenging environment.”
True eradication
Polio was supposed to be eradicated by 2000 — the goal set by the GPEI. Will the suite of novel oral vaccines finally mean victory?
Last year, a global group of academics argued in the British Medical Journal that polio will likely never be eradicated because of the perennial problems of hard-to-access conflict zones and community acceptance, as well as secondary, vaccine-derived epidemics. One author, Oliver Razum, of Bielefeld University in Germany, tells SciDev.Net the novel vaccine “is highly unlikely to be a game changer” because “technology does not resolve the socio-political constraints of polio eradication”.
Mkanda disagrees. He points out that Africa will have had no new cases of wild polio for four years in August — when an independent commission is expected to declare the region wild polio-free. Such eradications are “a massive achievement — to have completely broken the transmission networks for all three wild type polio viruses”, says Macadam. “So, it’s clearly doable.”
But vaccine-derived polio poses new problems, he says. “If you had 100 per cent coverage you wouldn’t get vaccine-derived outbreaks because herd immunity would prevent it,” Macadam says. “That’s never going to happen, particularly where there is no [polio] disease, because developing countries have other health issues. So why would they spend their time controlling a disease that doesn’t exist?“So, we shall see whether the new [vaccine] strains will … control outbreaks and stop them reoccurring. We’re very confident that they will be much better than the current strains.”
Andino believes the new vaccine will bring another advantage: “There is a sense of exhaustion in the eradication campaign. People have been working on this for 33 years … Now you have a new tool and that can energise the campaign.”













