02/06/21
Canine coronavirus strain found in humans

By: Melanie Sison
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[MANILA] Several pneumonia patients in Malaysia’s Sarawak state have tested positive for a coronavirus strain associated with dogs, according to a study.
Genome sequencing of the coronavirus identified it as a novel canine-feline recombinant alphacoronavirus, which was named CCoV-HuPn-2018. The study, published May in Clinical Infectious Diseases, says it is the first to report this type of coronavirus being detected in a human pneumonia patient.
CCoV-HuPn-2018, if confirmed as a pathogen, may be the eighth unique coronavirus that can make humans ill.
Coronaviruses already known to infect humans include SARS-CoV-1, known to cause Severe Acute Respiratory Syndrome (SARS), an outbreak of which occurred in 2002— 2004; MERS-CoV, which causes the Middle East respiratory syndrome, first detected in 2012, and SARS-CoV-2, which causes COVID-19.
All these diseases are zoonotic, meaning they can jump from animals to humans. SARS-CoV-1 is suspected to have jumped to humans from bats or civets, MERS-CoV from camels and SARS-CoV-2 from bats or minks.
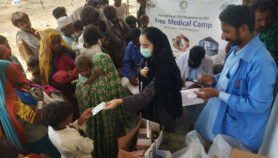
Samples taken in 2017— 2018 from eight of 301 hospitalised patients tested positive for the CCoV-HuPn-2018 coronavirus strain. Of these eight patients, seven were less than five years old, lived in rural areas and were frequently exposed to animals, both wild and domesticated. Most belonged to one of several indigenous ethnic groups in Sarawak. All patients recovered after four to six days in hospital.
There are various unknowns about the virus at this stage, says Gregory Gray, an author of the study and infectious diseases professor at the Global Health Institute, Duke University, US. These include how domesticated animals such as dogs and cats can get infected with a coronavirus strain, how they can infect humans, and whether human-to-human transmission is possible.
According to Gray, what is important is that these coronaviruses may be spilling over to humans from animals much more frequently than is known. “We are proposing future epidemiological studies to answer such questions,” Gray tells SciDev.Net.
“Our findings underscore the public health threat of animal coronaviruses and a need to conduct better surveillance for them,” the researchers wrote in the study. Coronaviruses are a group of viruses that have crown-like spikes on their surface.
In a press release issued by Duke University, Gray emphasised the importance of using diagnostic tools to enable early detection to arrest the spread of infections. “These pathogens don’t just cause a pandemic overnight. It takes many years for them to adapt to the human immune system and cause infection, and then to become efficient in human-to-human transmission. We need to look for these pathogens and detect them early.”
The research team used a powerful molecular diagnostic tool, which can detect most coronaviruses, including currently unknown ones. Gray tells SciDev.Net that they have already “published the methods and diagnostic companies may develop commercial kits”.
Keith Hamilton, head of the Preparedness and Resilience Department at the World Organisation for Animal Health (OIE), agrees that innovations have made it easier for scientists to detect viruses. “Major advancements in detection and analytical technologies over the past couple of decades are allowing scientists to detect, characterise and track viruses much more easily,” he says.
However, Hamilton notes that the study is inconclusive. “The finding of genetic material belonging to this virus in the nasopharyngeal swabs of the patients does not in itself prove that infection with this virus caused the pneumonia. Additionally, the paper does not present any evidence for human-to-human transmission.”
He also tells SciDev.Net that there is a difference between CCoV-HuPn-2018 and the coronaviruses that caused SARS, MERS, and COVID-19. “SARS-CoV-2, MERS and SARS belong to the genera of betacoronaviruses, whilst the virus discussed in the study appears to be a member of the genera alphacoronaviruses, so it is not closely related to MERS, SARS or SARS-CoV-2.”
“SARS-CoV-2, MERS and SARS belong to the genera of betacoronaviruses, whilst the virus discussed in the study appears to be a member of the genera alphacoronaviruses, so it is not closely related to MERS, SARS or SARS-CoV-2”
Keith Hamilton, World Organisation for Animal Health
Nonetheless, Hamilton says that studies such as this can help provide a clearer picture of the relationship between coronaviruses and hosts, along with environmental factors that can affect this interaction. “Such findings do highlight the potential value of surveillance and research to better understand the behaviour of coronaviruses at the human-animal-environmental interface.”
Sarah Caddy, veterinarian and viral immunologist at the University of Cambridge, tells SciDev.Net: “This research cannot conclusively show the source of human infections, but it is likely to be dogs.”
Caddy says there is no evidence of the canine coronavirus spreading. “There are several infections that can pass between dogs and humans, but generally these are rare,” she says. “Following good hygiene around our pets, e.g. washing hands after patting, is always a good idea regardless.”
This piece was produced by SciDev.Net’s Asia & Pacific desk.