By: Fatima Arkin
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
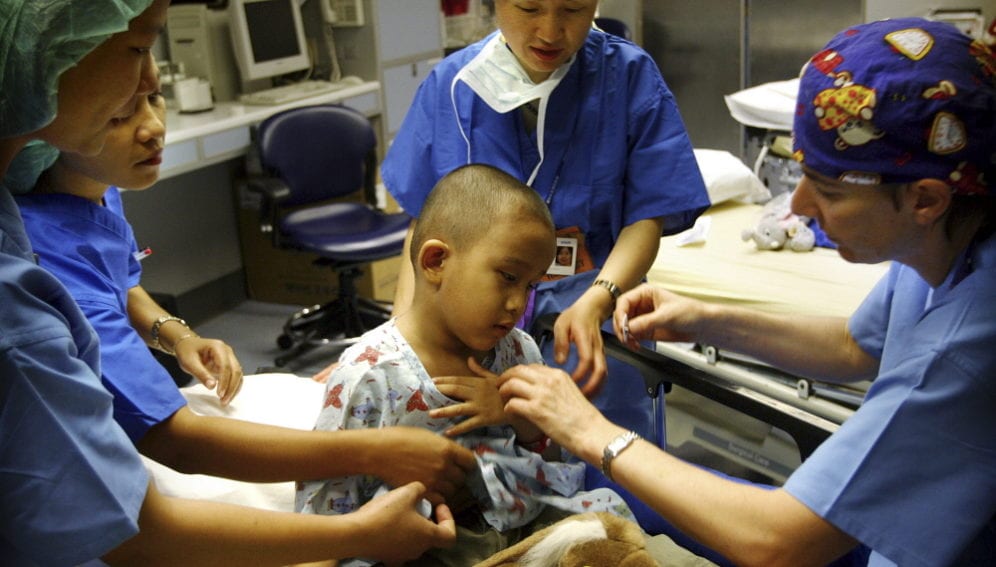
[MANILA] The government-owned Philippine Health Insurance Corporation (PhilHealth) is claiming a dramatic surge in membership to over 80 per cent of the population, up from 38 per cent in 2000, putting the country closer to achieving its target of universal health coverage for all.
While these figures have been hotly contested by NGOs and other organisations such as the Philippine Medical Association and the Health Alliance for Democracy, Manuel Dayrit, a former health secretary and the dean of public health and medicine at the Ateneo de Manila University, tells SciDev.Net there is a general sense that PhilHealth coverage is rising.
But the question is, how will the health insurance firm contain the costs and remain in the black?
PhilHealth is currently using a case rate payment system that offers hospitals a fixed fee for each treatment. But it is looking at adding a ‘pay-for-performance’ (P4P) model that rewards healthcare providers — physicians, hospitals and medical groups — for meeting certain quality standards.
“With the introduction of case rates, we need to develop a new system as it changes the dynamic between PhilHealth and how we pay our providers,” John Basa, senior vice president of PhilHealth, tells SciDev.net. “Since we are studying to move towards D.R.G.s [diagnosis-related group system of fixed reimbursement to hospitals], a bonus system can be integrated to reflect a P4P mechanism.”
A major study conducted in 2003 in the central Philippines documented “exceptional outcomes” for P4P. Biannual surveys of 30 public hospitals compared P4P with universal health coverage for children under six years old and below the poverty line. Quality of care was determined using written case studies focused on diarrhoea and pneumonia, which are common among children.
John Peabody, one of the authors of the study and president of QURE Healthcare, tells SciDev.Net that both P4P and universal healthcare coverage worked equally well, but P4P is cheaper to implement (US$13,000 per district per year under P4P compared to US$80,000 in the universal coverage).
“Not only did this experiment work, but once the improvements were made in the quality of care, they persisted,” says Peabody. “We went back seven years later and there was still a big effect.”
Still, several studies highlight the failures of P4P in healthcare. A six-year study published in the New England Journal of Medicine in 2012 looked at 30-day mortality in United States hospitals using the P4P programme compared with over 3,000 hospitals that were not using a P4P model.
The results showed that 30-day mortality — the rate at which people died within a month after availing of a treatment — was comparable between the two groups. The drop in mortality rate over the next six years was also similar.
Additionally, the conditions that were intentionally tied to incentives yielded no improvements when compared with conditions that did not use P4Ps. In the Philippines, P4Ps have already been implemented, including in the field of maternal health. But just how widely the intervention is practised remains unclear.
This article has been produced by SciDev.Net's South-East Asia & Pacific desk.