By: Prime Sarmiento
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
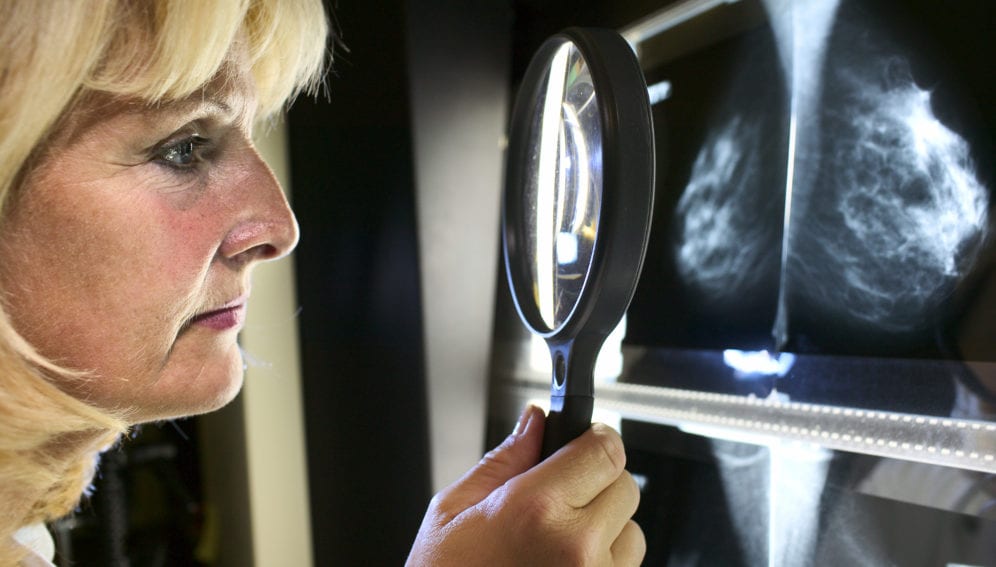
[MANILA] Singapore-based researchers have discovered a unique biomarker which, they say, can help predict breast cancer relapse and thereby reduce mortality incidence of one of the world’s most common cancers.
A team led by the Genome Institute of Singapore (GIS), Tan Tock Seng Hospital and National University Health System used integrative genomics to analyse tumour samples from 200 breast cancer patients in Denmark, Singapore and US. This helped them identify a biomarker strongly associated with breast cancer relapse and develop a blood-based diagnostic test kit.
“We conducted this study to find a unique biomarker for the aggressive tumour-initiating cells which is responsible for relapse in cancer patients”
Qiang Yu, Genome Institute of Singapore
According to the study’s findings, published in September in Nature Medicine, the biomarker was found in more than 70 per cent of recurrent tumours. Early-stage patients who tested positive for this biomarker on diagnosis are nearly 40 times more likely to develop a relapse within five years than patients who tested negative, according to the study.
“We conducted this study to find a unique biomarker for the aggressive tumour-initiating cells which is responsible for relapse in cancer patients,” says Qiang Yu, researcher at GIS and corresponding author. “Through our integrated genomic analysis, we found a genomic alteration which can also be exploited to develop a non-invasive liquid biopsy assay for monitoring breast cancer patients.”
The blood-based DNA test and technology developed by the team can be used to identify patients with high-risk relapse, monitor for tumour relapse after surgery (preliminary results show that it is more sensitive than conventional radiological imaging) and can be developed as a companion diagnostic to develop drugs which can effectively target aggressive cancer cells, says Yu.
Several studies have shown that breast cancer is one of the top causes of death among women in emerging economies. For instance, a study done by health science researchers from Iran noted that the high cost of breast cancer surgery, radiation and chemotherapy, has increased mortality incidence in developing countries.
In a research article published 2016 at the Asian Pacific Journal of Cancer Prevention, the researchers said “women in low-income countries, especially in Africa, seek treatment in advanced stages of disease, when it has spread to other organs. In England and Australia, very few women are diagnosed in third and fourth stages of disease. In Kenya and Uganda, almost all women are diagnosed late and are associated with higher mortality.”
Roel Tolentino, surgical oncologist at St. Luke’s Medical Centre and former president of the Philippine Society of Oncology, said that while the findings and technology can help breast cancer patients, its affordability will determine if this will gain traction among women with breast cancer in developing countries emphasising “that limited financial resources is one of top reasons why most people don’t seek early diagnosis and treatment for breast cancer.”But according to Yu, the blood-based DNA test is especially helpful for breast cancer patients in developing countries as it is more convenient and affordable than tissue biopsy and radiological imaging although he admitted that the findings need further clinical validation and commercial development.
“We want to conduct a prospective clinical study to further validate the biomarker and its application as a liquid biopsy test. We are also looking for an opportunity to develop and commercialise the assay so that it is readily available for patients and hospitals,” says Yu.
This piece was produced by SciDev.Net’s Asia & Pacific desk.