By: Brendon Lee
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
[KUALA LUMPUR] South-East Asia could be the catalyst of a malaria pandemic if drug-resistant malaria parasites are not brought under control, researchers warn.
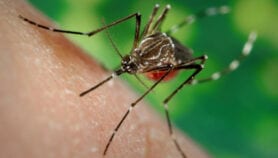
A new study published in The New England Journal of Medicine (31 July) revealed that malaria parasites discovered in the malaria-critical regions of Cambodia, Thailand and Vietnam displayed resistance to artemisinin, currently the most effective drug against the mosquito-borne disease.
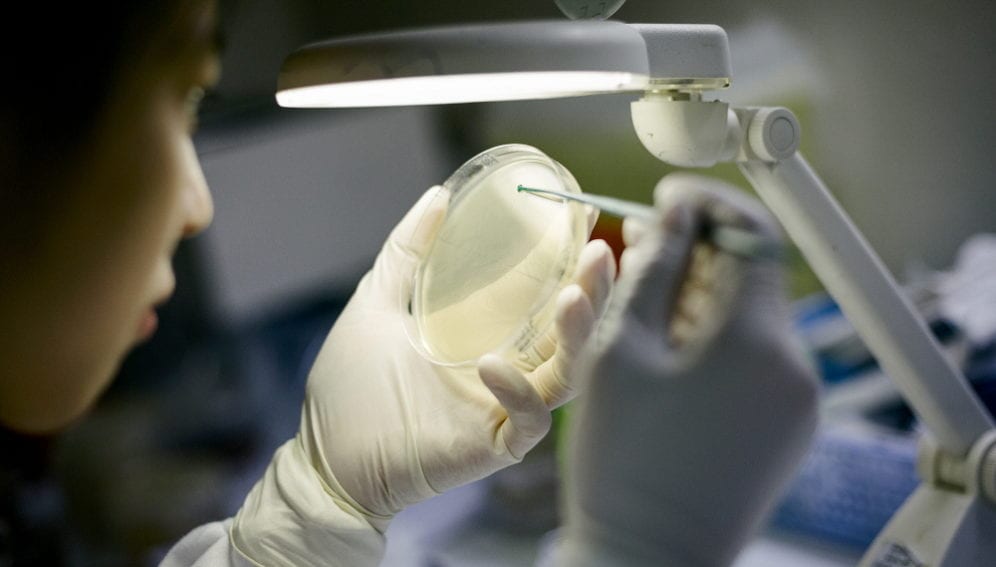
The study, which analysed blood samples from 1,241 malaria patients in 10 countries across Asia and Africa, has shown that Plasmodium falciparum, the parasite species responsible for the most common form of malaria, had developed resistance to artemisinin-based drugs and required extended treatment period and dosage.
Counterfeit or substandard anti-malarial drugs, and the unregulated use of artemisinin alone instead as part of a combination treatment, are some of the factors resulting in drug-resistant malaria parasites.
“The lack of regulation of antimalarial drug manufacture and prescription worldwide needs to be addressed. This could be particularly important in the not too distant future in African countries where numerous artemisinin-based combination therapies of variable quality are freely available,” according to the study’s lead author Elizabeth Ashley.
“One of the biggest challenges is that resistance always starts in South-East Asia where young working men in forested areas are most at risk,” Ashley noted.
Standard antimalaria treatment often last for three days but the new mutated strain of P. falciparum (identified as the kelch 13 gene) requires treatment to be extended to six days. However, experts warn that this is only a temporary solution.
One trait of the mutated P. falciparum strain is that it has a higher chance of remaining in its host body after treatment. Hence, patients with slow-clearing infections are more likely to infect mosquitoes even though they do not display any symptoms of the disease.
According to the study, this is not the first time that malaria parasites have developed resistance to frontline drugs. Before artemisinin, chloroquine and sulphadoxine-pyrimethamine were used from the 1950s to the 1970s to suppress the parasite before it evolved and developed resistance.
“When there is drug pressure on a parasite or a bacterium, the weaker strains get killed while mutations develop in some that survive. Prolonged exposure to lower levels of the drug can lead to emergence of drug resistance. But the exact mechanism is really unknown,” explains Balbir Singh, director of the Malaria Research Centre at Universiti Malaysia Sarawak.
Currently, new antimalarial medicines are being developed but these still require several years of testing before they can be distributed worldwide. Experts recommend reinforcing standard control measures and improving availability of early diagnosis and treatment with effective drugs.
Link to full paper in The New England Journal of Medicine
This article has been produced by SciDev.Net's South-East Asia & Pacific desk.
References
The New England Journal of Medicine doi: 10.1056/NEJMoa1314981 (2014)