By: Joel Adriano
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
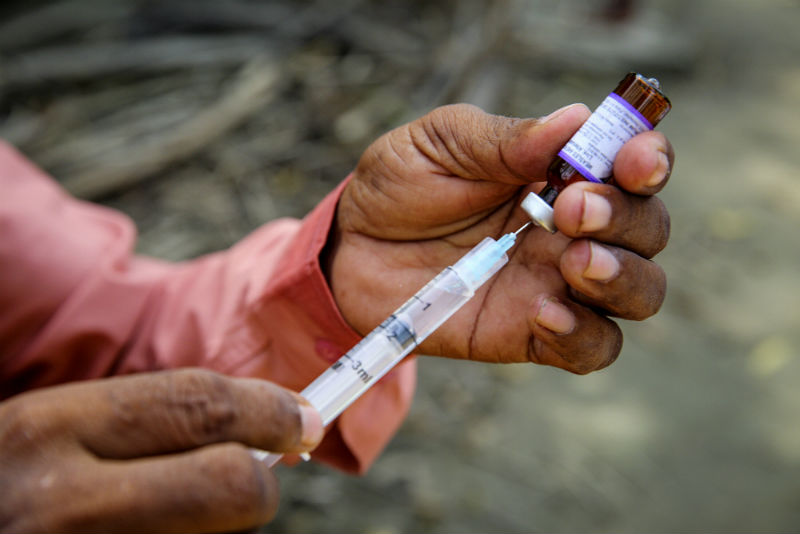
[MANILA] Should countries start vaccinating its citizens against dengue?
This is a dilemma countries with huge dengue cases have to grapple with while weighing the use of Dengvaxia, the world’s first approved dengue vaccine. The vaccine is 65.6 per cent effective against dengue, says Su-Peing Ng, global medical director of Sanofi Pasteur which produces the new vaccine.
In April, the Philippines became the first country to roll out Dengvaxia while Brazil launched a similar one last month. Indonesia is also reportedly considering mass vaccinations along with the Latin American countries of Costa Rica, El Salvador, Guatemala, Mexico, Paraguay and Peru.
Should you wait [for a better drug] at the expense of people’s lives?
Tikki Pang, Lee Kuan Yew School of Public Policy
But after vaccinating almost half a million school-age children, Philippine health officials under the administration of newly installed president Rodrigo Duterte halted the dengue vaccination programme and proposed a review over fears that the vaccine could cause side effects. Some local doctors also advised to wait for other countries to try out the vaccine first or wait for a better drug to come in.
Tikki Pang, former WHO director for research policy and a professor at the Lee Kuan Yew School of Public Policy of the National University of Singapore, says two other drug firms are close to coming up with dengue vaccines though it will probably take two or three years before these become available. He also thinks their efficacy wouldn’t be significantly different from Dengvaxia.
About 390 million people in over 100 countries are affected by dengue each year. He says while deaths in terms of percentage isn’t quite high, over 12,000 people dying each year from dengue are still too many.
“Should you wait [for a better drug] at the expense of people’s lives?” he asks. “The current vaccine might not be perfect but it’s the best we have at the moment. Moreover, it doesn’t prevent countries from shifting to a better vaccine later on once this becomes available.”
What is critical, he says, is for decision makers to determine the extent of the problem as it might be too costly to implement mass vaccination, and to consider independent scientific evidence.
Interestingly, Ng declined to reveal the cost of the Dengvaxia vaccine, which isn’t readily available outside of government-sponsored vaccination programmes. One can only guess that the vaccine doesn’t come cheap — which raises the question if poor countries can afford it.
Another suggestion Pang makes is tier pricing where drugs are sold higher in rich countries to subsidise prices in poorer ones like what’s happening with hepatitis B and typhoid vaccines.
This piece was produced by SciDev.Net’s South-East Asia & Pacific desk.