28/02/20
Polio eradication calls for both shots and drops
Send to a friend
The details you provide on this page will not be used to send unsolicited email, and will not be sold to a 3rd party. See privacy policy.
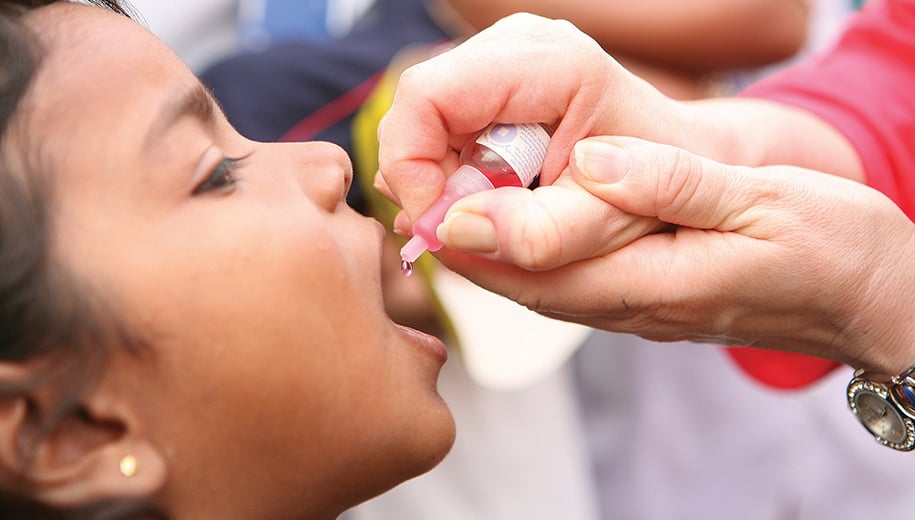
[NEW DELHI] India, which became polio-free in 2014 by using oral polio vaccine (OPV) drops, must shore up the success with injectable, inactivated polio vaccine (IPV) or face the possibility of resurgence, experts say.
Particularly worrying are circulating vaccine-derived polioviruses (cVDPV) — mutants of the strains used in making oral polio vaccine — which caused 227 polio cases in 2019, with 198 occurring in countries non-endemic for polio, according to the Global Polio Eradication Initiative (GPEI). That’s compared to the 116 cases of polio caused by the wild-type poliovirus, all of them in the last endemic countries of Afghanistan, Nigeria and Pakistan.
Given a chance to circulate from child-to-child, especially in areas with low immunisation levels, oral vaccine viruses can regain strength from their artificially weakened or attenuated condition and cause paralysis. The longer a vaccine virus exists in the environment, the greater the chances of it mutating into cVDPV.
Michel Zaffran, who leads GPEI, says that paralysis caused by cVDPV presents in the same way as paralysis caused by wild-polio viruses.
“Polio is a highly infectious disease and the risk is that it can always return even in polio-free countries unless it is completely eradicated,” says Zaffran. “Modelling suggests that if we abandon the eradication effort, polio will resurge globally and, within ten years, we would again see 200,000 new cases, every single year, all over the world,” he tells SciDev.Net.
Oral polio vaccination campaigns are conducted every year to maintain population (pre-school age) immunity, says T. Jacob John, emeritus professor of virology, Christian Medical College, Vellore, India.
“The publicised reason is to protect against risk of importation of poliovirus from neighbouring Pakistan or Afghanistan,” John says. “But the real reason is that if population immunity from the vaccine decreases, the vaccine virus can begin spreading, leading to cVDPV.”
“Polio is a highly infectious disease and the risk is that it can always return even in polio-free countries unless it is completely eradicated… Modelling suggests that if we abandon the eradication effort, polio will resurge globally and, within ten years, we would again see 200,000 new cases, every single year, all over the world”
Michel Zaffran, Global Polio Eradication Initiative
The answer to cVDPV is to fully include inactivated polio vaccine in the vaccination schedule he emphasised. “We have written [to the government] requesting full immunising schedule with IPV. Currently, only two intradermal fractional doses are given. That is equivalent to one full intramuscular dose. Perfect for priming but for long term at least one booster dose is needed.”
Inactivated polio vaccine, which is produced from wild-type poliovirus strains of each serotype that have been inactivated (killed) with formalin, provides immunity against all three types of polioviruses and has only mild or temporary side effects, says a WHO newsletter. However, IPV production carries risks as it involves handling large quantities of live poliovirus that require strict safety measures and containment.
Joel Calmet, former communications director at Sanofi Pasteur, a major manufacturer of both OPV and IPV, tells SciDev.Net that there is every chance of vaccine-derived polio cases increasing. “This situation of the secondary infection is very complex. When you stop vaccinating you create the exact conditions where you have this kind of resurgence.”
As India moved into a second phase — or ‘end game’ as WHO calls it — to eradicate vaccine-derived viruses, it became important to introduce full IPV coverage.
India has continued to conduct mass vaccination campaigns using bivalent (types 1 and 3) oral polio vaccine to maintain high levels of immunity in the population.
“As long as wild virus types 1 and 3 are persistent in Afghanistan, Nigeria and Pakistan, we will use bivalent OPV and, eventually, we will withdraw that also,” says John. “Actually, wild virus type 3 has not been seen for two years but we will have to wait for three full years before we assume that it has been eradicated.”
In 2018, type 2 polio vaccine viruses were discovered in sewage and stool samples and traced to supplies of trivalent OPV that was fully phased out in India in April 2016. However, India’s health ministry assured that the discovery of type 2 polio vaccine virus indicated “very robust polio surveillance” that it manages with WHO support.
Apart from cVDPV, India needs to be vigilant against Vaccine Associated Polio Viruses (VAPP), which are generated when the live attenuated virus in the Oral Polio Vaccine regains and causes what is called Non-Polio Acute Flaccid Paralysis (AFP). “VAPP is continuing to occur, but the government classifies it as non-polio AFP,” says John.
According to a WHO fact sheet, the risks from VAPP are small and confined to individual vaccine recipients and their close contacts.
The current (2019—2023) endgame strategy aims to eradicate polio by first interrupting circulation of all wild polio virus and then stopping all cVDPV outbreaks within 120 days of detection. That is to be followed by strengthening immunisation and health systems with continued sensitive surveillance.
However, outbreaks in 2019 of the type-2 vaccine-derived poliovirus (cVDPV2) in Africa and other areas called for a new strategy, prompting accelerated development and licensing of novel OPV2 (nOPV2) vaccine.
“WHO and partners are working on introducing nOPV2 later this year — this vaccine will have a much lower risk of cVDPV and could be used in areas for supplementary immunisation where cVDPV2 cases are occurring. Further, high coverage with IPV will provide the immunity needed to curtail occurrence of these cases,” Swaminathan said.
“There is a great need to strengthen routine immunisation systems in all countries and wherever outbreaks of cVDPV2 cases have occurred, there has been an issue with coverage. Surveillance is also key — an area where India has done well as there were no reports from India on either clinical or environmental samples being positive in 2019.”
This piece was produced by SciDev.Net’s Asia & Pacific desk.